- Medical Aid
- Currently Trending
The Best Medical Aids
- Compare Plans
- Gap Cover
- Best Gap Covers
- Hospital Plans
- Currently Trending
The Best Hospital Plans
- Medical Insurance
- Pet Insurance
Sizwe Hosmed Plus Medical Aid Plan
Overall, the Sizwe Hosmed Plus Medical Aid Plan is a trustworthy and comprehensive medical aid plan that offers 24/7 medical emergency assistance and access to extra preventative care tests for up to 3 Family Members. The Sizwe Hosmed Plus Medical Aid Plan starts from R7,227 ZAR.

Sizwe Hosmed Plus Plan – 7 Key Point Quick Overview
- ☑️ Sizwe Hosmed Plus Plan Overview
- ☑️ Sizwe Hosmed Plus Plan Contributions
- ☑️ Plus Plan Benefits and Cover Comprehensive Breakdown
- ☑️ Plus Plan Exclusions and Waiting Periods
- ☑️ Sizwe Hosmed Plus Plan vs. Similar Plans from other Medical Schemes
- ☑️ Our Verdict on The Plus Plan
- ☑️ Plus Plan Frequently Asked Questions
Sizwe Hosmed Plus Plan Overview
The Sizwe Hosmed Plus medical aid plan is one of 12, starting from R7,227 and includes additional non-PMB conditions, extra preventative care tests, vaccination benefits for COVID-19, HPV, Flu, and more. Gap Cover is not available on the Sizwe Hosmed Plus Plan. However, Sizwe Hosmed offers 24/7 medical emergency assistance. According to the Trust Index, Sizwe Hosmed has a trust rating of 3.9.
Sizwe Hosmed offers 12 medical aid plans
- ✅ Sizwe Hosmed Value Core
- ✅ Sizwe Hosmed Titanium Executive
- ✅ Sizwe Hosmed Silver Hospital
- ✅ Sizwe Hosmed Plus
- ✅ Sizwe Hosmed Platinum Enhanced
- ✅ Sizwe Hosmed Platinum Enhanced EDO
- ✅ Sizwe Hosmed Gold Ascend
- ✅ Sizwe Hosmed Gold Ascend EDO
- ✅ Sizwe Hosmed Value
- ✅ Sizwe Hosmed Essential Copper
- ✅ Sizwe Hosmed Access Saver 25
- ✅ Sizwe Hosmed Access Core
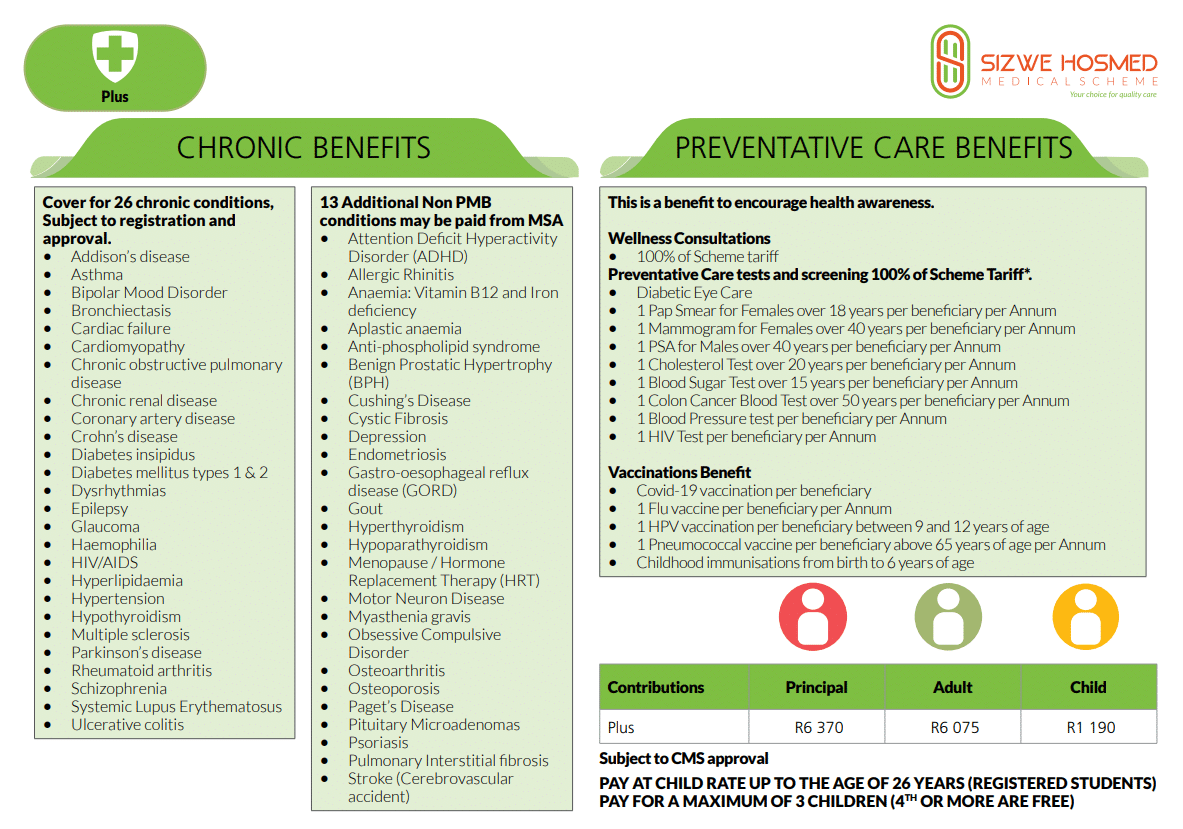
Sizwe Hosmed Plus Plan Contributions
| 👤 Main Member | 👥 Adult Dependent | 🍼 Child Dependent |
| R7,227 | R6,893 | R1,577 |
Plus Plan Benefits and Cover Comprehensive Breakdown
Plus In-Hospital Benefits
- ️ Hospital admissions
- Unlimited benefits for Specified Minimum Benefit circumstances.
- Hospital admissions—including PMBs—require pre-authorization and case management.
- Emergency admissions require 48-hour notification of the Scheme.
- Claims will be denied if admissions are not pre-authorized or reported within 48 hours.
- Plus hospital benefits are only available to Authorized Service Providers.
- There is a 10% co-payment for non-DSP hospital use.
- ️ In-hospital General Practitioner and Specialist services
- PMB and case management protocols apply.
- All procedures must be approved in advance.
Failing to pre-authorize or notify the scheme of admission within 48 hours will result in claim payments being withheld.
| 🔎 Hospital Admissions High Care Unit General Ward Theatre Recovery Room | Covered up to 100% of the Negotiated Tariff. |
| 📌 Medicines and consumables used in hospital and theatre | Covered up to 100% of the negotiated tariff. |
| 📍 Medicine to take home after discharge | Paid from the hospital benefit. Limited to 7 days’ medicine. |
| ☑️ Consultations and Procedures | Covered up to 200% of the negotiated tariff. |
