- Medical Aid
- Currently Trending
The Best Medical Aids
- Compare Plans
- Gap Cover
- Best Gap Covers
- Hospital Plans
- Currently Trending
The Best Hospital Plans
- Medical Insurance
- Pet Insurance
Medihelp MedAdd Medical Aid Plan
Overall, the Medihelp MedAdd Medical Aid Plan is a trustworthy and comprehensive medical aid plan that offers 24/7 medical emergency assistance and allied healthcare services to up to 3 Family Members. The Medihelp MedAdd Medical Aid Plan starts from R3,354 ZAR.
| 👤 Main Member Contribution | R3,354 |
| 👥 Adult Dependent Contribution | R2,832 |
| 💙 Child Dependent Contribution | R1,134 |
| 🔁 Gap Cover | None |
| 🏥 Hospital Cover | Unlimited |
| ➡️ Oncology Cover | R262,000 |
| 🤓 Optometry Benefit | ☑️ Yes |
| 🦷 Dentistry Benefit | ☑️ Yes |
| 🧠 Mental Healthcare Program | ☑️ Yes |
| 🌎 International Cover | None |

Medihelp MedAdd Plan – 13 Key Point Quick Overview
- ☑️ Medihelp MedAdd Plan Overview
- ☑️ Medihelp MedAdd Plan Contributions and Medical Savings
- ☑️ MedAdd Plan Benefits and Cover Comprehensive Breakdown
- ☑️ MedAdd Day-to-Day Benefits
- ☑️ MedAdd Medical Plan Benefit Breakdown
- ☑️ MedAdd Hospitalization and Advanced Treatment
- ☑️ Radiology, Pathology, and Medical Technologist Services
- ☑️ MedAdd Emergency Benefits
- ☑️ MedAdd Added Insured Benefits
- ☑️ Medihelp MedAdd Plan Exclusions and Waiting Periods
- ☑️ Medihelp MedAdd Plan vs. Similar Plans from other Medical Schemes
- ☑️ Our Verdict on The MedAdd Plan
- ☑️ MedAdd Plan Frequently Asked Questions
Medihelp MedAdd Plan Overview
The Medihelp MedAdd medical aid plan is one of 11, starting from R3,354 and includes generous medical savings, day-to-day benefits when savings are depleted, consultations, oncology, dental and optometry benefits, allied healthcare services, radiology, pathology, and more. Gap Cover is not available on the Medihelp MedAdd Plan. However, Medihelp offers 24/7 medical emergency assistance. According to the Trust Index, Medihelp has a trust rating of 4.2.
MediHelp has the following 11 plans to choose from:
- ✅ MediHelp Medprime
