- Medical Aid
- Currently Trending
The Best Medical Aids
- Compare Plans
- Gap Cover
- Best Gap Covers
- Hospital Plans
- Currently Trending
The Best Hospital Plans
- Medical Insurance
- Pet Insurance
Discovery Health Classic Priority Medical Aid Plan
Overall, the Discovery Health Classic Priority Medical Aid Plan is a trustworthy and comprehensive medical aid plan that offers 24/7 medical emergency assistance and flexible coverage to up to 3 Family Members. The Discovery Health Classic Priority Medical Aid Plan starts from R5,272 ZAR.
| 🔎 Medical Aid Plan | 🥇 Classic Priority |
| 👤 Main Member Contribution | R5,272 |
| 👥 Adult Dependent Contribution | R4,158 |
| 🍼 Child Dependent Contribution | R2,108 |
| 🔁 Gap Cover | ✅ Yes |
| 💙 Medical Savings Account | ✅ Yes |
| 👶 Maternity Benefits | ✅ Yes |
| ➡️ Pre- and Postnatal Care | ✅ Yes |
| ↪️ Extended Cover for Oncology | None |
| 💶 Hospital Cover | Unlimited |

Discovery Health Classic Priority – 22 Key Point Quick Overview
- ✅ Discovery Health Classic Priority Overview
- ✅ Discovery Health Classic Priority Contributions, Medical Savings Account, ATB, and Annual Threshold
- ✅ Discovery Health Priority Plan Benefits Summarized
- ✅ Discovery Health Classic Priority Benefits and Cover Comprehensive Breakdown
- ✅ Discovery WELLTH Fund
- ✅ Discovery Health WHO Outbreak Benefit
- ✅ Discovery Health Connected Care
- ✅ Discovery Health Hospital At Home
- ✅ Discovery Health Priority Day-to-Day Benefits
- ✅ Discovery Maternity and Early Childhood Benefits
- ✅ Discovery Health Chronic Benefits
- ✅ Discovery Health Care Programs
- ✅ Discovery Health Comprehensive Cancer Cover
- ✅ Discovery Health Hospital Benefit
- ✅ Discovery Health Annual Limits
- ✅ Discovery Health Priority Cover for Day Surgery Network Procedures
- ✅ Discovery Health Priority Additional Benefits
- ✅ Discovery Classic Priority Value-Added Offers
- ✅ Discovery Health Classic Priority Exclusions and Waiting Periods
- ✅ Discovery Health Classic Priority Plan vs Similar Plans from Other Medical Schemes
- ✅ Our Verdict on Discovery Health Classic Priority
- ✅ Discovery Health Classic Priority Frequently Asked Questions
Discovery Health Classic Priority Overview
The Discovery Health Classic Priority starts from R5,272 and is part of a series of comprehensive medical insurance plans offered by Discovery Health. The Classic Priority plan provides comprehensive and flexible coverage for medical expenses, with a range of preventative healthcare benefits and unlimited hospital cover. The Discovery Classic Priority provides an elevated level of cover for in-hospital expenses, day-to-day benefits, chronic medication, and other medical expenses. Gap Cover is available on the Discovery Health Classic Priority, along with 24/7 medical emergency assistance. According to the Trust Index, Discovery Health has a trust rating of 4.8.
Discovery Health Priority Series has two plans namely Discovery Health Classic Priority and Discovery Health Essential Priority
Discovery Health Classic Priority Contributions, Medical Savings Account, ATB, and Annual Threshold
Classic Priority Monthly Contributions
| 👤 Main Member | 👥 +1 Adult Dependent | 🍼 +1 Child Dependent |
| R5,272 | R4,158 | R2,108 |
Classic Priority Medical Savings Account (MSA)
| 👤 Main Member | 👥 +1 Adult Dependent | 🍼 +1 Child Dependent |
| R15,792 | R12,456 | R6,312 |
Classic Priority Annual Threshold Amount
| 👤 Main Member | 👥 +1 Adult Dependent | 🍼 +1 Child Dependent |
| R22,890 | R17,210 | R7,620 |
Classic Priority Limited Above-Threshold Benefit Amount (ATB)
| 👤 Main Member | 👥 +1 Adult Dependent | 🍼 +1 Child Dependent |
| R19,370 | R13,820 | R6,770 |
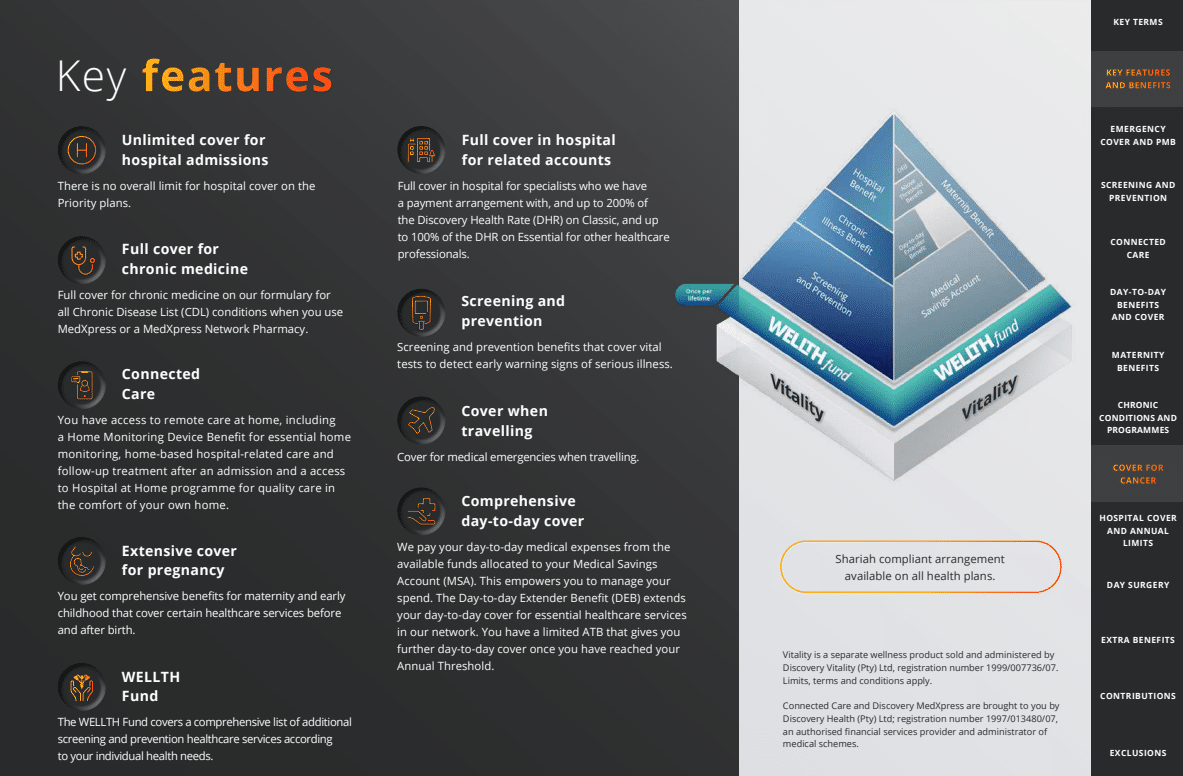
Discovery Health Priority Plan Benefits Summarized
| 🅰️ Classic Priority | – |
| 🅱️ Day-to-Day Cover | – |
| 🟥 Medical Savings Account (MSA) | 25% of the monthly contribution |
| 🟥 Day-to-Day Extender Benefit | The Discovery Health wellness network’s Day-to-Day Extender Benefit (DEB) covers essential healthcare services. You are also covered for child casualty visits. |
| 🅰️ Hospital Cover | – |
| 🟥 Cover for healthcare professionals in the hospital | Covered up to 200% of the Discovery Health Rate (DHR) |
POLL: 5 Best Hospital Plans under R500

