- Medical Aid
- Currently Trending
The Best Medical Aids
- Compare Plans
- Gap Cover
- Best Gap Covers
- Hospital Plans
- Currently Trending
The Best Hospital Plans
- Medical Insurance
- Pet Insurance
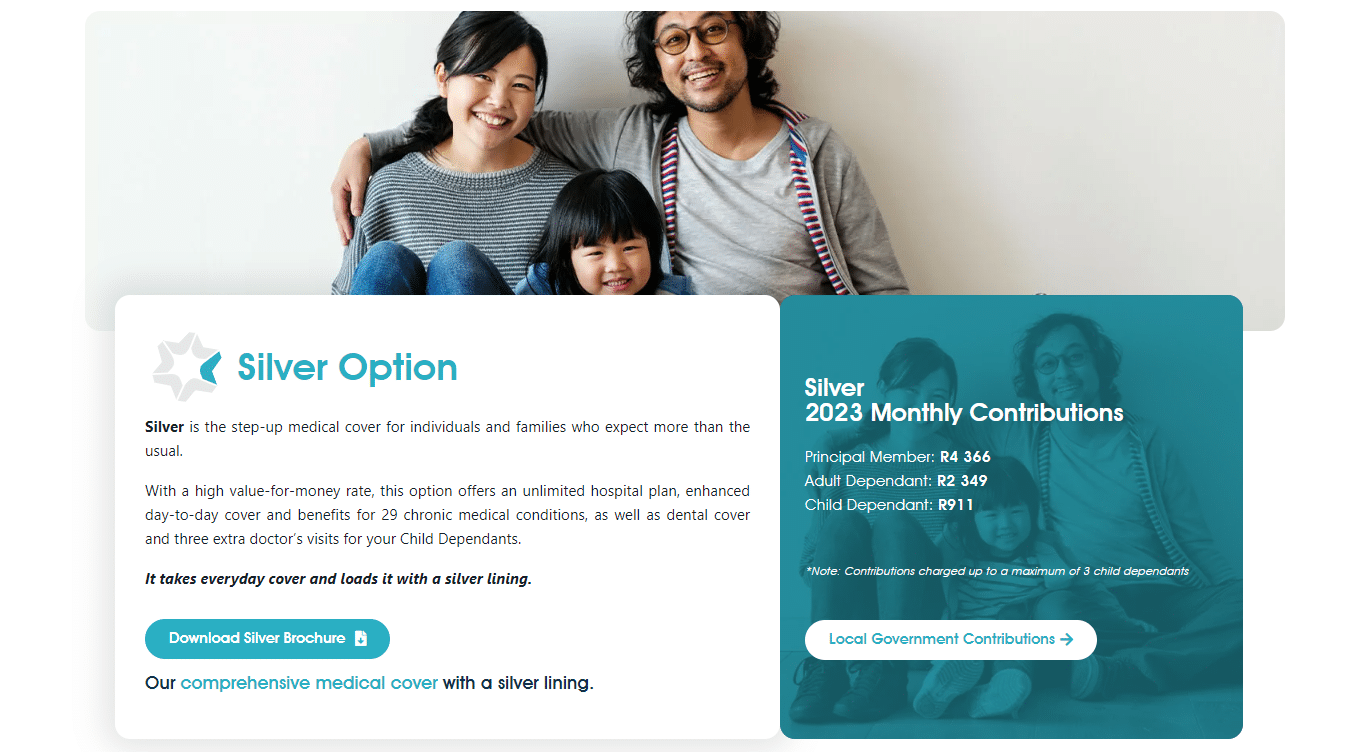
KeyHealth Silver Medical Aid Plan
Overall, the KeyHealth Silver Medical Aid Plan is a trustworthy and comprehensive medical aid plan that offers 24/7 medical emergency assistance and Gap Cover to up to 3 Family Members. The KeyHealth Silver Medical Aid Plan starts from R4,799 ZAR.