- ✅ MediHelp MedPrime Elect
- ✅ MediHelp MedPlus
- ✅ MediHelp MedElite
- ✅ MediHelp MedVital
- ✅ MediHelp MedVital Elect
- ✅ MediHelp MedSaver
- ✅ MediHelp MedMove
- ✅ MediHelp MedElect
- ✅ MediHelpMedAdd
- ✅ MediHelp MedAdd Elect
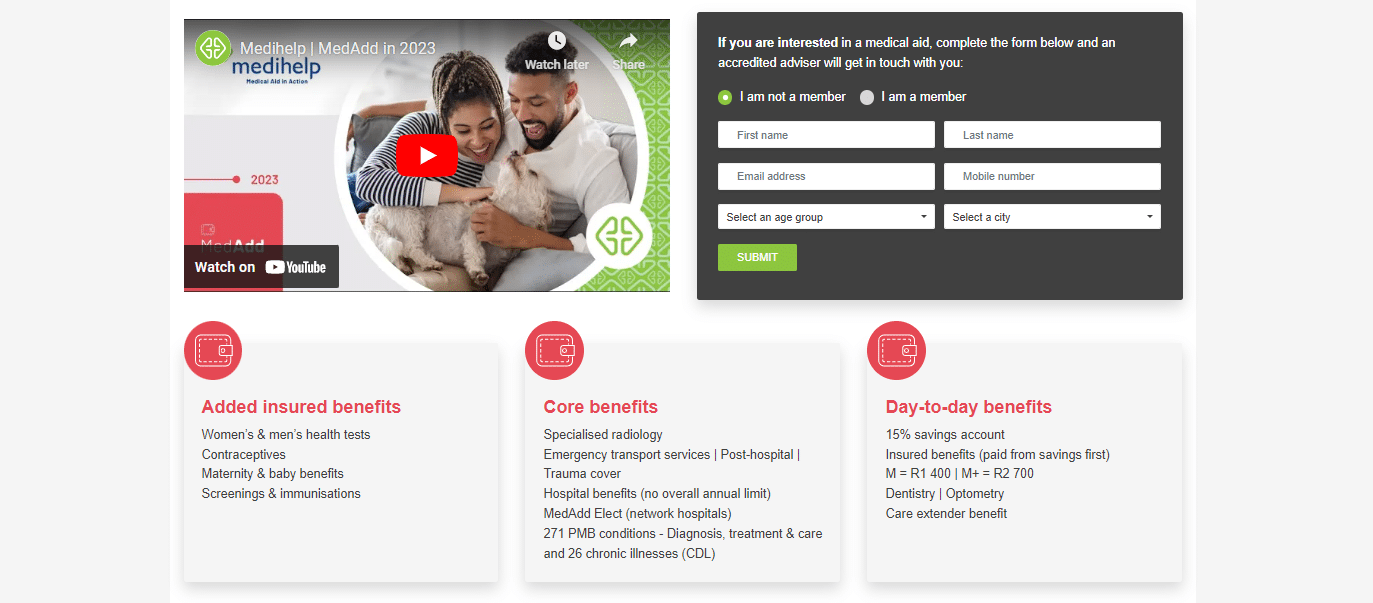
Medihelp MedAdd Plan Contributions and Medical Savings
Medihelp MedAdd Contributions
| 👤 Main Member | 👥 +1 Adult Dependent | 💙 +1 Child Dependent |
| R3,354 | R2,832 | R1,134 |
Medihelp MedAdd Medical Savings Account
| 👤 Main Member | 👥 +1 Adult Dependent | 💙 +1 Child Dependent |
| R504 per month | R426 per month | R168 per month |
| R6,048 per year | R5,112 per year | R2,016 per year |
Read more about the 5 Best Medical Aids under R1000
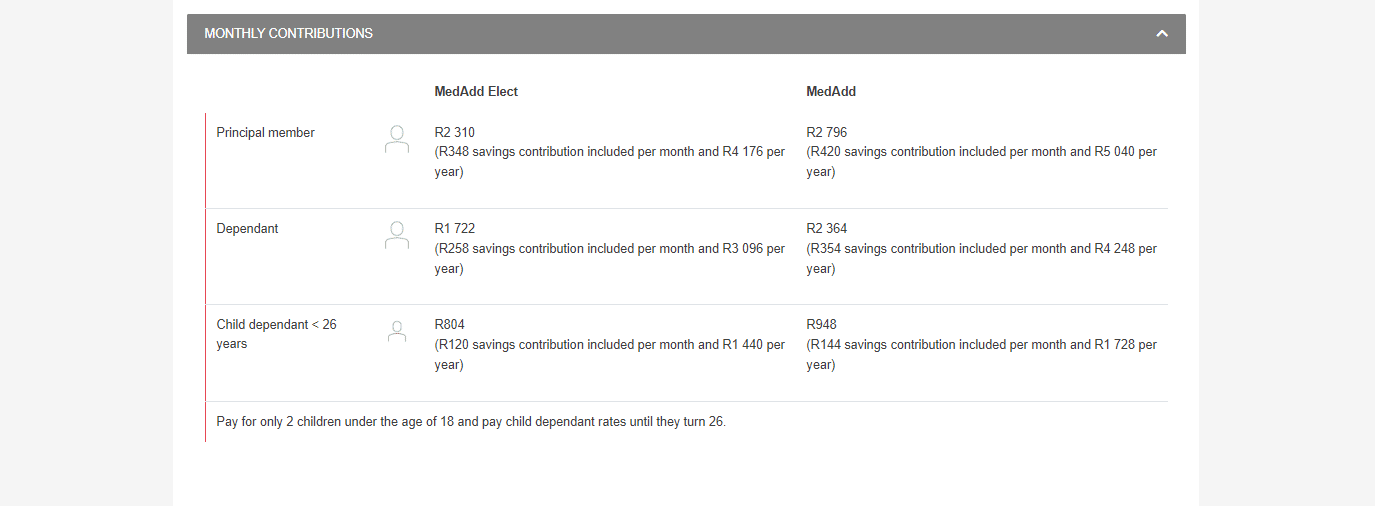

MedAdd Plan Benefits and Cover Comprehensive Breakdown
MedAdd Accumulative Unused Savings Contributions
MedAdd is a handy credit option that allows you to immediately access the cash in your medical savings account for the current year. In addition, any unused money is carried forward and earns interest the next year. Each month, a portion of your contributions equal to 15% is allocated to a savings account as follows:
- This amounts to R504 per month or R6,048 per year for the principal member.
- Adult dependents receive R426 per month or R5,112 per year.
- Child dependents receive R168 per month or R2,016 per year.
- These savings are intended to cover daily medical expenses.
- At the start of each year, the entire year’s contributions to the savings account become available as a credit facility.
- Any funds that are not used are carried forward to the following year.
- The remaining portion of your monthly contributions is used to fund your comprehensive core and insured benefits.
Except for services relating to prescribed minimum benefits (PMB), qualifying claims are paid from the savings account first until the account is empty. Claims are then reimbursed until the insured’s daily benefits are exhausted. PMB services are paid from day-to-day benefits until depleted, then from core benefits without limitation.