Discovery Health Classic Priority Benefits and Cover Comprehensive Breakdown
Emergency Cover
In case of a traumatic incident or after a traumatic event, you can get help from a trained professional. Calling Emergency Assist will help you and your loved ones in need. Furthermore, family members can get help after a traumatic event at any time. The survivors of gender-based violence can receive counseling and other support as part of this service.
Discovery Health Emergency Cover covers the following medical services:
- The emergency vehicle (or other medical transport).
- The hospital’s account of the incident.
- The observations of the physician who admitted you to the hospital.
- The anesthesiologist.
Any additional approved healthcare provider.
Prescribed Minimum Benefits
All medical schemes are required by the Prescribed Minimum Benefit (PMB) provisions of the Medical Schemes Act 131 of 1998 and its Regulations to cover the costs associated with the diagnosis, treatment, and care of:
- A life-threatening medical condition
- A defined listing of 271 conditions
- A list of 27 chronic illnesses.
Your medical condition must be on the Prescribed Minimum Benefit (PMB) conditions list to qualify for coverage. Furthermore, the necessary treatment must correspond to the treatments listed in the benefits. In addition, you are required to utilize designated service providers (DSPs) within the Discovery Health network. Once your condition has stabilized, you will be transferred to a hospital or other service providers in the Discovery Health network, if necessary, according to the scheme’s rules. Discovery Health will cover up to 80% of the Discovery Health Rate if you do not use a DSP (DHR). Your responsibility will be the difference between what Discovery Health will pay and the actual cost of your treatment. Furthermore, Discovery Health will pay according to your plan’s benefits if these criteria are unmet.
You might consider the 5 Best Medical Aids under R1000
Screening and Prevention
This benefit covers certain diagnostic procedures that detect early warning signs of serious diseases. The Discovery Health wellness providers cover a variety of screening tests, including blood glucose, cholesterol, HIV, Pap smear or HPV test for cervical screening, mammograms or ultrasounds, and prostate screenings. After all your membership members have completed their health check, you can access additional screening and preventive healthcare services through the WELLTH Fund.
The Discovery Health Screening and Prevention covers the following:
- Screening for kids will assess the child’s growth and development, including weight, height and body mass index measurements, blood pressure, and more.
- Screening for Adults includes blood pressure, blood glucose, HIV, and more. Discovery also covers mammograms, breast ultrasounds, pap smears, and more.
Screening for Seniors (65>) includes risk screening assessments and referrals to Premier Plus GPs according to the screening results.

Discovery WELLTH Fund
The WELLTH Fund covers a comprehensive list of screening and prevention healthcare services to empower you to act based on your individual health requirements. This benefit is distinct from and in addition to the Screening and Prevention Benefit; it is available once per lifetime to all members and dependents who have completed their health checks. Your WELLTH Fund can be used up to its maximum for screening and prevention services. However, the cover is subject to the Scheme’s clinical entry requirements, treatment protocols, and guidelines.
The Discovery Health WELLTH Fund for Classic Priority covers the following:
| 🩺 General Health | You can access screenings for vision, hearing, dental, and skin conditions as part of your primary care. Additionally, you are eligible for one GP screening consultation |
| ⚽ Physical Health | Dieticians, biokinetics, or physiotherapists are available for physical well-being evaluations. |
| 🧠 Mental Health | You have access to a mental health evaluation to promote mental health. |
| 💜 Women and Men’s Health | You have access to various screening and prevention services for women and men. These include, for instance: Consultation with your doctor for gynecological, prostate, or cardiac issues Bone density analysis |
| 💗 Children’s Health | A pediatrician, speech pathologist, or physiotherapist can evaluate your child’s progress toward important developmental milestones as part of a well-child check-up. |
| 📌 Medical Monitoring Devices | You have access to medical monitoring devices that assist in measuring, for instance, blood pressure, cholesterol, and blood sugar. |
The WELLTH Fund is available for two benefit years after all beneficiaries over two complete an age-appropriate health check with a Wellness Network provider. Furthermore, the benefit is available to new members in the joining year and subsequent years. The benefit is available once per lifetime per beneficiary. Cover for eligible healthcare services is limited to the Discovery Health Rate (DHR), subject to the overall benefit maximum.
Your WELLTH Fund maximum is based on the size and composition of your family as stated in your policy:
- ✅ Limited to R2,500 per adult dependent.
- ✅ Limited to R1,250 per two-year-old or older child dependent.
- ✅ Limited to R10,000 per family.
Furthermore, the WELLTH Fund is available to all registered membership beneficiaries and will not cover healthcare services already covered by other defined benefits.