| 👤 Main Member Contribution | R4,799 |
| 👥 Adult Dependent Contribution | R2,582 |
| 🍼 Child Dependent Contribution | R1,002 |
| 🔁 Gap Cover | ☑️ Yes |
| ⚕️ Hospital Cover | Unlimited |
| 💶 Prescribed Minimum Benefits | ☑️ Yes |
| 📉 Screening and Prevention | ☑️ Yes |
| 📌 Medical Savings Account | ☑️ Yes |
| 👶 Maternity Benefits | ☑️ Yes |
| ➡️ Oncology Cover | R189,500 |
KeyHealth Silver Plan – 9 Key Point Quick Overview
- ☑️ KeyHealth Silver Plan Overview
- ☑️ KeyHealth Silver Plan Contributions
- ☑️ Silver Plan Benefits and Cover Comprehensive Breakdown
- ☑️ KeyHealth Health Booster
- ☑️ KeyHealth Smart Baby Program
- ☑️ Silver Plan Exclusions and Waiting Periods
- ☑️ KeyHealth Silver Plan vs. Similar Plans from other Medical Schemes
- ☑️ Our Verdict on The Silver Plan
- ☑️ Silver Plan Frequently Asked Questions
KeyHealth Silver Plan Overview
The KeyHealth Silver medical aid plan is one of 6, starting from R4,799 and includes an unlimited hospital plan, day-to-day cover, additional doctor visits for children, dental cover, and more. Gap Cover is available on the KeyHealth Silver Plan, along with 24/7 medical emergency assistance. According to the Trust Index, KeyHealth has a trust rating of 4.1.
KeyHealth offers 6 medical aid plans:
- ✅ KeyHealth Essence Medical Aid Plan
- ✅ KeyHealth Origin Medical Aid Plan
- ✅ Keyhealth Equilibrium Medical Aid Plan
- ✅ Keyhealth Silver Medical Aid Plan
- ✅ Keyhealth Gold Medical Aid Plan
- ✅ Keyhealth Platinum Medical Aid Plan
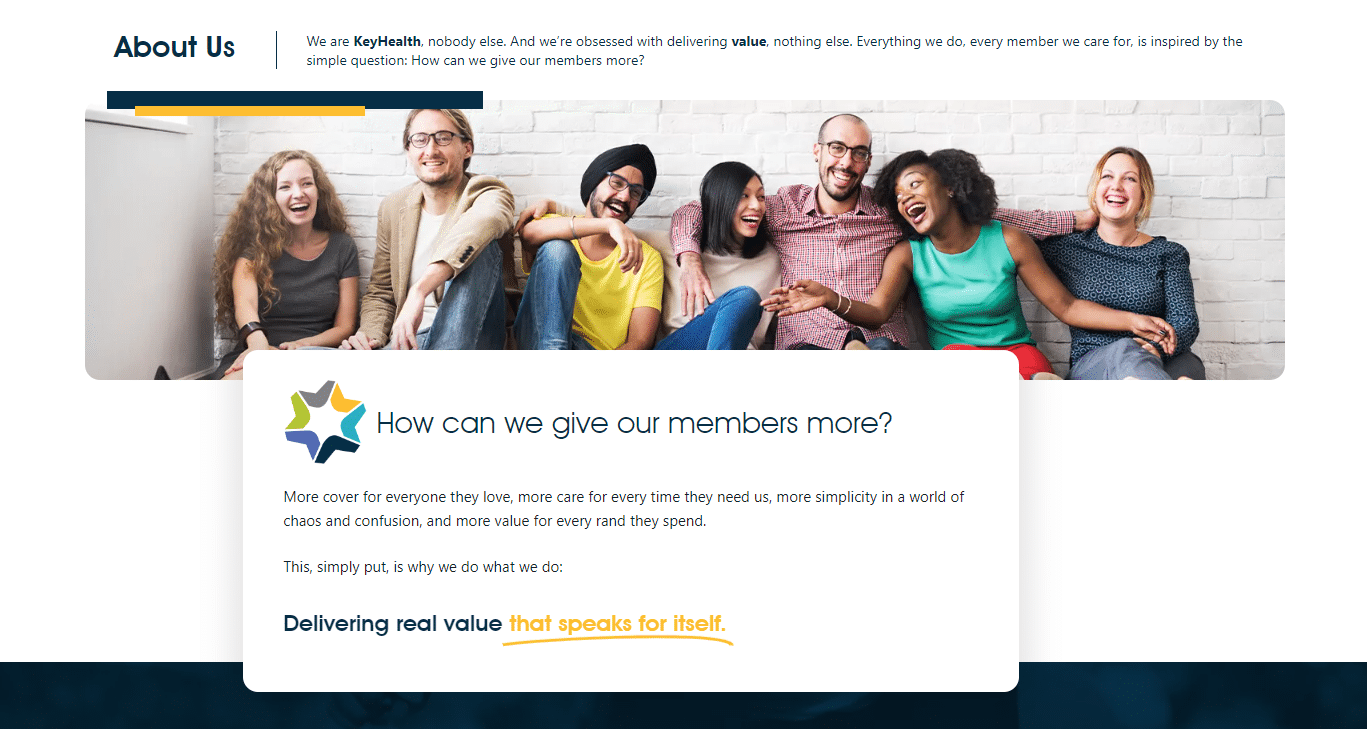
KeyHealth Silver Plan Contributions
| 👤 Main Member | 👥 Adult Dependent | 🍼 Child Dependent |
| R4,799 | R2,582 | R1,002 |
Silver Plan Benefits and Cover Comprehensive Breakdown
Silver Plan Major Medical Benefits
| 📌 Varicose vein surgery Facet joint injections Hysterectomy Rhizotomy Reflux surgery Back and Neck Surgery (including spinal fusion) Joint Replacement | Only PMBs are covered with varicose veins and reflux surgery. Other procedures are covered up to 100% of the negotiated tariff. |
| 🏥 Private Hospital Admissions | Unlimited cover. Covered up to 100% of the agreed tariff. Subject to using DSP hospitals. A 30% co-payment will apply when using a non-DSP hospital. |
| 🚑 State Hospital Admissions | Unlimited covers up to 100% of the agreed tariff. |
| ☑️ Specialist and Anesthetist Services | Covered up to 100% of the medical scheme tariff. Unlimited cover, subject to using a DSP. |
| 💊 Medication upon discharge | Limited to R575 per admission. Covered up to 100% of the medical scheme tariff. |
| 🍼 Maternity | Covered up to 100% of the medical scheme tariff. Private ward access for three days for natural birth. |
| 🩹 Sub-acute facilities and wound care Hospice Private Nursing Rehabilitation Step-down Facilities Wound Care | Limited to R32,100 per family per year. Covered up to 100% of the medical scheme tariff. Pre-approval needed. Subject to case management and scheme protocols. Wound care is included but limited to R10,300. This benefit is combined in and out-of-hospital. |
