- Medical Aid
- Currently Trending
The Best Medical Aids
- Compare Plans
- Gap Cover
- Best Gap Covers
- Hospital Plans
- Currently Trending
The Best Hospital Plans
- Medical Insurance
- Pet Insurance
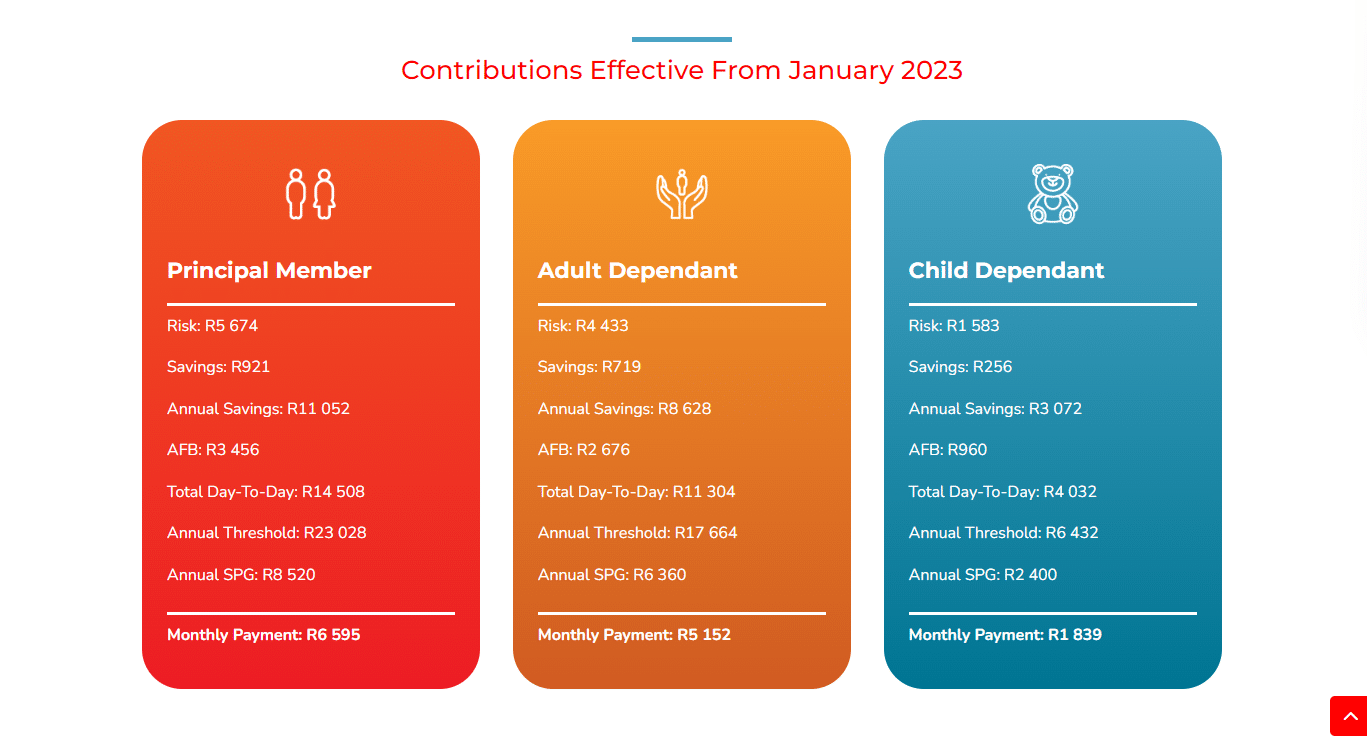
CompCare DYNAMIX Medical Aid Plan
Overall, the CompCare DYNAMIX Medical Aid Plan is a trustworthy and comprehensive medical aid plan that offers 24/7 medical emergency assistance and unlimited hospital cover to up to 3 Family Members. The CompCare DYNAMIX Medical Aid Plan starts from R7,578 ZAR.