Discovery Health WHO Outbreak Benefit
The basket of care includes the following:
- ✅ COVID-19 vaccines and their administration according to the COVID-19 guidelines of the National Department of Health.
- ✅ Screening consultations with a network general practitioner (virtual, telephone, or in-person).
- ✅ COVID-19 PCR and Rapid Antigen screening tests if referred by a qualified medical practitioner.
- ✅ A set of defined pathology tests for COVID-19-positive individuals.
- ✅ A predetermined assortment of x-rays and scans for COVID-19-positive individuals.
- ✅ Members at risk who meet the clinical entry criteria will receive supportive care, including medication and a home monitoring device to track oxygen saturation levels.
- ✅ When you are admitted to the hospital because of symptoms of COVID-19, you will be covered by the Hospital Benefit of the Classic Priority and, if necessary, the PMBs.
- ✅ Access to the Long COVID Recovery Program.
How members of the Discovery Health Classic Priority are covered in terms of Monkeypox:
- ✅ The treatment protocol for confirmed cases consists of a diagnostic PCR screening test
- ✅ Two visits to a dermatologist or general practitioner.
Formulary of supportive medications for pain management.
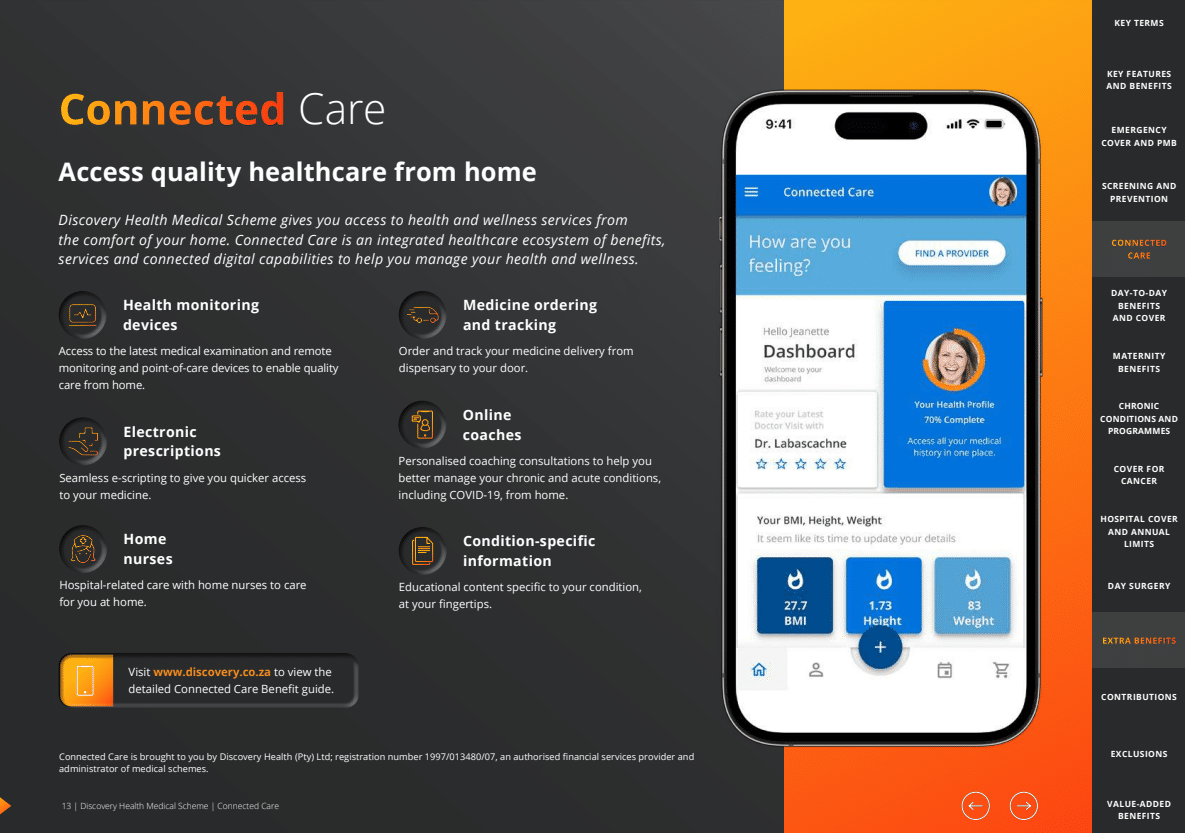
Discovery Health Connected Care
Discovery Health Medical Scheme provides home-based access to health and wellness services. Connected Care is an integrated ecosystem of benefits, services, and digitally connected capabilities designed to assist you in managing your health and wellness.
| 🟥 Health Monitoring Devices | Access to the most up-to-date medical examination, remote monitoring, and point-of-care devices to facilitate the delivery of quality care at home. |
| 🟧 Electronic Prescriptions | Electronic prescribing for expedited access to medications. |
| 🟨 Home Nurses | Hospital-related care is provided at home by registered nurses. |
| 🟩 Medicine Ordering and Tracking | Order and track the delivery of your medication from the dispensary to your door. |
| 🟦 Online Coaches | At-home consultations with a coach to help you better manage your chronic and acute conditions, including COVID-19. |
| 🟪 Condition-Specific Information | Educational content pertinent to your condition is readily accessible. |
✅ Connected care for members at home
Previously unimaginable access to medical professionals is now at your fingertips, thanks to the advent of online consultations. Thanks to the Home Monitoring Device Benefit, you can get various approved home monitoring devices for chronic and acute conditions. You will not see any changes to your regular benefits because of having cover approved for these gadgets.
✅ Connected care for those with chronic conditions
Through Connected Care, you and your doctor can work together to keep your chronic condition under control while you are at home. Eligible members can use various digital services connected to Priority remote monitoring, point-of-care devices, and individualized coaching consultations to monitor and control their chronic condition in the comfort of their homes.
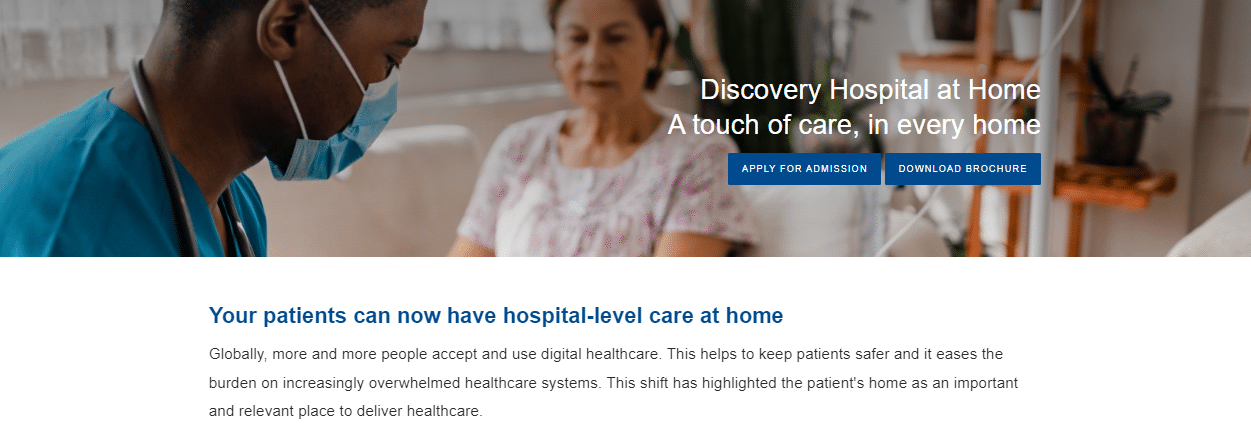
Discovery Health Hospital At Home
Hospital at Home patients receive specialized care from a dedicated medical staff in the comfort of their own homes. Each of these benefits and services contributes to your overall health and well-being. They all work together to make your healthcare more efficient and your life safer. Suppose you have a valid pre-authorization for hospitalization. In that case, Discovery Health will use your Hospital Benefit to cover any services provided as part of Discovery’s Hospital at Home program. For those who meet the program’s clinical and benefit criteria, this unlocks cover for approved medical devices and services.
Furthermore, Discovery Health covers the following:
- 24/7 clinical oversight from a care team virtually, including nurses, doctors, and allied healthcare professionals.
- 24/7 real-time remote monitoring, which is supported by innovative healthcare technology.
- Hospital-level diagnostics and intervention to manage post-surgical or medical care at home.
✅ Acute Care at home
This includes cover and treatment for COVID-19, as well as post-discharge care. In addition, you are eligible for the Home Monitoring Device Benefit.
✅ Home Monitoring Devices