| ❤️ Organ Transplants (Solid Organs, Tissue, and Corneas) Hospitalization Harvesting Drugs for Immuno-Suppressive Therapy | Covered up to 100% of the medical scheme tariff. Pre-approval needed. Subject to case management. Only PMBs are covered in DSP hospitals. |
| 🩺 Renal Dialysis | Covered up to 100% of the medical scheme tariff. Pre-approval needed. Subject to case management and scheme protocols. Only PMBs are covered. |
| 🧪 Oncology | Covered up to 100% of the medical scheme tariff. Covered up to R169,000 per family per year. Pre-approval needed. Subject to case management and scheme protocols. Must use a DSP for treatment. |
| 📌 Palliative Care | Covered up to 100% of the medical scheme tariff. Available instead of hospitalization. Pre-approval is needed. Subject to case management and scheme protocols. |
| 📈 Radiology | Covered up to 100% of the medical scheme tariff. Pre-approval is needed for specialized radiology (MRI, CT) Hospitalization is not covered if hospitalization admission is for investigative purposes. Day-to-day benefits cover investigative admissions. |
| 📉 MRI and CT scans | Limited to R17,800 per family per year. Combined in and out-of-hospital cover. |
| ❎ X-Rays | Unlimited cover. |
| 🚩 Pathology | Covered up to 100% of the medical scheme tariff. Unlimited cover. Not covered if admission is for investigative purposes. |
Silver Plan Out-of-Hospital Benefits
| 🔎 Routine Medical Expenses GP and Specialist Consultations Radiology Prescribed and OTC medicine Optical and Auxiliary services | Covered up to 100% of the medical scheme tariff. Day-to-day benefits available: Main Member – R8,315 per year Adult Dependent – R6,045 per year Child Dependent – R1,680 per year Additional GP consults are limited to 3 per family per year after depleting available daily benefits for child dependents up to 21. |
| 💊 Over-the-counter medicine | Limited to R1,790 per family per year. Covered up to 100% of the medical scheme tariff. Subject to the day-to-day benefit. |
| 🤓 Over-the-counter reading glasses | Limited to R135 per family per year. Limited to one pair per year. Subject to the OTC medicine sub-limit. |
| 📈 Pathology | Covered up to 100% of the medical scheme tariff. Subject to the day-to-day benefit. |
| 📉 Optical Services | Limited to R1,690 per beneficiary every two years. Optical management protocols will apply. The benefit must be confirmed with the scheme. Covered up to 100% of the medical scheme tariff. |
| 👓 Frames | Limited to R560 and one frame per beneficiary every 2 years. Subject to the overall optical benefit. |
| 👁️🗨️ Lenses | Limited to 1 pair of single-vision lenses per beneficiary every 2 years. Subject to the overall optical benefit. |
| 👁️ Eye Tests | Limited to one test per beneficiary every 2 years. Subject to the overall optical benefit. |
| ➡️ Contact Lenses | Limited to R755 per beneficiary per year. Subject to the overall optical benefit. |
| 🦷 Conservative Dentistry | Subject to DENIS protocols. Managed care interventions and Scheme rules apply. Scheme Exclusions will apply. |