Discover the 5 Best Hospital Plans under R200

MedAdd Day-to-Day Benefits
Benefits are first paid from the available Medical Savings Account. Once funds are depleted, the following limits apply to day-to-day benefits:
- All claims are paid up to 100% of the Medihelp Tariff (MT).
- Main Members – limited to R1,700 per year.
- Main Member and Dependents – limited to R2,700 per year.
Consultations
- GP appointments and follow-up appointments.
- Specialists
- Telemedicine, virtual consultations, and visits from nurses at network pharmacies.
- Pharmacies providing primary care and emergency units, including primary care drug therapists, in terms of consultations and follow-ups.
- Physiotherapy, including material and treatment.
Medication
- The medication is obtained through the Medihelp Preferred Pharmacy Network and prescribed or given by a physician.
- Acute and non-PMB chronic medication and self-medication, including emergency room drugs and immunizations.
- Generic medicine – 100% of the MMAP Original medicine if no generic equivalent – 80% of the MT.
- 70% of the MMAP comprises original medication taken willingly when a generic alternative is available.
- Homeopathy, naturopathy, and osteopathy account for 25% of the possible daily benefit.
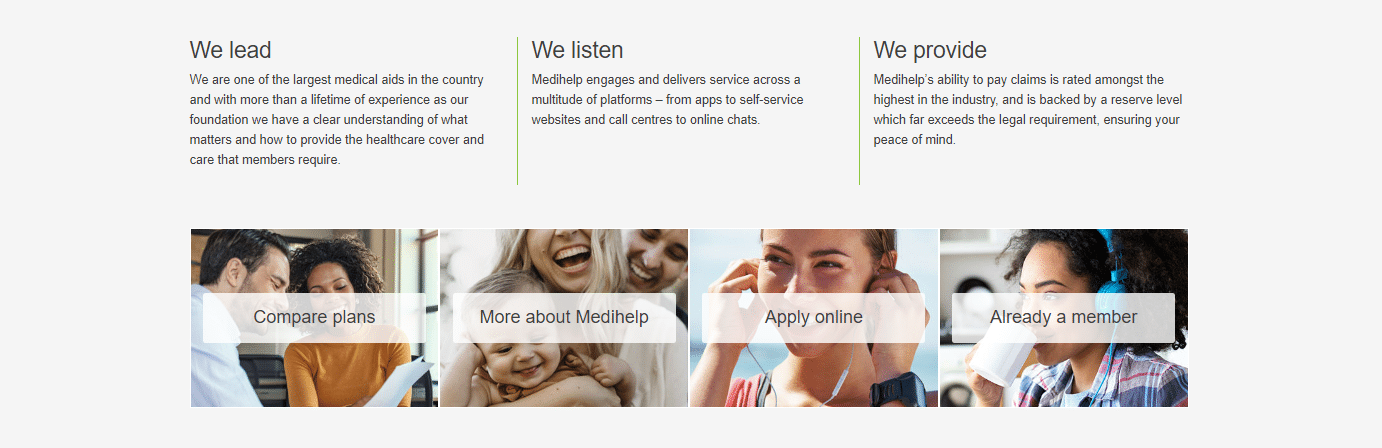
MedAdd Medical Plan Benefit Breakdown
Care Extender
| ☑️ Additional GP Consultation | A beneficiary’s Pap smear, mammography, prostate test, FOBT, or bone mineral density test activates a family consultation benefit. |
| ✅ R475 for Self-Medication | After a beneficiary claims the combo health screening (blood glucose, cholesterol, BMI, and blood pressure measurement) at a preferred pharmacy clinic, the family will receive R475 for non-prescribed medicine. |
| ☑️ PMB Chronic Medicine | Pre-approval and registration on Medihelp’s PMB drug management program are required. Covered up to 100% of the MHRP. There is a 60% co-payment for non-compliance with the formulary and DSP. The unlimited cover is provided. |
| ✅ Clinical Psychology and Psychiatric Nursing in and out-of-hospital | Covered up to 100% of the MT. Claims for services and treatment are paid from the medical savings account. |
Allied Medical Services (Out-of-Hospital)
Allied Medical Services (Out of Hospital) include:
- Occupational and speech therapy
- Dietitian services
- Audiometry
- Podiatry
- Massage
- Orthoptic
- Chiropractic
- Homeopathic
- Herbal and naturopathic
- Osteopathic
- Biokinetic services
Pathology and Medical Technologist Services
| ➡️ Oxygen | Covered out-of-hospital. Subject to pre-approval and clinical protocols and must be prescribed by a medical doctor. Covered up to 100% of the MT. Unlimited cover. 20% co-payment if this benefit is not pre-approved before treatment. |
| 🤓 Optometry | Subject to pre-authorization by a PPN. Services must be via a PPN provider. There is a limit of 1 composite consultation, including refraction test, tonometry, and visual field test per 2-year cycle. Covered up to 100% of the MT. |
| 👓 Spectacles or Contact Lenses | Spectacles – Frames or lens enhancement Limited to R285 per beneficiary/2 years. Lenses (1 x clear pair) Limited to single-vision or bifocal lenses per beneficiary/2 years. Multifocal lenses are covered at the cost of bifocal lenses. Contact lenses Limited to R670 per beneficiary/2 years. |
MedAdd General and Specialized Dentistry
| 📌 Conservative Dental Services | Benefits are subject to Dental Risk Company (DRC) protocols, contracted to Medihelp as a DSP. Benefits are subject to protocols and are limited to certain item codes. |
| 📍 Routine Check-ups | Covered up to 100% of the MT. Limited to once every six months for beneficiaries <18. Only available to two beneficiaries per year. The benefit is paid from the savings account for beneficiaries 18>. |
| 🦷 Oral Hygiene | Scale and Polish Treatments: Covered up to 100% of the MT. Limited to once every six months for beneficiaries <18. Only available to two beneficiaries per year. The benefit is paid from the savings account for beneficiaries 18>. Fluoride Treatment for children between 5 and 13: Covered up to 100% of the MT. Paid from the medical savings account. Fissure sealants for children between 5 and 16 (permanent teeth): Covered up to 100% of the MT. Paid from the medical savings account. |