| 👤 Main Member Contribution | R7,578 |
| 👥 Adult Dependent Contribution | R5,920 |
| 💙 Child Dependent Contribution | R2,113 |
| 📉 Annual Limit | Unlimited |
| ➡️ Hospital Cover | Unlimited |
| 🍼 Maternity Benefits | ☑️ Yes |
| ↪️ Gap Cover | None |

CompCare DYNAMIX Plan – 7 Key Point Quick Overview
- ☑️ CompCare DYNAMIX Plan Overview
- ☑️ CompCare DYNAMIX Plan Contributions and Benefits
- ☑️ DYNAMIX Plan Benefits and Cover Comprehensive Breakdown
- ☑️ DYNAMIX Plan Exclusions and Waiting Periods
- ☑️ CompCare DYNAMIX Plan vs. Similar Plans from Other Medical Schemes
- ☑️ Our Verdict on The DYNAMIX Plan
- ☑️ DYNAMIX Plan Frequently Asked Questions
CompCare DYNAMIX Plan Overview
The CompCare DYNAMIX medical aid plan is one of 9, starting from R7,578. With the DYNAMIX option, you can enjoy comprehensive coverage that includes unlimited hospital coverage. In addition, you can also benefit from a savings account, flexible risk cover, and above-threshold benefits.
Gap Cover is not available on the CompCare DYNAMIX Plan. CompCare offers 24/7 medical emergency assistance.
According to the Trust Index, CompCare has a trust rating of 3.4.

CompCare DYNAMIX Plan Contributions and Benefits
CompCare DYNAMIX Contributions
| 👤 Main Member | 👥 Adult Dependent | 🍼 Child Dependent |
| R7,578 | R5,920 | R2,113 |
CompCare DYNAMIX Annual Savings
| 👤 Main Member | 👥 Adult Dependent | 🍼 Child Dependent |
| R12,720 | R9,936 | R3,540 |
READ MORE: 5 Best Medical Aids under R200
CompCare DYNAMIX Annual Flexi Benefit (AFB)
| 👤 Main Member | 👥 Adult Dependent | 🍼 Child Dependent |
| R3,624 | R2,808 | R1,008 |
Discover the Best Medical Aids in South Africa Covering Braces
CompCare DYNAMIX Total Day-to-Day Benefit
| 👤 Main Member | 👥 Adult Dependent | 🍼 Child Dependent |
| R16,344 | R12,744 | R4,548 |
CompCare DYNAMIX Threshold Amount
| 👤 Main Member | 👥 Adult Dependent | 🍼 Child Dependent |
| R26,569 | R20,379 | R7,428 |
You might also like the 5 Best Hospital Plans under R1500 in South Africa
CompCare DYNAMIX Annual Self-Payment Gap (SPG)
| 👤 Main Member | 👥 Adult Dependent | 🍼 Child Dependent |
| R10,225 | R7,635 | R2,880 |

DYNAMIX Plan Benefits and Cover Comprehensive Breakdown
In-Hospital Benefits
| 🏥 Hospitalization Private Hospitals Nursing Homes | Covered up to 100% of the scheme rate. Subject to pre-approval, case management, and scheme protocols. |
| 🅰️ Efficiency Discounted (ED) Members can choose Designated Service Providers (DSPs) for in-hospital services and chronic medicines to receive discounts. Voluntary admission to a non-Netcare facility requires a 30% co-payment of R7 500 – Not applicable to emergencies. Non-DSP pharmacies require a 25% co-payment. | Netcare hospitals can be used. Medicine can be obtained from Dis-Chem pharmacies. |
| 🅱️ Overall Annual Limit | Unlimited |
| 👩⚕️ GPs and Specialists | Covered up to 100% of the scheme rate. Unlimited cover provided. |
| 💊 Medication in-hospital | Covered up to 100% of the cost. |
| ☑️ Medication upon discharge from the hospital | Subject to Reference Pricing (RP) and Formularies. Limited to 7 days’ supply. |
| 🦾 Surgical Prostheses | Subject to pre-authorization. Limited to an overall limit of R47,000. Sub-limits will apply according to categories. |
| ✅ Auxiliary Services | Limited to R8,800 per family. The combined limit for in and out-of-hospital treatment. Subject to pre-approval and protocols. A medical practitioner must recommend treatment. |
| 🧠 Psychiatric In-hospital Treatment | Covered up to 100% of the scheme rate. Subject to pre-authorization, protocols, and PMBs. |
| ➡️ Psychology (non-psychiatric admissions) | Limited to R4,290 per family. |