| ✅ Basic Radiology and Pathology | Covered up to 100% of the scheme tariff. |
| 🟥 Specialized Radiology | Limited to two scans per beneficiary yearly. There is a 10% co-payment for non-PMB MRI and CT scans. |
| 🟧 Oncology | Covered up to 100% of the DSP tariff. Enhanced oncology DSP protocols will apply. Unlimited Oncology treatment is available for PMB. Benefits over R679,500 are subject to a 20% co-payment on non-PMBs. |
| 🟨 Renal Dialysis | Covered up to 100% of the negotiated tariff. |
| 🟩 Organ Transplants | Covered up to 100% of the scheme tariff. |
| 🟦 Dental Hospitalisation | Covered up to 100% of the scheme tariff. Children under seven can receive general anesthesia benefits once per year for intensive dental treatment. Symptomatic wisdom tooth removal is covered solely as Day Case. Subject to pre-approval. Treatment protocols will apply. |
| 🟪 Maxillo-facial and Oral Surgery | Covered up to 100% of the scheme tariff. Subject to managed care protocols. Only symptomatic wisdom teeth and surgical exposure are allowed. All other operations are subject to PMB approval alone. Only symptomatic impacted wisdom teeth are removed on a day-to-day basis. |
| 💊 Drug and Alcohol Rehabilitation | Covered up to 100% of the scheme tariff. Limited to R21,457 per family per year. |
| 🧠 Psychiatric Treatment (PMB) Consultations Ward Fees Medicines Psychiatry/psychology therapy sessions | Covered up to 100% of the scheme tariff. 21 in-patient days or up to 15 outpatient interactions per year per beneficiary Fourteen days per family with a maximum of R25,195. |
| ➡️ Non-PMB Psychiatric Treatment | Up to 3 days for the Psychologist for combined therapy sessions with the Psychiatrist at the same admission. After that, pre-authorization with the treatment plan is required. |
| ⬇️ Step-down Facilities | Covered up to 100% of the negotiated tariff. Limited to 14 days per beneficiary per year. |
| 🏡 Home-Based Care | Covered up to 100% of the negotiated tariff. Limited to 14 days per beneficiary per year. |
| 🩹 Negative Pressure Wound Therapy | Covered up to 100% of the negotiated tariff. Limited to R29,657 per family per year. |
| 😮💨 Hyperbaric Oxygen Therapy | Covered up to 100% of the negotiated tariff. Limited to R53,695 per family per year. |
| 🅰️ Male Sterilisation/Vasectomy | Covered up to 100% of the negotiated tariff. Sterilization is limited to R17,472 per beneficiary per year. Subject to pre-approval and PMBs. |
| 🅱️ Female Sterilisation/Tubal Ligation | Covered up to 100% of the negotiated tariff. Sterilization is limited to R17,472 per beneficiary per year. Subject to pre-approval and PMBs. |
| 📈 Back and Neck Surgery | Spinal surgery authorization for treating chronic back or neck pain is subject to managed care guidelines. Before authorizing surgery, managed care may require adherence to conservative clinical treatment. |
| 📉 Stereotactic Radiosurgery | Covered up to 100% of the scheme tariff. Only covers Primary Central Nervous System tumors. |
| 📊 Age-related Muscular Degeneration Treatment | Covered up to 100% of the negotiated tariff. Pre-authorization required. |
| 🔍 Laparoscopic Hospitalisation and Associated Costs | Pre-authorization required. Subject to PMBs. |