| 😷 Fillings | Treatment plans and x-rays might be requested where multiple fillings are necessary. Pre-approval is required for 4> fillings per year and 2 fillings on front teeth per visit. Covered up to 100% of the MT. Limited to 1 filling per tooth per year for beneficiaries <18. Fillings for beneficiaries 18> are paid from the available medical savings. |
| ✳️ Tooth Extractions and Root Canals on permanent teeth in the Dentist’s chair | Pre-authorization for 4> extractions in a single visit. Covered up to 100% of the MT. Beneficiaries under 18 have unlimited cover. Treatment for beneficiaries 18> is paid from the available medical savings. |
| 😊 Laughing Gas (Dentist’s Chair) | Covered up to 100% of the MT. Paid from the medical savings account. |
| 💤 Dentistry under conscious sedation (Dentist’s chair) | The benefit is only available for removing impacted teeth (3rd molars) Covered up to 100% of the MT 20% co-payment for no authorization. |
| 😴 Dentistry under general anesthesia in a day procedure facility, including the removal of impacted teeth and extensive dental treatment for children <7 (only once per beneficiary yearly) | Covered up to 100% of the MT Member must pay the first R3,700 per admission. 35% co-payment for procedures not performed in a day procedure network. 20% co-payment for no authorization. |
| 🔎 Special Needs Patients – dentistry under general anesthesia in a day procedure | Covered up to 100% of the MT 35% co-payment for procedures not performed in a day procedure network. 20% co-payment for no authorization. |
| 🦷 Plastic Dentures | Covered up to 100% of the MT. Paid from the medical savings account. Limited to one set per beneficiary/4 years. |
| ❌ X-Rays | Intra-Oral X-Rays Covered up to 100% of the MT. Beneficiaries under 18 have unlimited cover. Treatment for beneficiaries 18> is paid from the available medical savings. Extra-Oral X-Rays Covered up to 100% of the MT. Beneficiaries under 18 have unlimited cover. Treatment for beneficiaries 18> is paid from the available medical savings. |
| 🪥 Specialized Dentistry | Subject to pre-authorization and DRC protocols. |
| ☑️ Partial Metal Frame Dentures | Covered up to 100% of the MT. Paid from the savings account. 20% co-payment for no authorization. |
| 🙂 Maxillofacial Surgery and Oral Pathology | Benefits for temporomandibular joint (TMJ) benefit limited to non-surgical treatment or interventions. Covered up to 100% of the MT. Paid from the savings account. 20% co-payment for no authorization. |
| 👑 Crowns and Bridges | Covered up to 100% of the MT. Paid from the savings account. 20% co-payment for no authorization. |
| 🚩 Implants | Covered up to 100% of the MT. Paid from the savings account. 20% co-payment for no authorization. |
| 🔁 Orthodontic Treatment | Covered up to 100% of the MT. Paid from the savings account. Limited to once per beneficiary <18. Payment is made from the authorization date until the patient turns 18. |
| 📊 Periodontal Treatment | Covered up to 100% of the MT. Paid from the savings account. 20% co-payment for no authorization. |
POLL: 5 Best Medical Aid for Unemployed in South Africa
External Prostheses and Medical Appliances
| ☑️ Services in and out of the hospital, including fitting, cost of repairs, maintenance, spares, accessories, and adjustments on the following: Artificial Eyes Speech and Hearing Aids Artificial Limbs Wheelchairs External Breath Prostheses Medical Appliances CPAP Apparatus | Covered up to 100% of the MT. Paid from the savings account. |
| ☑️ Hyperbaric Oxygen Treatment (In and Out-of-Hospital) | Covered up to 100% of the MT. Limited to R800 per family per year. |
| ☑️ Stoma Components Incontinence Products or Supplies | Covered up to 100% of the MT. The unlimited cover is available. |
MedAdd Hospitalization and Advanced Treatment
| 📌 Chronic Illness and PMB | Subject to protocols, pre-authorization, DSPs, and the specialist network. Covered up to 100% of the cost or the contracted tariff. Unlimited cover provided. Co-payments can apply if not using a DSP or deviating from the code. |
| 📍 Trauma Benefits This applies to major trauma requiring hospitalization, for example: Motor Vehicle Accidents Stab Wounds Gunshot Wounds Head Trauma Burns Near-drowning | Subject to authorization, PMB protocols, and case management. Covered up to 100% of the cost or the contracted tariff. |
| ☑️ Post-Exposure Prophylaxis (HIV/AIDS) | Subject to authorization, PMB protocols, and case management. Covered up to 100% of the cost or the contracted tariff. |
Emergency Transport Services via Netcare 911