| 🪥 Dentistry: Consultations | Covered up to 100% of the medical scheme tariff. Two check-ups per beneficiary per year. Three specific (emergency) consultations per beneficiary per year. |
| ❎ Extra-oral X-Rays | One extra-oral x-ray per beneficiary every 3 years Covered up to 100% of the medical scheme tariff. |
| 📌 Dentistry: Preventative Care | One scale and polish treatment per beneficiary per year. Covered up to 100% of the medical scheme tariff. |
| 📍 Fillings | One per tooth every 720 days. Covered up to 100% of the medical scheme tariff. Multiple fillings require a treatment plan and X-rays. Retreatment is subject to clinical protocols. |
| 🦷 Tooth Extractions and root canal treatment | Root canal therapy on primary (milk) teeth, wisdom teeth (third molars), and direct or indirect pulp capping is excluded from treatment on this benefit. Covered up to 100% of the medical scheme tariff. |
| 🅰️ Plastic Dentures | One set per beneficiary per year. DENIS pre-approval is required. |
| 🅱️ Orthodontics (non-cosmetic and only treatment) | Covered up to 100% of the medical scheme tariff. DENIS approval is required. Cases are assessed using orthodontic indices where the function is impaired. Only one beneficiary per family can receive treatment once a year. Limited to beneficiaries between 9 and 18. |
| 😊 Maxillo-Facial and Oral Surgery | Covered up to 100% of the medical scheme tariff. DENIS protocols and Scheme rules apply. Exclusions will apply according to scheme rules. |
| 💺 Surgery in Dental Chair | Covered up to 100% of the medical scheme tariff. DENIS pre-authorization is required. Only covers the removal of impacted teeth. |
| 🏥 Surgery in-hospital with general anesthesia | Covered up to 100% of the medical scheme tariff. DENIS pre-authorization is required. Only covers the removal of impacted teeth. |
| 💤 Hospitalization and Anaesthesia | DENIS protocols and Scheme rules apply. Subject to managed care interventions. Certain exclusions will apply according to scheme rules. |
| 😴 Hospitalization and general anesthesia | Covered up to 100% of the medical scheme tariff. DENIS pre-authorization is required. Only covers the removal of impacted teeth. |
| 😷 Inhalation sedation in dental rooms | Covered up to 100% of the medical scheme tariff. DENIS pre-authorization is not required. Only covers the removal of impacted teeth. Limited to extensive dental treatment for children <5. |
| ✔️ Moderate/deep sedation in dental rooms | Covered up to 100% of the medical scheme tariff. DENIS pre-authorization is required. Only covers the removal of impacted teeth. |
Discover more about Hospital plans
Silver Plan Chronic Benefits
| 🅰️ Category A CDL | Covered up to 100% of the medical scheme tariff. Unlimited cover. Subject to reference pricing and protocols. Beneficiaries must register on the Disease Risk Program. |
| 🅱️ Category B (Other) | Covered up to 100% of the medical scheme tariff. Additional 3 non-PMB / CDL conditions are covered for children up to 21. |
Silver Plan falls within Category A of the CDL of KeyHealth and covers the following 27conditions:
- Addison’s Disease
- Asthma
- Bipolar Mood Disorder