- Suppose you meet the Scheme’s clinical entry criteria. In that case, you have healthcare coverage up to a limit of R4,250 per person per year at 100% of the Discovery Health Rate (DHR) for monitoring certain conditions like chronic obstructive pulmonary disease, congestive heart failure, diabetes, pneumonia, and COVID-19.
- If you meet the clinical entry criteria, the Scheme also covers up to 75% of the Discovery Health Rate (DHR) for defined point-of-care medical devices. You are responsible for 25% of the total cost of these devices. In addition, you have access to the most advanced remote medical examination device, known as TytoHome.
- TytoHome enables you to conduct a medical examination by transmitting throat, ear images, and heart and lung sound to your doctor in real time.
✅ Home Care Cover
- Discovery Home Care is a service that provides you with high-quality care in the comfort of your own home if your doctor recommends it as an alternative to hospitalization. Postnatal care, end-of-life care, intravenous infusions (drips), and wound care are provided. These services are covered by the Hospital Benefit, pending authorization.
- Discovery Home Care is the designated service provider (DSP) for intravenous infusion administration. Use Discovery Home Care for these infusions to avoid a 20% co-payment.
✅ Home-based care for follow-up treatment after hospital admission
- Once discharged from the hospital, patients with clinically appropriate conditions such as chronic obstructive pulmonary disease, chronic cardiac failure, ischemic heart disease, and pneumonia have access to enhanced home-based care.
If you meet the clinical entry criteria, you are covered for bedside medicine reconciliation before admission discharge, a follow-up consultation with a GP or specialist, and a defined basket of supportive care at home, including in-person and virtual consultations with a Discovery Home Care nurse.
Discover the 5 Best Medical Aid with Immediate Cover (No Waiting Period)
Discovery Health Priority Day-to-Day Benefits
Discovery Health will cover your day-to-day medical expenses with funds from your Medical Savings Account (MSA) or Day-to-Day Extender Benefit (DEB).
✅ The Medical Savings Account (MSA)
Discovery Health pays for the day-to-day medical expenses of its members, such as consultations with GPs and specialists, medicine (excluding registered chronic medicine), radiology, and pathology, from the available funds in the member’s Medical Savings Account (MSA). Any unused funds will be carried over to the next year. In addition, members can have their claims paid at the Discovery Health Rate (DHR) or at cost. If the member chooses to have their claims paid at cost and the claims exceed the DHR, the Scheme will automatically fund the excess from the MSA. If the member chooses to have their claims paid at the DHR and wishes to have claims paid more than the DHR from the available funds in their MSA, they can request a special payment.
✅ The Day-to-Day Extender Benefit (DEB)
Pays for daily benefits after your MSA runs out but before the Annual Threshold. Covers wellness network pharmacy clinic and GP video call consultations. After a video call or pharmacy clinic virtual GP referral, you have unlimited face-to-face network GP consultations. Furthermore, Discovery will cover Discovery Health Rate face-to-face consultations (DHR). Kids under 10 get two casualty visits a year on the Classic plan.
✅ The Self-payment Gap (SPG)
If your MSA expires before you reach your Annual Threshold, you must pay for claims until you reach it. You must keep sending in claims during the SPG so we can track your Annual Threshold.
✅ The Above Threshold Benefit (ATB)
Over Threshold After your Annual Threshold, the benefit covers daily expenses. Some claims do not meet your Annual Threshold or ATB payment:
- Medicine that you do not need a prescription for (over-the-counter medicine)
- Childhood vaccines and immunizations
- Lifestyle-enhancing products
- Claims more than the Discovery Health Rate (DHR).
- Claims paid more than annual benefit limits.
Furthermore, the limited Above Threshold Benefit (ATB) covers daily expenses at the Discovery Health Rate (DHR) or a portion. Benefit limits apply, and any difference between the DHR and the amount claimed. Any amount over the annual benefit limit or ATB limit must be paid. The tables below illustrate how much we cover your routine healthcare costs under the Priority plans. When you file a claim, the following amounts are added to determine your Annual Threshold.