| ☑️ In the Beneficiary’s Country of Residence (RSA, Lesotho, Eswatini, Mozambique, Namibia, Zimbabwe, Botswana), including road and air transport. | Unlimited Cover. Covered up to 100% of the MT. If not pre-approved, a 50% co-payment applies. |
| ☑️ Outside the beneficiary’s Country of Residence | Road Transport Covered up to 100% of the MT. If not pre-approved, a 50% co-payment applies. Limited to R2,320 per case. Air Transport Covered up to 100% of the MT. If not pre-approved, a 50% co-payment applies. Limited to R15,400 per case. |
MedAdd Hospitalization
(Only MedAdd hospital and day procedure network can be used)
| ✅ Intensive Care and high-care wards Ward Accommodation Theatre fees Treatment and medicine in the ward In-hospital consultation with GPs and specialists Surgery Anesthesia | Unlimited Cover. Covered up to 100% of the MT. If not pre-approved, a 20% co-payment applies. If not admitted to a hospital/day procedure facility in the network, a 35% co-payment applies. Additional co-payments on certain procedures may apply. |
| ✅ Day Procedures (Including Ophthalmological, endoscopic, ear, nose, and throat procedures, dental procedures, removal of skin lesions, circumcisions, and procedures as pre-authorized) | Unlimited Cover. Covered up to 100% of the MT. If not admitted to a hospital/day procedure facility in the network, a 35% co-payment applies. Additional co-payments on certain procedures may apply. |
| ✅ Hospital Medicine upon Discharge | Covered up to 100% of the MT. There is an R390 limit per admission. |
MedAdd Childbirth and Home Delivery
Childbirth
Subject to pre-authorization, protocols, and case management
- Unlimited Cover.
- Covered up to 100% of the MT.
- If not pre-approved, a 20% co-payment applies.
Home Delivery
Includes the following:
- Professional Nursing Fee
- Equipment
- Material and Medicine
- Covered up to 100% of the MT.
- Limited to R14,900 per event.
- If not pre-approved, a 20% co-payment applies.
Worth the read:
- 5 Best Hospital Plans for Babies
- 5 Best Medical Aids for Babies in South Africa
- Best Medical Aid for Women
Radiology, Pathology, and Medical Technologist Services
- In-Hospital cover only.
- Subject to clinical protocols and approved hospital admission.
- Members must use Ampath as the contracted Pathology DSP.
| 📌 Radiography | Covered up to 100% of the MT. Limited to R1,210 per family yearly. |
| 📍 Specialized Radiography | MRI and CT scans Subject to pre-authorization. Covered up to 100% of the MT. Unlimited Cover. Member pays the first R3,200 per examination and R2,700 out of the hospital. Angiography Covered up to 100% of the MT. Unlimited Cover. |
| ☑️ Clinical Technologist Services | Covered up to 100% of the MT. Unlimited Cover. |
| ❤️ Organ Transplants | Covered up to 100% of the MT. Unlimited Cover. Subject to pre-authorization and clinical protocols. Cornea implants Covered up to 100% of the MT. Limited to R32,600 per implant yearly. |
| ☑️ In-hospital Oxygen | Covered up to 100% of the MT. Unlimited Cover. |
| ✅ Renal Dialysis Acute Renal Dialysis Chronic/Peritoneal Renal Dialysis | Covered up to 100% of the MT. Unlimited Cover. Subject to pre-authorization and clinical protocols. 20% co-payment if not pre-approved. |
| ✳️ Post-Hospital Care Speech therapy, occupational therapy, and physiotherapy 30 days after discharge | Accessible day-to-day benefits cover prescription medication and medical equipment. Covered up to 100% of the MT. Limited to the following: Main Member – R2,100 per year. Main Member + Dependents – R3,000 per year. |
| 📌 Other Medical Services Dietitian services, physiotherapy, and occupational therapy Speech therapy Audiometry and orthoptic services Podiatry | Must be pre-approved and requested by the treating physician Covered up to 100% of the MT. Unlimited Cover. |
| 📍 Psychiatry Psychiatrist-provided hospital and outpatient treatments General ward accommodations Institution-supplied medication Outpatient consultations | Covered up to 100% of the MT. Limited to R27,600 per beneficiary per year, with a limit of R38,000 per family per year. If not pre-approved, a 20% co-payment applies. |
| ☑️ Oncology PMB Cases | Pre-authorization and Medihelp Oncology Program registration are required. Protocols, a DSP, and the MORP apply. Covered up to 100% of the MT. Unlimited Cover. 10% co-payment on non-DSP treatment. 20% co-payment for deviating from protocol. |