| ✔️ PMB Laparoscopic Procedures | PMBs are covered in DSP facilities. Subject to clinical protocols. In-hospital procedures will incur an R5,250 co-payment, except for diagnostic laparoscopy, aspiration/excision ovarian cyst, lap-appendicectomy, and treatment of recurrent or bilateral inguinal hernias. A co-payment does not apply if procedures are done at a day hospital or as a day case. |
| 🦾 Internal and External Prostheses | Covered up to 100% of the negotiated tariff. Subject to PMBs and pre-approval. Overall prostheses limit of R75,348 per family per year within the hospital limit. |
| 🦿 Instrumentation and disc prostheses, including components and fixation devices for the back or spine. | The following sub-limits apply: R31,832 per level, subject to the overall limit. Limited to 2 levels unless there is clinical motivation, or it has been approved within the PMB protocols. |
| 🧬 Internal Prostheses | Limited to R46,321 per year. Subject to the overall limit. Limited to one event per year unless it involves trauma or sepsis. Cement is not included. |
| 🩺 Aphakic Lenses | Subject to protocols and PMBs. Limited to R6,452 per lens. |
| 🧪 Cardiac Stents | One per lesion, maximum 3. Subject to the overall prostheses limit. Bare metal stents are limited to R16,774 per stent. Drug-eluting stents are limited to R23,625 per stent. |
| 📌 Internal sphincters and stimulators | Limited to PMBs. |
| 📍 Cochlear implants | Subject to the overall prostheses limit. |
| ☑️ Insulin pumps and monthly materials | Subject to the overall prostheses limit. |
| ✅ Unlisted prostheses, Artificial Limbs, and external prostheses, such as artificial eyes, etc. | Subject to the overall prostheses limit. Only covers children under 7. Limited to R19,089. |
| 🩸 Blood Transfusions | Covered up to 100% of the scheme tariff. |
| ↪️ Physiotherapy and Biokinetics | Covered up to 100% of the scheme tariff. |
| 🍎 Dietician and Occupational Therapy | Covered up to 100% of the scheme tariff. |
Discover the 5 Best Medical Aids under R300
Plus Day-to-Day Benefits
| 🔴 Day Hospital Procedures using a DSP hospital Network | Covered up to 100% of the scheme tariff. |
| 🟠 Co-payments on day procedures | This will apply depending on the treatment. |
| 🟡 Out-of-Hospital Consultations General Practitioners Specialists Outpatient Facilities | Covered up to 100% of the scheme tariff. There is a limit of 26 GP visits per family per year or 16 GP visits per beneficiary. There is a 30% co-payment after the 10th GP visit beneficiary. Members have the following number of visits to Specialists: Main Member – 5 visits Member + 1 Dependent – 7 Visits Member +2 and more dependents – 9 Visits |
| 🟢 Acute Medicine | Covered up to 100% of the scheme tariff. Paid from MSA. No accumulation towards the SPG or Above Threshold Benefit (ATB) exists. |
| 🔵 PMB Disease List Medicines | Covered up to 100% of the reference price. Limited to R16,763 per family per year. Limited to R9,854 per beneficiary per year. A 20% co-payment applies for using benefits above R10,416 per family. |