Discovery Maternity and Early Childhood Benefit
With the Discovery Health Classic Priority, you get coverage for healthcare services related to your pregnancy and treatment for the first two years of your baby’s life. This applies from the date of activation of the benefit for each pregnancy and each child from birth until they are two years old. Discovery Health Maternity Benefit covers the following:
✅ During Pregnancy:
- Scans and Screenings
- Eight antenatal consultations with a midwife, GP, or gynecologist.
- 2 x 2D ultrasound scans
- Nuchal translucency test
- 3D and 4D scans up to the 2D scan rate.
- Non-invasive Prenatal Test (NIPT)
- One flu vaccination during pregnancy.
- Discovery Health will cover predetermined blood tests to confirm your pregnancy.
READ more about Health Insurance for Pregnancy
✅ After giving birth, Discovery Health covers the following:
- GP and Specialist help for up to 2 years.
- Postnatal care, including complications during delivery, nutritional assessment, etc.
Discovery Health’s prenatal and postnatal care includes Five antenatal or postnatal classes and One Breastfeeding consultation.

Discovery Health Chronic Benefits
The Chronic Disease List lists 27 conditions for which the Chronic Illness Benefit (CIB) provides cover (CDL).
✅ Discovery Health pays for consultations and medicines in the following ways:
You must select a primary care physician from the Discovery Health Network to manage your chronic conditions. You must see a Discovery Health Network physician to receive full coverage for your doctor visits. Use of a non-network primary care physician will incur a 20% co-payment. Discovery Health will pay up to the Discovery Health Rate (DHR) for medications purchased at one of the network pharmacies. The DHR for medication consists of the price of the medication and the dispensing fee.
✅ Medicine covered in terms of the chronic disease list (CDL):
You have coverage for all chronic medications on the approved list. Discovery Health covers you for medications, not on the list up to the Chronic Drug Amount monthly maximum (CDA).
Discovery Health Classic Priority Full List of conditions covered:
- Addison’s disease
- Asthma
- Bipolar mood disorder
- Bronchiectasis
- Cardiac failure
- Cardiomyopathy
- Chronic obstructive pulmonary disease
- Chronic renal disease
- Coronary artery disease
- Crohn’s disease
- Diabetes insipidus
- Diabetes Type 1
- Diabetes Type 2
and many more.
Chronic Medicine
Utilize our designated service providers (DSPs), MedXpress and MedXpress Network Pharmacies, to avoid paying a 20% co-payment on your chronic medication. Through MedXpress, you can order or reorder your medication online and have it delivered to your place of business or residence. Alternatively, you can:
- You can order your medication online and pick it up at a MedXpress Network Pharmacy or
- Fill a prescription as usual at any pharmacy in the MedXpress Network.
✅ Medicine Tracker
You can set reminders and prompts to help you take your medication as prescribed and on time. For example, your approved chronic medication will be displayed automatically, and you will be prompted to take your medication and confirm each dose.

Discovery Health Care Programs
Discovery Health will cover preventative and condition-specific care programs that assist with managing diabetes, mental health, HIV, and heart-related conditions. You must be registered with these condition-specific care programs to access additional benefits and services. On a personalized dashboard, you and your Premier Plus GP can identify the next steps to manage your condition and optimally maintain your health over time.
| 🔴 Discovery Health Disease Prevention Program | Priority Premier Plus GPs can enroll you in the Disease Prevention Program if you have cardiometabolic risk syndrome. GPs, dietitians, and health coaches coordinate care. Consultations, pathology tests, and medicine are covered for enrolled members. Health coaching will help you manage your condition daily. |
| 🟠 Discovery Health Mental Health Care Program | Once enrolled by your network psychologist or Priority Premier Plus GP, you have defined major depression cover. The program provides medication coverage, virtual and in-person psychotherapy, and additional GP visits for treatment evaluation, tracking, and monitoring. Relapse prevention programs cover psychiatry consultations, counseling, and care coordination for qualifying members. |
| 🟡 Discovery Health Diabetes Care Program | Your Priority Premier Plus GP can enroll you in the Diabetes Care Program if you receive the Chronic Illness Benefit (CIB) for diabetes. The program covers extra glucometer strips and dietitian and biokinetics visits. A nurse educator can help you manage your condition. |
| 🟢 Discovery Health HIV Care Program | Your Priority Premier Plus GP registers you on the HIV program, which includes social worker cover. Confidentiality is guaranteed. Avoid a 20% co-payment by getting your medicine from a DSP. |
| 🔵 Discovery Health Cardio Care Program | If referred by your Priority Premier Plus GP and enrolled in the Cardio Care Program, you can receive a defined basket of care and an annual cardiovascular assessment for hypertension, hyperlipidemia, or ischemic heart disease on the Chronic Illness Benefit (CIB). |
The cover is subject to the Scheme’s clinical entry requirements, treatment protocols, and guidelines.
Discovery Health Comprehensive Cancer Cover
You have access to comprehensive cancer treatment coverage. This includes access to expensive medications, innovative treatments, and extended coverage once certain thresholds are reached.
| 🎗️ Discovery Health Prescribed Minimum Benefits (PMB) | PMB cancer treatment is always covered. PMB treatment costs total the cover. Discovery Health will fully cover PMB cancer treatment if it exceeds the cover amount. |
| 💛 Discovery Health Oncology Benefit | After Discovery Health approves your cancer treatment, the Oncology Care Program covers you. Discovery Health will cover approved cancer treatment for 12 months. The first R250,000 is covered. Discovery Health will cover up to 80% of your treatment costs if they exceed the coverage amount. Discovery Health Rate covers 100% of cancer-related healthcare services (DHR). If your doctor charges more, you may have a co-payment. |
| 🟨 Discovery Health Oncology Innovation Benefit | Subject to the Scheme’s clinical entry criteria, the Oncology Innovation Benefit covers a subset of innovative cancer medicine. The member must cover 50% of these treatments. |
| 🟡 Discovery Health – Covering Medicine | To avoid a 20% co-payment, get your approved oncology medicine from a DSP on the Scheme’s medicine list. Ask your doctor if they use the Scheme’s DSPs for your in-room or facility treatment. |
| 💴 Discovery Health Advanced Illness Benefit | Members receive comprehensive palliative care. This program covers unlimited home care, care coordination, counseling, and supportive care for appropriate end-of-life clinical and psychologist services. Your palliative care treatment plan includes GP consultations. |