| ↪️ All specialized radiology MRI scans CT scans PET scans | Covered up to 100% of the scheme rate. Unlimited – Authorization is required. PET scans require special motivation and approval. Unauthorized scans are not covered. Screening scans are not covered. The PMSA covers the first R2,500. Claims accumulate to the threshold unless there is a PMB. |
| 🔁 Basic Radiology | Covered up to 100% of the scheme rate. Unlimited cover but subject to scheme protocols. |
| 📈 Pathology | Covered up to 100% of the scheme rate. Subject to pre-approval and protocols. The cover is unlimited. |
| 📉 Confinements for Maternity | Covered up to 100% of the scheme tariff. Subject to pre-authorization and clinical protocols. |
| 📊 Rehabilitation in-hospital Alcoholism Drug Dependence Narcotics | Subject to pre-authorization, protocols, and PMBs. |
| 💖 Organ Transplants, Plasmapheresis, Renal Dialysis | Subject to pre-authorization, protocols, and PMBs. |
| 🏈 Professional Sports Injuries | Subject to pre-approval. Scheme protocols will apply. |
Hospitalisation Alternatives
| 🎗️ Oncology Chemotherapy Radiotherapy | Unlimited cover when using an Oncology DSP. Subject to pre-approval and protocols. The Oncology formulary will apply. |
| 🧪 Biological agents and Specialised Medication | Limited to R250,000 per family per year. Pre-approval is required. Protocols will apply. Non-PMB medicines attract a 25% co-payment. |
| ⬇️ Step-down facilities, hospice, rehabilitation | Unlimited coverage is offered. Subject to pre-authorization and clinical guidelines. |
| 🩺 Surgical Procedures performed out-of-hospital | Unlimited cover. Subject to pre-approval and protocols. |
| 🧬 Radial Keratotomy and Excimer Laser | Limited to R8,000 per eye. Subject to the optical benefit. Pre-authorization is required, and protocols will apply. |
| 🩹 Wound care instead of hospitalization | Unlimited cover provided. Subject to pre-approval and protocols. |
Day-to-Day Benefits
| 🟥 Day-to-day Benefits and Limits | Paid from the PMSA and then the AFB. After depleting these, the member enters the Self-Payment Gap, where they must pay for all out-of-pocket claims. Claims will accumulate to the threshold at the scheme rate. Once the threshold is reached, Above Threshold Benefits (ATB) will be available up to R9,200 per beneficiary and R16,380 per family. Sub-limits might apply. |
| 🟧 General Practitioner (GPs) Consultations | Covered up to 100% of the scheme rate and includes consultation fees, procedures, and material costs. The benefit is paid from the PMSA, AFB, and SPG. Unlimited after the threshold is reached. Children <6 years have unlimited GP visits. |
| 🟨 Specialist Consultations | Covered up to 100% of the scheme rate. The benefit is paid from the PMSA, AFB, and SPG. Unlimited after the threshold is reached. Members must be referred by a GP or face a 30% co-payment. |
| 🟩 Chronic Medicine | Subject to the formulary. Reference Pricing will apply. Unlimited coverage for 65 conditions (27 CDL and 38 non-CDL conditions). The benefit is paid from the PMSA, AFB, and SPG. Unlimited after the threshold is reached. Limited to R10,000 per beneficiary and R17,850 per family. The ATB is limited to R3,500 and subject to the Above Threshold Limit. |
| 🟦 Acute Medicine (Schedule 3>) | The benefit is paid from the PMSA, AFB, and SPG. Unlimited after the threshold is reached. The ATB is limited to R3,350 per family and is subject to the annual threshold. There is a 25% co-payment for non-generic products. Subject to the MMAP. |
| 🟪 Over the Counter (OTC) Medicine | The benefit is paid from the PMSA, AFB, and SPG. Unlimited after the threshold is reached. Limited to R1,050 per beneficiary and R1,500 per family, with an R240 maximum per event. Specified Sports supplements are available if there is a valid NAPPI code. |