| ✅ Oncology Non-PMB Cases | Covered up to 100% of the MT. Limited to R242,000 per family per year. 10% co-payment on non-DSP treatment. 20% co-payment for deviating from protocol. |
| ✔️ Hospice Services and Subacute Care Facilities | Covered up to 100% of the MT. 20% co-payment if not pre-authorized Unlimited cover. |
| 📌 Palliative Care | Covered up to 100% of the MT. 20% co-payment if not pre-authorized Limited to R24,000 per family per year. |
| 📍 Private Nursing | Covered up to 100% of the MT. 20% co-payment if not pre-authorized Unlimited cover. |
| ☑️ Appendectomy – Conventional or Laparoscopic Procedure | Unlimited cover. Covered up to 100% of the MT. |
| ✅ Appendectomy – Conventional or Laparoscopic Procedure | Member pays the first R6,600 per admission. Covered up to 100% of the MT. |
MedAdd Emergency Benefits
A medical emergency is a sudden and unexpected occurrence that necessitates quick medical or surgical treatment to safeguard a patient’s health. Failure to offer medical or surgical treatment would result in severe impairment of bodily functioning or severe dysfunction of a bodily organ or portion or jeopardize the individual’s life. Netcare 911 is the designated service provider for Medihelp’s emergency transport services, and you must contact them in an emergency. Phone 082 911. Furthermore, you may also seek assistance at the nearby hospital’s emergency room. However, the following conditions apply:
- Emergency admissions must be reported to Medihelp on the following business day by calling 086 0200 678.
- If you visit an emergency facility but are not hospitalized, the care you receive will be covered by your regular plans.
- Facilities costs are not included.
Emergency Transport Services via Netcare 911
| 📌 In the Beneficiary’s Country of Residence (RSA, Lesotho, Eswatini, Mozambique, Namibia, Zimbabwe, Botswana), including road and air transport. | Unlimited Cover. Covered up to 100% of the MT. If not pre-approved, a 50% co-payment applies. |
| 📌 Outside the beneficiary’s Country of Residence | Road Transport Covered up to 100% of the MT. If not pre-approved, a 50% co-payment applies. Limited to R2,320 per case. Air Transport Covered up to 100% of the MT. If not pre-approved, a 50% co-payment applies. Limited to R15,400 per case. |
MedAdd Added Insured Benefits
- With a strong emphasis on preventative care, early diagnosis of potential health problems, and maternity benefits and childcare, these benefits are offered annually in addition to your insured benefits unless otherwise specified.
- Protocols and item codes may be applicable.
- Members can look for network provider information on Medihelp’s website or app using the provider search option.
- You can also sign up for HealthPrint, a free online health and fitness program offered by Medihelp, to activate the specified benefits.
MedAdd Women’s Health
| 1️⃣ Mammogram | For women 40 – 75 years old. Every two years. A medical doctor must request it. |
| 2️⃣ Pap Smear | For women 21 – 65 years old. Every three years. A medical doctor must request it. |
| 3️⃣ Flu Vaccines | Once yearly. It must be done at network pharmacy clinics. |
| 4️⃣ Contraceptives | Oral, injectable, or implantable contraceptives Female beneficiaries up to 50 years. Covered up to R155 per month and up to R2,015 per beneficiary. Intra-uterine devices for women up to 50 years Every 60 months. Covered up to R2,420 per beneficiary. |
Try our free Menstrual Cycle Calculator
Enhanced Maternity Benefits
HealthPrint’s Maternity and Infant program registration will activate these additional benefits per family per year.
- Ten prenatal and postnatal consultations with a midwife, general practitioner, or gynecologist. However, a recommendation from a network GP to the gynecologist is not required.
- Two prenatal and postnatal visits to a lactation consultant, dietician, or antenatal classes.
- Two 2D ultrasound imaging.
Child Benefits
- Babies <2 years receive two additional visits to a general practitioner, pediatrician, or ear, nose, and throat specialist. However, a network Physician reference is not required to see these specialists.
- In network pharmacy clinics, the full series of regular child immunizations are covered for up to seven years.
- Vaccination of children against influenza at network pharmacy clinics.
READ: Health Insurance for Kids
Routine Screening and Immunization
- A combo test, including blood glucose, cholesterol, BMI & blood pressure measurement.
- Individual tests, including blood glucose or cholesterol.