- Bronchiectasis
- Cardiac Failure
- Cardiomyopathy Disease
- Chronic Renal Disease
- Coronary Artery Disease
- Crohn’s Disease
- Chronic Obstructive Pulmonary Disorder
- Diabetes Insipidus
- Diabetes Mellitus Type 1
- Diabetes Mellitus Type 2
- Dysrhythmias
- Epilepsy
- Glaucoma
- Hemophilia
- Hyperlipidaemia
- Hypertension
- Hypothyroidism
- Hormone Replacement Therapy (HRT)
- Multiple Sclerosis
- Parkinson’s Disease
- Rheumatoid Arthritis
- Schizophrenia
- System Lupus Erythematosus
- Ulcerative Colitis
Silver Plan covers the following additional non-PMB/CDL conditions:
- Acne
- Hyperkinesis or ADD (attention deficit disorder)
- Rhinitis
Silver Plan Supplementary Benefits
| 💗 Psychiatric Treatment | Limited to R21,500 per family per year. Covered up to 100% of the medical scheme tariff. Pre-approval is required. Subject to case management. Out-of-hospital is only covered for PMB. |
| 🩸 Blood Transfusions | Unlimited cover. Covered up to 100% of the medical scheme tariff. Pre-approval required. |
| 🦾 Prostheses Internal External Fixation Devices Implanted Devices | Limited to R6,900 per beneficiary per year. Covered up to 100% of the medical scheme tariff. Pre-approval is required, and it is subject to case management. Covered according to reference pricing. Scheme protocols will apply, and beneficiaries must use a preferred provider. |
| ⚕️ Document-Based Care (DBC) for back and neck | Covers conservative back and neck treatment instead of surgery. Covered up to 100% of the medical scheme tariff. Requires pre-authorization and will be subject to case management and scheme protocols. Only approved DBC facilities can be used. Only PMBs are covered. |
| ➡️ HIV/AIDS | Unlimited cover. Covered up to 100% of the medical scheme tariff. Must be registered with the Chronic Disease Risk Program (LifeSense) |
| 🚑 Ambulance Services | Subject to protocols. Covered up to 100% of the medical scheme tariff. |
| 👩🏻🦼 Wheelchairs Orthopaedic Appliances Incontinence Equipment | Limited to R8,200 per family per year. Covered up to 100% of the medical scheme tariff. Combined benefit for in and out-of-hospital. Subject to quantities and protocols. |
| 🫁 Oxygen Nebulizers Glucometer Blood Pressure Monitor | Pre-approval is required and will be subject to approval. |
| 🦻 Hearing aids, maintenance, and batteries | Subject to the medical appliances’ benefit |
| 📈 Endoscopic Procedures (Scopes) | Covered up to 100% of the medical scheme tariff. |
| 📉 Colonoscopy or gastroscopy | Pre-approval is required. Co-payments do not apply when using a DSP hospital and specialist for out-of-hospital services for PMB. |
| 📊 All other procedures | Pre-approval is required. Co-payments do not apply when using a DSP hospital and specialist for out-of-hospital services for PMB. |
You might consider reading about the 10 Things to Consider Before Cancelling your Medical

KeyHealth Health Booster
The KeyHealth health booster provides members additional benefits for preventative treatment. This includes free screening tests, among several other features, as seen in the benefits table below.