| 🟣 Other Chronic (non-CDL) medicines | Covered up to 100% of the reference price. Limited to R30,676 per family per year. Limited to R16,044 per beneficiary per year. Non-formulary medicines incur a 30% co-payment when obtained voluntarily. |
| 🔴 Pharmacy Advised Treatment (PAT) | Covered up to 100% of the reference price. Limited to R3,507 per family per year. A maximum of R252 per script is covered. |
| 🟠 Contraceptives | Covered up to 100% of the reference price. |
| 🟡 Oral and injectable | Limited to R1,838 per family per year. Subject to oral, injectable, and patch contraceptives. |
| 🟢 Mirena Device | Subject to a sub-limit of R2,100 per beneficiary every 5 years for abnormal uterine bleeding. |
Plus Optical Benefits
| 😎 Spectacle Lenses | Covered up to 100% of the DSP tariff. The following is covered: R221 per lens for clear single-vision lenses. R467 per lens for clear bifocal lenses. R809 per lens for multifocal lenses. Fixed tints up to 35%. |
| 👁️ Contact Lenses | Covered up to 100% of the DST tariff. Limited to R3,061 per beneficiary every 2 years. |
| 👓 Frames/Lens Enhancements | Covered up to 100% of the DSP tariff. Limited to R1,292 per beneficiary. |
| 🤓 Eye Tests | Covered up to 100% of the DSP tariff. Limited to one comprehensive consultation per beneficiary every 2 years. |
Plus Dentistry Benefits
| 1️⃣ Basic/Conservative Dentistry | Covered up to 100% of the scheme tariff. Limited to R7,434 per beneficiary and R9,371 per family per year. |
| 2️⃣ Consultations, Fillings, Extractions | Covered up to 100% of the scheme tariff. |
| 3️⃣ Root Canal | Limited to one set per beneficiary every 5 years. Subject to the necessary protocols. |
| 4️⃣ Preventative scale and polish | Limited to one per beneficiary every 4 years. Subject to benefit availability. |
| 5️⃣ Crowns Bridgework Dentures Orthodontics Removal of Impacted Wisdom Teeth Non-Surgical Periodontics | Covered up to 100% of the scheme tariff. Limited to R7,434 per beneficiary and R9,371 per family per year. |
| 6️⃣ Dental Implants | Limited to two implants per family per year over 5 years, limited to R16,380. |
| 7️⃣ Partial Metal Frame Dentures | Limited to beneficiaries 16> Limited to one set per beneficiary every 5 years. Subject to the advanced dentistry limit. |
| 8️⃣ Acrylic (Plastic) Dentures for beneficiaries 16> | Limited to one per beneficiary for members 16>. Subject to benefit availability. |
| 9️⃣ Maxillo-Facial and Oral Dental Surgery | Covered up to 100% of the Scheme Tariff. Only hospitalization benefits are payable in accidents, injuries, congenital anomalies, and oncology-related operations. |
Plus Auxiliary Benefits
| ➡️ Alternative Services include: Speech therapy Podiatry Occupational therapy Social worker Dietetics | Covered up to 100% of the scheme tariff. Collectively limited to R4,457 per family per year. Medicine dispensed is limited to acute medicine limits. |
| ↪️ Remedial and Other Therapies | Covered up to 100% of the scheme tariff. Collectively limited to R5,644 per family per year. |
| 🔁 Physiotherapy Out-of-Hospital and Biokinetics | Covered up to 100% of the scheme tariff. Limited to R2,982 per beneficiary and R4,772 per family. |
Plus Medical Appliances Benefits
- Covered up to 100% of the negotiated tariff.