Discovery Health Hospital Benefit
The Classic Priority includes hospitalization cover. Furthermore, there is no limit on the total amount covered by the Hospital Benefit.
- This benefit covers the costs associated with hospitalization.
- The cover is unlimited in any private hospital approved by the Scheme.
- You are covered for planned hospital stays.
- You may visit any private hospital approved by the Scheme for funding.
- On all health plans, funding newly licensed facilities are contingent upon Scheme approval.
- Certain in-hospital procedures, including those performed by the Day Surgery Network, require an upfront payment.
- Your Hospital Benefit is used to cover planned hospital stays.
- Discovery Health will pay for hospitalization-related services, including all healthcare professionals, services, and medications authorized by the Scheme.
- If you utilize physicians, specialists, and other healthcare professionals with whom Discovery Health agrees, the scheme will pay in full for their services.
- The scheme will pay up to 200% of the Discovery Health Rate (DHR) for other healthcare professionals.
✅ Pre-operative Management Program for major surgeries
- For arthroplasty, colorectal surgery, coronary artery bypass graft, radical prostatectomy, and mastectomy, you are covered for a pre-operative nurse assessment, a consultation (face-to-face, virtual, or telephonic) with your treating healthcare professional, and specific laboratory, pathology, and radiology tests.
- Clinical entry and treatment guidelines govern cover.
✅ The following table summarizes how Discovery Health pays for approved hospital admissions within the Classic Priority.
Healthcare Providers and Services
- The Hospital Account: The full hospital-agreed account according to a rate agreed with the hospital
- Specialist with whom Discovery Health has an arrangement: The entire account, according to the agreed rate
- Specialists with whom Discovery Health does not have an arrangement: Paid up to 200% of the DHR.
- Radiology and Pathology: Up to 100% of the DHR.
Upfront Payments for in-hospital procedures
- Upfront Payment for a defined list of procedures that are performed outside the Day Surgery Network: The member must pay R6,300 upfront
- A defined list of procedures that are performed in a specialist’s room: Covered according to the Scheme-approved rate.
✅ Upfront Amounts payable by the member when a procedure below is performed within the Day Surgery Network
- Conservative Back and neck Treatments, adenoidectomy, myringotomy (grommets), and tonsillectomy: The member must pay R4,300 upfront.
- Arthroscopy, functional nasal procedures, hysterectomy (except for pre-operatively diagnosed cancer), laparoscopy, hysteroscopy, and endometrial ablation: The member must pay R10,000 upfront.
- Nissen fundoplication (reflux surgery), spinal surgery (back and neck), joint replacements: The member must pay R20,600 upfront.
If the procedure can be performed outside the hospital, such as in the doctor’s office, you will not be required to pay the hospital in advance. If any of these procedures are on the list of day surgery procedures, you must pay the greater of the two upfront amounts if the procedure is performed outside the Day Surgery Network.
✅ MRI and CT scans
- Discovery Health pays the first R3,470 of the scan from the day-to-day benefits.
- The Hospital Benefit covers up to 100% of the Discovery Health Rate (DHR) scan balance.
- The member must pay the first R4,300 of the hospital account for conservative back and neck treatment.
- The Hospital Benefit covers the scan balance up to 100% of the DHR.
- This benefit is limited to one scan per spinal and neck region.
Scopes
You are responsible for the following amount depending on where your scope is performed. Your Hospital Benefit will cover the remaining hospital and related charges.
| 🟥 Medical Aid Plan | 🟧 Day Clinic Account | 🟨 Hospital Account |
| 🟩 Classic Priority | R4,050 | This co-payment will be reduced from R6,500 to R5,300 if performed by a doctor in the Scheme’s value-based network. |
| 🟦 If a gastroscopy and colonoscopy are performed during the same admission | – | – |
| 🟪 Classic Priority | R4,950 | This co-payment will be reduced from R8,150 to R6,650 if performed by a doctor in the Scheme’s value-based network. |
Furthermore, the following will apply to scopes on the Classic Priority:
- Scopes performed outside the Day Surgery Network will incur an upfront payment of R6,300 unless performed in a hospital outside the Day Surgery Network.
- The upfront payment will be R6,500.
- Where a gastroscopy and colonoscopy are performed, the upfront payment of R8,150 will apply.
If scopes are performed in the doctor’s office as part of a confirmed Prescribed Minimum Benefits (PMB) condition or if the patient is under 12 years old, no upfront payment is required. Furthermore, the Hospital Benefit covers the bill.