| 🍼 Baby Immunisation | Child dependents <6 years. According to the Department of Health schedule. |
| 💉 Flu Vaccination | All beneficiaries are covered. |
| 😷 COVID-19 Vaccination | All beneficiaries are covered. |
| ☑️ Tetanus-Diphtheria Injection | All beneficiaries are covered when needed. |
| ✅ Pneumococcal Vaccination | All beneficiaries are covered. |
| 🦟 Malaria Medication | All beneficiaries are covered. Limited to R440 per year. |
| 📌 HPV vaccination | Two doses per lifetime for female beneficiaries between 9 and 14. |
| 🚼 Baby Growth Assessment | Three yearly assessments at a pharmacy or baby clinic for babies <35 months. |
| 🩹 Contraceptive Medication – Tablets and Patches | Limited to R175 every 20 days. Female beneficiaries 16> |
| 💉 Contraceptive Medication – Injectables | Limited to R270 every 20 days. Female beneficiaries 16> |
| 📈 Pap Smear (Pathology) | Once per year. Female beneficiaries 15> |
| 📉 Pap Smear Consultation Pelvic Organs Ultrasound | Once per year. Female beneficiaries 15> |
| 📊 Mammogram | Once per year. Female beneficiaries 40> |
| ✳️ Prostate Specific Antigen (PSA) | Once per year. Male beneficiaries 40> |
| 📎 HIV/AID Tests | Once per year. All beneficiaries are covered. |
| 💙 Health Assessment Body Mass Index (BMI) Blood Pressure Measurement Cholesterol Test (Finger prick) Blood Sugar Test (Finger prick) PSA (Finger Prick) | Once per year. All beneficiaries are covered. |
| ➡️ Weight Loss Program | Beneficiaries with a BM of 30> will receive the following: Three dietician consultations (one per week) One biokinetics consultation. Three additional dietician consultations per week if a weight loss chart was received, proving weight loss after the first three weeks. One follow-up with biokinetics. |
| 👩⚕️ Antenatal Visits to a GP, Gynaecologist, or midwife and a Urine Test | Pre-notification and pre-approval are needed. Twelve visits are covered. |
| 👨⚕️ Ultrasounds – one before the 24th week and one after | Pre-notification and pre-approval are needed. Limited to two scans per pregnancy. |
| 💵 Short Payments / Co-payments for services rendered and birthing fees | Covered up to 1,290 per pregnancy. |
| 🍼 Paediatrician Visits | The baby must be registered on the scheme. Limited to 2 visits within the baby’s first year and one in the second year. |
| 💊 Antenatal Vitamins | Limited to R2,180 per pregnancy. |
| 🧡 Antenatal Classes | Limited to R2,180 for the first pregnancy. |
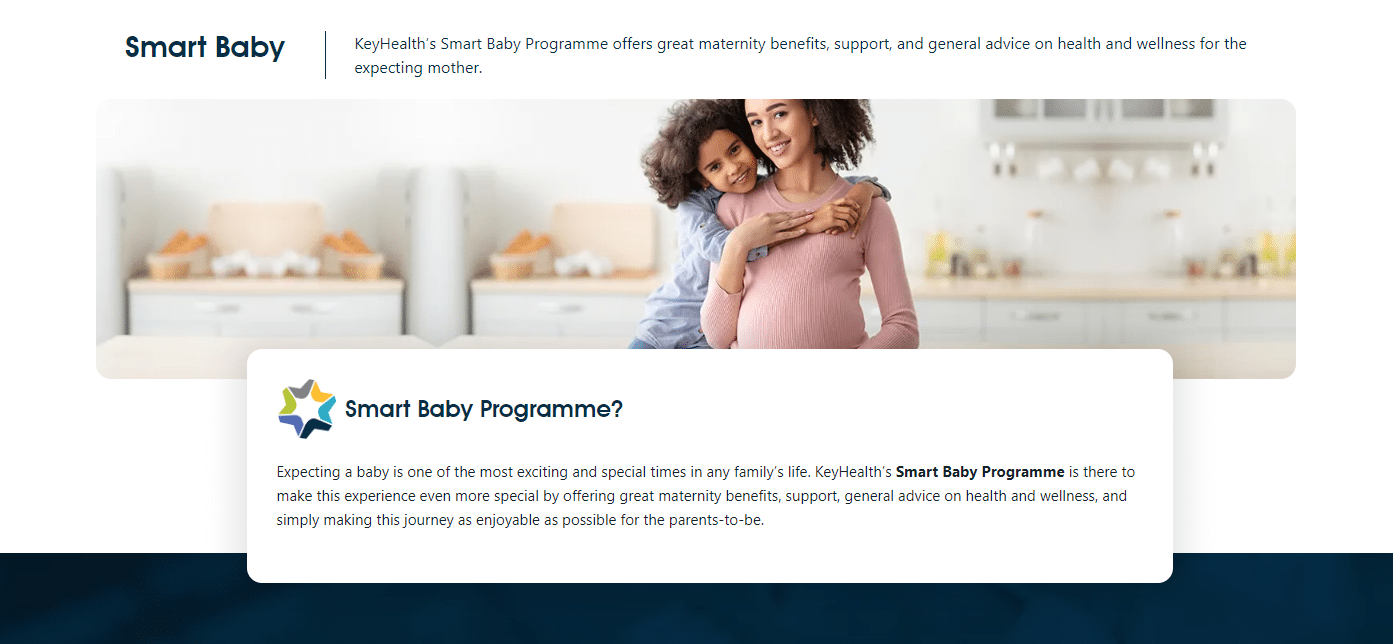
KeyHealth Smart Baby Program
The Smart Baby Programme by KeyHealth provides expecting mothers and fathers with general guidance and support on health and well-being throughout the pregnancy while ensuring peace of mind.
Smart Baby Program Features
- Coverage under Health Booster for antenatal visits (GP, gynecologist, or midwife), scans, and birthing fees that require short/co-payments.
- Provision of KeyHealth’s maternity benefits and instructions on how to access them.
- The New Baby and Childcare Handbook, authored by Marina Petropulos, is specifically for first-time parents.