- Limited to R16,097 per family per year.
- The following applies:
- Stoma Care is subject to a sub-limit of R8,279 per family per year.
- Wheelchairs are limited to one claim per beneficiary every three years (subject to pre-authorization).
- Hearing aids are limited to one claim per beneficiary every 2 years (subject to pre-authorization).
- Blood Pressure Monitors are subject to a sub-limit of R599 for beneficiaries registered for Hypertension.
Read more about How to Calculate Medical Aid Fringe Benefit
Plus Other Benefits
| ✈️ Air/Road Ambulance and Emergency Services | Covered up to 100% of Negotiated Tariff 24-hour Contact Center Access, including Telephonic Nurse Advice Line. Emergency: Subject to pre-approval within 72 hours of the emergency. Only a preferred provider can perform inter-hospital transfers. Emergency response by road or air to the scene of the occurrence, as well as transfer from the scene to the nearest, most appropriate facility Escort repatriation of stranded children is possible. Non-emergency: Subject to pre-authorization. Medically justifiable inter-facility transfers. Medical repatriation. |
| 🧠 Psychology and Psychiatry Treatment | Covered up to 100% of the scheme tariff. Limited to R10,437 per family and R5,219 per beneficiary. |
| ☑️ Infertility | Covered up to 100% of the scheme tariff. |
| 👩⚕️ Hospice and Private Nursing | Covered up to 100% of the Negotiated Tariff. Subject to the combined limit of 14 days per year except for PMBs. |
Plus Sizwe Hosmed Bambino Benefits
Sizwe Hosmed is concerned about its maternity mothers. This program offers information and advantages to help them during their pregnancy. In addition, pregnant women enrolled in the Bambino Programme are eligible for a complimentary maternity bag filled with baby goods at 24 weeks of pregnancy.
| ❤️ Sizwe Hosmed Bambino Program | Covered up to 100% of the scheme tariff. PMB based on clinical protocols. |
| 🧡 Hospital Confinement | Admissions can only be done to a DSP Hospital Network. Natural Delivery – Limited to 2 days Cesarean – Limited to 4 days. |
| 💛 Home Delivery | Covered up to 100% of the negotiated tariff. |
| 💚 Maternity Ultrasounds | Limited to three 2D and one 3D ultrasound in and out-of-hospital. |
| 💙 Maternity Visits/Consultations | Covered up to 100% of the scheme tariff. Extra 9 GP maternity appointments, of which 6 are for a GP or Midwife, and three are for a Specialist Obstetrician visit. |
| 💜 Antenatal Pathology Screening | Covered up to 100% of the scheme tariff. |
| 🤍 Vitamins | R120, subject to the day-to-day limit. |
| 🖤 Child Immunisation Benefit | According to the Immunisation schedule of the Department of Health, only up to 6 years old. |
Plus Preventative Care Benefits
| 🟥 Wellness Consultations | Limited to R1,219 per family per year. |
| 🟧 COVID-19 Vaccination | Covered according to guidelines. |
| 🟨 Diabetic eye care | Covered |
| 🟩 Pap Smear for female beneficiaries 18> | One per qualifying beneficiary yearly. |
| 🟦 Mammogram for female beneficiaries 40> | One per qualifying beneficiary yearly. |
| PSA for Male Beneficiaries 40> | One per qualifying beneficiary yearly. |
| 🟥 Cholesterol Test for beneficiaries 20> | One per qualifying beneficiary yearly. |
| 🟧 Flu Vaccine for all beneficiaries | One per beneficiary yearly. |
| 🟨 Blood Sugar | Test for those 15> – one test per qualifying beneficiary. |
| 🟩 Colon Cancer Blood Test for beneficiaries 50> | One per qualifying beneficiary yearly. |
| Blood Pressure test for all beneficiaries. | One per beneficiary yearly. |
| 🟦 HIV test for all beneficiaries | One per beneficiary yearly. |
| 🟥 HPV Vaccines for beneficiaries between 9 and 12. | One per qualifying beneficiary. |
| 🟧 Pneumococcal Vaccines for beneficiaries 65> | One per qualifying beneficiary yearly. |