- HIV testing, counseling & support
- A tetanus vaccine
- A flu vaccination
- Two HPV vaccinations for girls and boys between 10 – 14 years or three between 15 – 26 years
Men’s Health
- A prostate test (PSA level) was requested by a physician for men aged 40 to 75.
- Flu vaccination is administered at network pharmacies.
Screening and Immunization for beneficiaries 45>
- An FOBT test for recipients 45-75 years
- Women aged 65 and older can access one bone mineral density test every two years if requested by a physician.
- A Pneumovax vaccine on a 5-year cycle for each 55-year-old with asthma or COPD who is registered.
Wellness Support
- Back Treatment – this benefit covers back therapy at a DBC facility as an alternative to surgery for eligible patients. Moreover, treatment is a precondition for spinal surgery.
- One dietitian consultation with each registered HealthPrint member whose BMI is greater than 30 and whose BMI was determined by a BMI test.
- An oncology schedule is provided in conjunction with Independent Clinical Oncology Network oncologists (ICON)
- HIV program – Presented in partnership with LifeSense Disease Management
Care Extender Benefit
Additional GP visit
- Once your increased insured benefits pay for a Pap smear, mammography, prostate test, FOBT, or bone mineral density test, the family will receive a one-time GP visit benefit.
- Test protocols will apply to this benefit.
Self-Medication (R475)
Once your enhanced insured benefits pay for a combo health screening (blood glucose, cholesterol, BMI, and blood pressure), the family will receive a one-time R475 for self-medication.

Medihelp MedAdd Plan Exclusions and Waiting Periods
Medihelp MedAdd Exclusions
As medical research advances, new medical services are introduced each year. However, Medihelp covers life-saving medical treatment first. The Medical Schemes Act requires medical schemes to cover the diagnostic, treatment, and care costs of the mandated minimum benefits (PMB) without co-payments or limits. Furthermore, services must follow legislation’s PMB treatment algorithms and Medihelp’s managed healthcare guidelines, which may include pharmaceutical formularies. Medihelp will cover the cost of a substitute treatment if a protocol or formulary drug is ineffective or hazardous. However, the Medihelp MedAdd plan excludes several items, including but not limited to the following:
- Restorative fillings for teeth injured by toothbrush abrasion, attrition, erosion, and fluorosis
- Resin bonding for restorations is billed separately from the restoration.
- The polishing of restorations
- Gold foil embellishments
- Ozone therapy Diagnostic dentures and laboratory fees
- Snoring aids and accompanying laboratory expenses
- Provisional dentures and corresponding laboratory fees
- Implants for third molars
- Dolder bars and accompanying implant abutments, including laboratory costs
- Fees for laboratory delivery
- Cosmetic orthodontic treatment and accompanying laboratory expenses
- Orthodontic treatment for those aged 18 and older
- Surgical periodontics, including gingivectomies, periodontal flap surgery, tissue grafting, and tooth hemisection.
- Placement of perio-chip
- Appointments missed
- The plan of treatment finished
- Electrognathographic recordings, pantographic recordings, and similar electronic examinations
- Tests for caries susceptibility and microbiology
- Pulp tests
- The price of mineral trioxide
- Enamel micro-abrasion
- All biological, biosimilar, and other drugs excluded by Medihelp’s drug exclusion list
- Advanced medical techniques, surgical instruments, and medications
- Blood-derived pharmaceuticals, including autologous blood serum eye drops, and more.
You might consider reading more about Medical Aid Ombudsman – Complaints Procedure
Medihelp MedAdd Waiting Periods
During waiting periods, members are eligible for membership but not for benefits. For example, Medihelp could implement either a general or condition-specific waiting period as follows:
- The general waiting period is up to three months from the date of membership. During this time, you will not be eligible for benefits other than the minimum prescribed benefits (PMB). During this waiting period, the Scheme will not pay any claims you file.
- From the day you join, a condition-specific waiting period of up to 12 months applies. During this period, you will not be eligible for benefits related to a specific ailment for which you get medical advice, a diagnosis, care, or treatment (this excludes PMB).
Medihelp MedAdd Plan vs. Similar Plans from other Medical Schemes
| 🔎 Overview | 🥇 Medihelp MedAdd | 🥈 POLMED Aquarium | 🥉 LA Health Active |
| 👤 Main Member Contribution | R3,354 | R | R |
| 👥 Adult Dependent Contribution | R2,832 | R | R |
| 💙 Child Dependent Contribution | R1,134 | R | R |
| 🔁 Gap Cover | None | None | None |
| 📉 Annual Limit | Unlimited Hospital Cover | Unlimited | Unlimited Hospital Cover |
| 💶 Prescribed Minimum Benefits | ☑️ Yes | ☑️ Yes | ☑️ Yes |
| 💻 Screening and Prevention | ✅ Yes | ✅ Yes | ✅ Yes |
| 💳 Medical Savings Account | ☑️ Yes | None | ☑️ Yes |
| ➡️ Oncology Cover | R262,000 | R271,400 | R228,000 |

Our Verdict on The MedAdd Plan
Medihelp’s MedAdd is a medical aid plan offering comprehensive coverage for various healthcare needs. It provides unlimited private hospital cover, including in-hospital specialists, surgeries, diagnostic procedures, and full coverage for chronic medication (subject to scheme protocols). Members have access to day-to-day benefits, such as GP consultations, specialist consultations, diagnostic tests, emergency medical services coverage, and international travel insurance. The plan also offers value-added services, such as access to wellness programs and lifestyle benefits. However, while MedAdd provides peace of mind for members who may require expensive medical treatment, it may be more expensive than other medical aid plans, particularly for those who do not require comprehensive coverage.