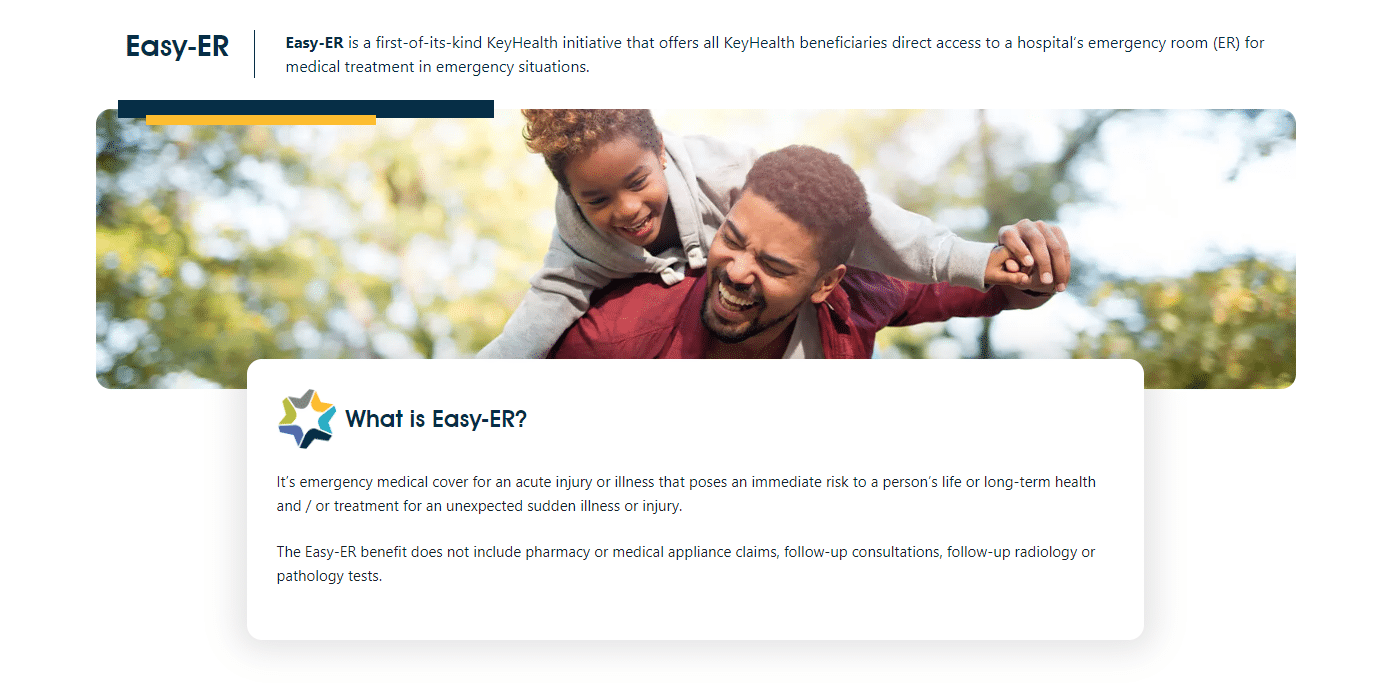
- Information on the initial year of the baby’s life, including vaccinations, Easy-ER, and other details.
- Availability of Netcare 911’s 24-hour Health-on-Line service at 082 911 for medical advice and insights from a registered nurse.
Discover: 5 Best Private Hospitals to Give Birth
Smart Baby Program Benefits
The Smart Baby Programme benefits accessible to women (and babies) are distinct from day-to-day benefits and medical savings accounts.
| 👶 Antenatal visits | Twelve visits, one of which is after the birth. |
| 💙 Ultrasounds | Limited to two pregnancy ultrasounds. |
| 🍼 Paediatrician Visits (after the baby is a registered beneficiary) | Limited to two visits in the baby’s first year. |
| 💊 Antenatal vitamins | Limited to R2,320 per pregnancy. |
| ➡️ Antenatal classes | Limited to R2,320 per pregnancy. |
Silver Plan Exclusions and Waiting Periods
Exclusions
The KeyHealth Silver Plan has specific exclusions, including:
- Acupuncture
- Bio-stress assessments
- Colonic irrigation
- Conservative back/neck treatment in the hospital
- Cosmetic / non-functional procedures
- DNA testing
- Gender reassignment
- Industrial and educational psychologists
- IQ tests and learning or educational problems
- Music and water therapy
- Obesity and weight loss surgery (excluding benefits available on the Health Booster)
- Polysomnogram and titration (sleep study)
Waiting Periods
If a Principal Member or their dependent is diagnosed with a specific illness, the Scheme reserves the right to exclude benefits for this condition for 12 months. Subject to the regulations, KeyHealth can impose waiting periods on an individual who applies for membership or admission as a dependent and has not been a beneficiary of a medical scheme for a minimum of 90 days before the application date. Such waiting periods may include the following:
- A general waiting period of up to 3 months also encompasses PMB conditions.
- A condition-specific waiting period of up to 12 months, including PMB conditions.
If an individual who applies for membership or admission as a dependent was previously a beneficiary of a medical scheme for a continuous period of up to 24 months, which ended less than 90 days before the application date, Keyhealth could impose the following:
- A condition-specific waiting period of up to 12 months, except for any treatment or diagnostic procedures covered within PMB conditions.
If the previous medical scheme had imposed a general or condition-specific waiting period on such an individual, and the waiting period had not expired at the time of termination, Keyhealth could impose a waiting period for the remaining duration as imposed by the previous medical scheme. However, any child born into the Scheme during membership will not be subject to waiting periods. Furthermore, Keyhealth can impose the following:
- A general waiting period of up to 3 months, except for any treatment or diagnostic procedures covered within PMB conditions, on any person who applies for membership or admission as a dependent and was previously a beneficiary of a medical scheme for a continuous period of more than 24 months, which ended less than 90 days before the application date.