| 🟨 Bone density testing for female beneficiaries between 50 and 69 and male beneficiaries 65 years old. | One per qualifying beneficiary yearly. |
| 🟩 HIV/AIDS Management Program | Covered up to 100% of the scheme tariff. Treatment is subject to the treatment care plan. Clinical protocols per CDL apply. |
| 🟦 COVID-19 Screening, Diagnosis, and Treatment | Covered up to 100% of the scheme tariff. Subject to PMB. |
POLL: 5 Best Hospital Plans for Unemployed
Plus Plan Chronic Diseases Benefit
Sizwe Hosmed Plus covers the following chronic conditions on the CDL list:
- ☑️ Addison’s Disease
- ☑️ Epilepsy
- ☑️ Asthma
- ☑️ Glaucoma
- ☑️ Bipolar Mood Disorder
- ☑️ Hemophilia
- ☑️ Bronchiectasis
- ☑️ HIV/AIDS
- ☑️ Cardiac Failure
- ☑️ Hyperlipidemia
and many more.
Sizwe Hosmed Plus covers the following 25 additional non-PMB conditions:
- ☑️ Attention Deficit Hyperactivity Disorder (ADHD)
- ☑️ Allergic Rhinitis
- ☑️ Anaemia: Vitamin B12 and Iron deficiency
- ☑️ Aplastic anemia
- ☑️ Anti-phospholipid syndrome
- ☑️ Benign Prostatic Hypertrophy (BPH)
- ☑️ Cushing’s Disease
- ☑️ Cystic Fibrosis
- ☑️ Depression
- ☑️ Endometriosis
and many more.
Discover more about health insurance
Plus Plan Exclusions and Waiting Periods
Plus Plan Exclusions
Sizwe Hosmed indicates that the following are excluded. However, these are only a few items; the complete list can be viewed on the Sizwe Hosmed website.
- Costs that exceed the annual or biennial maximum allowed for the category
- Operations, medicines, treatments, and procedures for cosmetic purposes or personal reasons
- Medical service not deemed necessary by the medical advisor for the management of the medical condition
- Treatment with no proven efficacy and safety
- Services rendered by unregistered persons or institutions not registered in terms of any law
- Abdominoplasties and repair of divarication of abdominal muscles
- Geriatric hospital, nursing home, frail care facility, or similar accommodations and services
- Alternative therapists, such as art therapists, aromatherapists, massage therapists, reflexologists, and Chinese medicine practitioners
- Anabolic steroids and immunostimulants, excluding immunoglobulins and growth hormones
- Ante- and postnatal exercises
- Ozone therapy
and more.
Plus Plan Waiting Periods
When new members join the plan, they may be subject to a three-month general waiting period during which they cannot receive benefits. Except in the case of Specified Minimum Benefits, if the new member has a pre-existing ailment, they may be subject to a one-year condition-specific waiting period.
Sizwe Hosmed Plus Plan vs. Similar Plans from other Medical Schemes
| 🔎 Medical Aid Plan | 🥇 Sizwe Hosmed Plus | 🥈 Fedhealth Maxima EXEC | 🥉 Medihelp MedElite |
| 👤 Main Member Contribution | R7,227 | R8,456 | R7,368 |
| 👥 Adult Dependent Contribution | R6,893 | R7,340 | R6,900 |
| 🍼 Child Dependent Contribution | R1,577 | R2,613 | R1,998 |
| 💙 Hospital Cover | Unlimited for PMBs | Unlimited | Unlimited |
| 🟦 Oncology Cover | R679,00 | R624,000 | R299,000 |
Poll: 5 Best Gap Cover Options for Under R3000
Our Verdict on The Plus Plan
Sizwe Hosmed Plus Plan is a comprehensive medical aid plan offered by Sizwe Medical Fund in South Africa. The plan is designed to cater to the healthcare needs of individuals and families with a moderate budget. It provides a range of benefits that cover in-hospital and day-to-day medical expenses, including chronic medication, preventative care, and emergency services. One of the key features of the Sizwe Hosmed Plus Plan is its affordability. It is priced competitively in the market, making it an excellent option for individuals and families who want quality healthcare coverage without breaking the bank. The plan also offers generous limits for benefits such as hospitalization, chronic medication, and primary healthcare services.