The plan may have certain exclusions or limitations that should be carefully reviewed before joining. But ultimately, the plan’s benefits make it a strong option for those seeking comprehensive healthcare coverage in South Africa.
You might also consider the following options of MediHelp:
- MediHelp HealthPrint
- MediHelp Medprime
- MediHelp MedPrime Elect
- MediHelp MedPlus
- MediHelp MedElite
- MediHelp MedVital
- MediHelp MedVital Elect
- MediHelp MedSaver
- MediHelp MedMove
- MediHelp MedElect
- MediHelp MedAdd Elect
MedAdd Plan Frequently Asked Questions
What is Medihelp MedAdd?
Medihelp MedAdd is a medical aid plan that provides comprehensive cover for a wide range of healthcare needs, including in-hospital treatment, chronic medication, and day-to-day medical expenses.
What does MedAdd cover?
MedAdd offers unlimited private hospital cover, chronic medication cover (subject to scheme protocols), and day-to-day benefits, such as GP consultations, specialist consultations, and diagnostic tests. It also includes emergency medical services coverage and international travel insurance.
What are the benefits of MedAdd?
The benefits of MedAdd include comprehensive coverage for a wide range of healthcare needs, unlimited private hospital coverage, full coverage for the chronic medication (subject to scheme protocols), day-to-day benefits, emergency medical services coverage, and international travel insurance.
How much does MedAdd cost?
The cost of MedAdd varies depending on several factors, such as the level of coverage required and the individual’s healthcare needs. As a result, it may be more expensive than other medical aid plans, particularly for those not requiring comprehensive coverage.
Does MedAdd cover pre-existing conditions?
MedAdd might cover pre-existing conditions, subject to certain exclusions and limitations.
What are scheme protocols?
Scheme protocols determine the level of coverage for certain medical conditions and treatments. For example, MedAdd covers chronic medication subject to scheme protocols, meaning certain conditions and medications may be excluded from full coverage.
Can I choose my own healthcare provider with MedAdd?
MedAdd allows members to choose their own healthcare providers, including doctors and specialists. However, certain benefits may be subject to network provider arrangements, which should be reviewed before joining the plan.
What is emergency medical services cover?
Emergency medical services provide financial protection for emergency medical treatment, such as ambulance services and emergency hospitalization. MedAdd includes emergency medical services coverage as part of the plan benefits.
Does MedAdd cover international travel?
MedAdd includes international travel insurance, which provides financial protection for emergency medical treatment while traveling outside South Africa.
What are value-added services?
Value-added services are additional benefits included with MedAdd at no extra cost. These services include wellness programs, lifestyle benefits, and access to health information and resources.
Does MedAdd have any exclusions or limitations?
MedAdd may have certain exclusions and limitations, such as age restrictions, waiting periods, and sub-limits for certain benefits.
What is private hospital cover?
Private hospital cover provides financial protection for in-hospital treatment at a private hospital. MedAdd offers unlimited private hospital cover, meaning members can access expensive medical treatment without worrying about a cap on benefits.
What are day-to-day benefits?
Day-to-day benefits provide financial protection for routine healthcare expenses, such as GP consultations, specialist consultations, and diagnostic tests. MedAdd offers a range of day-to-day benefits as part of the plan.
What is chronic medication cover?
Chronic medication cover provides financial protection for ongoing medication for certain medical conditions. MedAdd covers chronic medication subject to scheme protocols, meaning certain conditions and medications may be excluded from full coverage.
Can I change my MedAdd plan?
Medihelp allows members to change their MedAdd plan, subject to certain terms and conditions.
You might also like
Table of Contents
Free Medical Aid Quote
Our Trusted Partners
We work with leading medical aid companies in South Africa.

7 Actionable Ways to save 32% on your MEDICAL AID in 14 days.

- +27 72 7967 530
- [email protected]
- 2nd Floor, West Tower, Nelson Mandela Square, Sandton, 2196, Johannesburg, Gauteng, South Africa
🔎 Report a bug or outdated data to be updated to [email protected]
© Medicalaid.com | All rights Reserved |
Copyright 2024
Top 5 Medical Aids
Top 5 Gap Cover Plans
