POLL: 5 Best Medical Aids under R3000
Medical Aid Comparisons : KeyHealth Silver Plan vs. Similar Plans from other Medical Schemes
| 🔎 Medical Aid Plan | 🥇 KeyHealth Silver | 🥈 GEMS Emerald | 🥉 Momentum Custom |
| 🌎 International Cover | ☑️ Yes | ☑️ Yes | ☑️ Yes |
| 👤 Main Member Contribution | R4,799 | R | R |
| 👥 Adult Dependent Contribution | R2,582 | R | R |
| 🍼 Child Dependent Contribution | R1,002 | R | R |
| ⚕️ Hospital Cover | Unlimited | Unlimited | Unlimited |
| 🔍 Oncology Cover | R189,500 | R242,300 | R300,000 |
| 💶 Prescribed Minimum Benefits | ☑️ Yes | ☑️ Yes | ☑️ Yes |
| 📉 Screening and Prevention | ☑️ Yes | ☑️ Yes | ☑️ Yes |
| 💙 Medical Savings Account | ☑️ Yes | None | None |

Our Verdict on The Silver Plan
KeyHealth Silver is a medical aid plan offered by KeyHealth Medical Scheme that provides comprehensive healthcare coverage to its members. The plan is designed to cater to individuals and families requiring affordable healthcare services without compromising on quality. One of the key features of the KeyHealth Silver plan is its unlimited hospital coverage. This means that members can access private hospitals without any limit on the cost of their hospital stay. The plan also provides unlimited coverage for chronic conditions such as HIV/AIDS, diabetes, and hypertension. In addition to hospital cover, the KeyHealth Silver plan offers a range of benefits, including comprehensive primary care, specialist consultations, and prescription medication. The plan also covers a range of diagnostic tests and procedures, including X-rays, blood tests, and MRI scans. Furthermore, it is also a great option for families, as the plan covers up to four children under 21.
However, the KeyHealth Silver plan also has some unique drawbacks. One is the limited day-to-day benefit, which only covers essential healthcare services such as GP consultations, dentistry, and optometry. This means that members may need to pay for additional healthcare services out of their own pocket. But overall, the KeyHealth Silver plan is an excellent option for individuals and families who require comprehensive healthcare coverage at an affordable price. While it may have some limitations, the plan provides excellent value for money. As a result, it is an excellent choice for those seeking quality healthcare services in South Africa.
You might also like: KeyHealth Equilibrium
You might also like: KeyHealth Essence
You might also like: KeyHealth Gold
You might also like: KeyHealth Origin
You might also like: KeyHealth Platinum
Silver Plan Frequently Asked Questions
What is KeyHealth Silver?
KeyHealth Silver is a medical aid plan offered by KeyHealth Medical Scheme that provides comprehensive healthcare coverage to its members.
What benefits does KeyHealth Silver offer?
KeyHealth Silver offers unlimited hospital coverage for chronic conditions, primary care, specialist consultations, prescription medication, and cover for diagnostic tests and procedures such as X-rays, blood tests, and MRI scans.
Is KeyHealth Silver affordable?
No, KeyHealth Silver might not be affordable for all families or individuals. Contributions from R4,799 might be more than many can afford. Furthermore, the premium is much higher than medical aid plans with similar benefits.
What is the day-to-day benefit of KeyHealth Silver?
The day-to-day benefit of KeyHealth Silver covers essential healthcare services such as GP consultations, dentistry, and optometry, but it is limited.
Can families be covered under KeyHealth Silver?
Yes, KeyHealth Silver covers up to four children under 21, making it a great option for families.
Does KeyHealth Silver have any limitations?
One limitation of KeyHealth Silver is its limited day-to-day benefit, meaning members may need to pay for additional healthcare services out of their own pocket.
Is KeyHealth Silver a good option for individuals and families seeking comprehensive healthcare coverage?
Yes, KeyHealth Silver is an excellent option for individuals and families who require comprehensive healthcare coverage at an affordable price.
You might also like
Table of Contents
Free Medical Aid Quote
Our Trusted Partners
We work with leading medical aid companies in South Africa.

7 Actionable Ways to save 32% on your MEDICAL AID in 14 days.

- +27 72 7967 530
- [email protected]
- 2nd Floor, West Tower, Nelson Mandela Square, Sandton, 2196, Johannesburg, Gauteng, South Africa
🔎 Report a bug or outdated data to be updated to [email protected]
© Medicalaid.com | All rights Reserved |
Copyright 2024
Top 5 Medical Aids
Top 5 Gap Cover Plans
