Discovery Health Annual Limits
| 🦻 Cochlear Implants, Auditory Brain Implants, and processors | R230,400 per person per benefit |
| 🧬 Internal Nerve Stimulators | R175,200 per person |
| 🩺 Major Joint Surgery | No limit for planned hip and knee joint replacements if you use a provider in the network, or up to 80% of the Discovery Health Rate (DHR) if you use a provider outside the network, up to R30,900 per prosthesis per admission. Emergency and trauma surgeries are excluded from the network. |
| 🦾 Shoulder Joint Surgery | If you use a provider outside the network, you can pay up to R45,550 for your prosthesis. |
| 🍹 Alcohol and Drug Rehabilitation | Discovery Health will cover 21 days of rehabilitation per person per year. Three days for detoxification per approved admission. |
| 🧠 Mental health | Twenty-one days for admissions or 15 out-of-hospital consultations per person for major affective disorders, anorexia, and bulimia, and 12 for acute stress disorder with recent significant trauma. Three days for attempted suicide admissions. Other mental health admissions are 21 days. Network facilities cover all mental health admissions. If you go elsewhere, the Scheme will pay up to 80% of the Discovery Health Rate (DHR) for the hospital account. |
| ⚕️ Prosthetic Devices used during Spinal Surgery | The preferred prosthesis suppliers have no limit. If you do not use a preferred supplier, the first level is R26,250, and two or more levels are R52,500, limited to one procedure per person per year. The spinal surgery network covers approved spinal surgery admissions. The hospital account will receive up to 80% of the Discovery Health Rate (DHR) for planned admissions outside the Scheme’s network. |
| 🦷 Dental Treatment in the hospital | Dental Limit: Dental treatment is unlimited. However, all dental appliances, prostheses, placement, and orthodontic treatment (including related accounts for orthognathic surgery) are paid at 100% of the Discovery Health Rate (DHR) and up to 200% for anesthetists on the Classic plan. Your daily benefits cover these claims up to R20,300 per person. If you join the Scheme after January, you will not get the full limit because it’s calculated by counting the remaining months in the year. Severe Dental and Oral Surgery In-Hospital: The Severe Dental and Oral Surgery Benefit covers procedures without upfront payment or limit. This benefit requires authorization and Scheme Rules. Basic Dental Trauma: The Basic Dental Trauma Benefit covers unexpected dental injuries requiring emergency treatment after an accident. Dental appliances, prostheses, and placement are covered up to R61,500 per person per year if clinical entry criteria are met. Dental Treatment In-Hospital: Dental admissions require prepaying your hospital or day clinic bill, except for severe dental and oral surgery. Age and treatment location determine this amount. Your Hospital Benefit pays the hospital bill up to 100% of the Discovery Health Rate (DHR). In addition, your Hospital Benefit covers related bills, including the dentist’s, up to 100% of the Discovery Health Rate (DHR). Anesthetists receive 200% of the Discovery Health Rate (DHR). Members 13 and older must pay for routine conservative dentistry like preventive care, fillings, and root canals. Upfront Payments for Dental Admission: Hospital Account – R7,800 for members 13> and R3,000 for members <13 Day Clinic Account – R5,000 for members 12> and R1,350 for members <13 |
Discovery Health Priority Cover for Day Surgery Network Procedures
Discovery Health will provide cover for certain day surgery procedures. A day surgery may take place in a hospital, a day clinic, or an independent facility. Furthermore, these services are covered by your Hospital Benefit. Discovery Health will pay for hospitalization-related services, including all authorized healthcare professionals, services, and medications. If you utilize physicians, specialists, and other healthcare professionals with whom Discovery Health will have a payment arrangement, Discovery Health will cover up to 200% of these services. Furthermore, if you go to a facility not part of the Day Surgery Network, you must pay R6,300 upfront.
If any of these procedures are on the list of hospital admission procedures with an upfront payment, the higher of the two upfront payments will apply. The following list provides the procedures that can be performed in a Discovery Health Day Surgery Network:
- ✅ Biopsies
- ✅ Breast Procedures
- ✅ Ear, nose, and throat procedures
- ✅ Eye Procedures
- ✅ Ganglionectomy
- ✅ Gastrointestinal scopes and procedures
- ✅ Gynecological Procedures
- ✅ Orthopedic Procedures
and many more.

Discovery Health Priority Additional Benefits
✅ Claims Relating to Traumatic Events
- Trauma Recovery Extender Benefit covers out-of-hospital trauma claims.
- The Trauma Recovery Extender Benefit pays claims for the rest of the year and the year after.
- For the year the trauma occurred and the year after, you and your dependents on your health plan can receive six counseling sessions per person per year from a psychologist, clinical social worker, or registered counselor.
- To qualify, members must apply for this benefit.
✅ Africa Evacuation Cover
- Emergency medical evacuations from sub-Saharan African countries to South Africa are covered.
- Excludes pre-existing conditions.
✅ International Travel Benefit
- While traveling outside South Africa, you are covered for emergency medical costs up to R5 million per person.
- The cover lasts 90 days after leaving South Africa.
- This benefit excludes pre-existing conditions.
- Suppose the elective treatment is freely available in South Africa and covered by your plan. In that case, Discovery Health might cover it at equivalent local costs.
✅ International Second Opinion Services
- The Clinic by Cleveland Clinic provides second opinions for life-threatening and life-changing conditions through your specialist.
- Discovery Health will pay 75% for second opinions.
✅ Spinal Care Program
- Conservative spinal treatment out-of-hospital includes virtual and face-to-face consultations with an appropriately registered allied healthcare professional.
✅ In-Room Procedures
- The cover is limited to specialist room procedures.
- Hospital Benefit covers up to the Scheme-authorized rate.
✅ Advanced Illness Benefit
- Members receive comprehensive palliative care.
- This program covers unlimited home care, care coordination, counseling, and supportive care for appropriate end-of-life clinical and psychologist services.
Your palliative care treatment plan includes GP consultations.