Another advantage of the Sizwe Hosmed Plus Plan is its flexibility. Members can choose from various network providers, including hospitals, doctors, and specialists. The plan also offers a variety of benefit options, allowing members to customize their coverage according to their unique healthcare needs.
- You might also like: Siswe Hosmed Review
- You might also like: Sizwe Hosmed Gold Ascend
- You might also like: Sizwe Hosmed Platinum Enhanced EDO
- You might also like: Sizwe Hosmed Platinum Enhanced
- You might also like: Sizwe Hosmed Silver Hospital
- You might also like: Sizwe Hosmed Titanium Executive
- You might also like: Sizwe Hosmed Value Core
- You might also like: Sizwe Hosmed Value
- You might also like: Sizwe Hosmed Access Saver 25
- You might also like: Sizwe Hosmed Access Core
- You might also like: Sizwe Hosmed Copper Essential
- You might also like: Sizwe Hosmed Gold Ascend EDO
Plus Plan Frequently Asked Questions
Does the Sizwe Hosmed Plus Plan cover dental treatment?
Yes, the plan covers dental treatment for its members. However, the coverage is limited, and members may have to pay a co-payment or use their savings account to cover the cost.
Does the Sizwe Hosmed Plus Plan offer wellness programs?
Yes, the plan offers a range of wellness programs, including health assessments, fitness programs, and disease management programs.
Are child immunizations covered under the Sizwe Hosmed Plus Plan?
Yes, child immunizations are covered under the plan’s preventative care benefit. In addition, the plan covers the cost of recommended vaccines for children up to a certain age.
What are PMB conditions under the Sizwe Hosmed Plus Plan?
PMB conditions are prescribed minimum benefits that the plan is required by law to cover. These include certain medical conditions such as diabetes, HIV/AIDS, and cancer.
Is chronic medication covered under the Sizwe Hosmed Plus Plan?
Yes, the plan covers the cost of chronic medication for its members. However, members may have to pay a co-payment or use their savings account to cover the cost.
What are the in-hospital benefits of the Sizwe Hosmed Plus Plan?
The plan offers a range of in-hospital benefits, including hospitalization costs, specialist fees, and surgical procedures.
Does the Sizwe Hosmed Plus Plan cover the cost of wheelchairs?
Yes, the plan covers the cost of wheelchairs for members who require them. However, there may be limits to the coverage, and members may have to pay a co-payment or use their savings account to cover the cost.
Are hearing aids covered under the Sizwe Hosmed Plus Plan?
Yes, the plan covers the cost of hearing aids for members who require them.
Does the Sizwe Hosmed Plus Plan cover the cost of pregnancy vitamins?
Yes, the plan covers the cost of pregnancy vitamins for pregnant members.
Does the Sizwe Hosmed Plus Plan cover alternative therapies such as acupuncture and chiropractic?
Yes, the plan covers the cost of alternative therapies such as acupuncture and chiropractic.
Does the Sizwe Hosmed Plus Plan cover the cost of cosmetic surgery?
No, the plan does not cover the cost of cosmetic surgery. However, there may be exceptions for cases where the surgery is deemed medically necessary.
You might also like
Table of Contents
Free Medical Aid Quote
Our Trusted Partners
We work with leading medical aid companies in South Africa.

7 Actionable Ways to save 32% on your MEDICAL AID in 14 days.

- +27 72 7967 530
- [email protected]
- 2nd Floor, West Tower, Nelson Mandela Square, Sandton, 2196, Johannesburg, Gauteng, South Africa
🔎 Report a bug or outdated data to be updated to [email protected]
© Medicalaid.com | All rights Reserved |
Copyright 2024
Top 5 Medical Aids
Top 5 Gap Cover Plans
