Discovery Classic Priority Value-Added Offers
- ✅ Healthy Care at Clicks or Dis-Chem offers discounts on personal and family products. Healthy Care includes baby care, dental care, eye care, foot care, sun care, hand care, first aid, and over-the-counter medicine.
- ✅ Your plan’s optometrists offer 20% off frames and lenses when you pay immediately.
- ✅ Expectant parents can cryogenically store their newborn baby’s umbilical cord blood and tissue stem cells at a discounted rate with Netcells’ exclusive offer.
- ✅ Vitality, the world’s leading science-based wellness program, rewards healthy living. As a result, Discovery Vitality members live longer and healthier lives.
Discovery Health collaborates with myHealthTeam, a global leader in online patient communities. This gives members with diabetes, heart disease, and long-term COVID access to a digital community of patients to manage their conditions.

Discovery Health Classic Priority Exclusions and Waiting Periods
✅ Exclusions include the following:
- Reconstructive surgical procedures and treatments, including cosmetic procedures and treatments.
- Otoplasty for bat ears, blepharoplasty, and port-wine stains (eyelid surgery).
- Breast reductions or augmentations and gynecomastia are considered cosmetic procedures.
- Obesity
- Unless included in Prescribed Minimum Benefits (PMBs) or Assisted Reproductive Therapy, infertility is not covered (ART) Benefit.
- Frail care
- Abuse of alcohol, drugs, or solvents.
- Willful and significant infraction of the law.
- Willful participation in a war, a terrorist act, a riot, a civil disturbance, a revolt, or an uprising.
- Injuries incurred or medical care rendered during travel to or within a country at war.
- Experimental, unproven, or unregistered treatments or practices.
- Rescue and search.
✅ Discovery Health’s waiting periods are as follows:
- During your waiting periods, you will not have access to the Prescribed Minimum Benefits (PMBs) if you are subject to waiting periods due to never having belonged to a medical scheme or a break in membership of more than 90 days before joining Discovery Health Medical Scheme, including emergency admission cover.
If you had less than a 90-day break in cover before enrolling in Discovery Health Medical Scheme, you might be eligible for Prescribed Minimum Benefits (PMBs) during waiting periods.

Discovery Health Classic Priority Plan vs Similar Plans from Other Medical Schemes
| 🔎 Medical Aid Plan | 🥇 Classic Priority | 🥈 Bestmed Pace 1 | Medihelp MedPrime |
| 👤 Main Member Contribution | R5,272 | R4,620 | R4,200 |
| 👥 Adult Dependent Contribution | R4,158 | R3,245 | R3,552 |
| 🍼 Child Dependent Contribution | R2,108 | R1,166 | R1,230 |
| 🔁 Gap Cover | ✅ Yes | None | None |
| 💙 Medical Savings Account | ✅ Yes | ✅ Yes | ✅ Yes |
| 👶 Maternity Benefits | ✅ Yes | ✅ Yes | ✅ Yes |
| ➡️ Pre- and Postnatal Care | ✅ Yes | ✅ Yes | ✅ Yes |
| ↪️ Extended Cover for Oncology | None | Out-of-Hospital cover | None |
| 💶 Hospital Cover | Unlimited | Unlimited | Unlimited |

Our Verdict on Discovery Health Classic Priority
The Classic Priority is a medical aid plan offered by the Discovery Health Medical Scheme. It covers medical expenses such as hospitalization, specialist consultations, and chronic medication. One of the key features of this plan is that it allows members to choose their healthcare providers and specialists, which gives them greater flexibility and control over their healthcare. Another noteworthy feature of the Classic Priority plan is that it provides unlimited hospital cover, which means that members can stay in the hospital for as long as they need to without worrying about running out of cover.
This is particularly important for those requiring extended hospital stays for serious medical conditions or surgeries. In addition, the plan includes a range of preventative healthcare benefits, such as annual health assessments and screenings, which can help members identify potential health risks and take steps to address them before they become more serious. However, one potential drawback of the Classic Priority plan is that it is relatively expensive compared to other medical aid plans offered by the Discovery Health Medical Scheme.
This may make it less accessible to individuals or families on a tighter budget and cannot afford higher premiums. Another potential drawback is that some of the benefits offered by the plan, such as certain chronic medication benefits, may be subject to specific limits and restrictions. This means that members may be unable to access certain medications or treatments if they exceed these limits.
You might also like: ➡️ Discovery Health Priority Series
You might also like: ➡️ Discovery Health Essential Priority
Discovery Health Classic Priority Frequently Asked Questions
Are pre-existing conditions covered on the Classic Priority plan?
Yes, pre-existing conditions are covered on the Classic Priority plan. However, they may be subject to waiting periods before the full cover is provided.
Can I choose my healthcare providers on the Classic Priority plan?
Yes, one of the key features of the Classic Priority plan is that it allows members to choose their own healthcare providers and specialists.
Does the Classic Priority plan cover emergency medical expenses?
Yes, the Classic Priority plan covers emergency medical expenses, including ambulance services and emergency room visits.
Can I add dependents to my Classic Priority plan?
Yes, you can add dependents such as spouses and children to your Classic Priority plan, subject to certain eligibility criteria. A child dependant start at R2,108
How do I know if the Classic Priority plan covers a specific medication or treatment?
You can check the Classic Priority plan guide or contact the Discovery Health Medical Scheme call center to confirm whether a specific medication or treatment is covered under the plan.
You might also like
Table of Contents
Free Medical Aid Quote
Our Trusted Partners
We work with leading medical aid companies in South Africa.

7 Actionable Ways to save 32% on your MEDICAL AID in 14 days.

- +27 72 7967 530
- [email protected]
- 2nd Floor, West Tower, Nelson Mandela Square, Sandton, 2196, Johannesburg, Gauteng, South Africa
🔎 Report a bug or outdated data to be updated to [email protected]
© Medicalaid.com | All rights Reserved |
Copyright 2024
Top 5 Medical Aids
Top 5 Gap Cover Plans
