| 🟥 Basic Radiology Black and White X-Rays Ultrasounds | Covered up to 100% of the scheme rate. The benefit is paid from the PMSA, AFB, and SPG. Unlimited after the threshold is reached. An ATB of R4,000 per family is subject to the overall annual limit. |
| 🟧 Specialized Radiation MRI scans CT scans PET scans | Combined in out-of-hospital specialized radiology benefits. The first R2,500 is paid from the PMSA, AFB, and SPG and will accumulate to the threshold. |
| 🟨 Pathology | Covered up to 100% of the scheme rate. The benefit is paid from the PMSA, AFB, and SPG. Unlimited after the threshold is reached. An ATB of R4,000 per family is subject to the overall annual limit. |
| 🟩 Conservative Dentistry Consultations Preventative Care Fillings Extractions Infection Control | Paid up to 100% of the scheme rate. The benefit is paid from the PMSA, AFB, and SPG. Unlimited cover for children <6 years. |
| 🟦 Specialized Dentistry Maxillo-facial and oral surgery In and Out-of-hospital combined limit | Covered up to 100% of the scheme rate. Subject to a sub-limit of R14,850 per beneficiary and R20,000 per family. Subject to scheme protocols. The benefit is paid from the PMSA, AFB, and SPG. |
| 🟪 Optometry | Paid from the PMSA and AFB. Limited to two visits per beneficiary every second year. |
| 🟥 Lenses and Contact Lenses | Paid up to 100% of the scheme rate. Paid from the AFB. Subject to a sub-limit of R4,600 per beneficiary. Subject to protocols. |
| 🟧 Frames | A sub-limit of R2,000 applies per frame. There is a limit of one frame per beneficiary per second year included in the lens limit. |
| 🟨 Allied Services Speech Therapists Social Workers Podiatrists Occupational Therapists Homeopaths and Naturopaths Dieticians Chiropractors, etc. | Covered up to 100% of the scheme rate. The benefit is paid from the PMSA, AFB, and SPG. Collectively limited to R8,800 per family in and out-of-hospital. |
| 🟩 Clinical Psychologists | Covered up to 100% of the scheme rate. The benefit is paid from the PMSA, AFB, and SPG. Subject to a sub-limit of R3,000 per family. |
| 🟦 Surgical and Medical Appliances Wheelchairs Crutches Glucometers Artificial eyes External fixators | Covered up to 100% of the scheme rate. Subject to sub-limits and protocols. Paid from the PMSA and AFB. |
| 🟪 Psychiatry | Covered up to 100% of the scheme rate. Paid from the AFB up to a sub-limit of R12,500 per family. |
| 🟥 Psychosocial Counselling | Paid from risk. Unlimited telephonic counseling sessions through the Universal Wellness Care Centre Member can opt for referral to one-on-one sessions with qualified psychologists, social workers, or registered counselors up to three referral sessions PB per year. |
| 🟧 Oxygen Home Ventilation | Covered up to 100% of the scheme rate. Paid from the PMSA and AFB. |
| 🟨 Home Nurse Visits | Covered up to 100% of the scheme rate. Limited to 40 days per family. Paid from the PMSA and AFB. |
| 🟩 Antenatal Classes | Covered up to 100% of the scheme rate. Paid from the PMSA and AFB. Limited to 12 antenatal classes and one lactation consultation with a midwife. Limited to R1,650 per pregnancy. |
| 🟦 Antenatal Visits and Scans | Covered up to 100% of the scheme rate. Limited to 12 visits with a GP, midwife, or specialist. The benefit is paid from risk. Limited to 2 x 2D fetal scans per beneficiary per year. Members can opt for one 3D scan, which is paid at the rate of a 2D scan. A maternity bag is issued once a pregnant member registers for the maternity program. |
| 🟪 Emergency roadside assistance and ambulance transport (Netcare 911) | Covered up to 100% of the scheme rate. Netcare 911 must authorize non-emergency transportation within 24 hours or risk a 25% co-payment. |
| 🟥 International Travel Benefit Healthcare services outside South Africa | Subject to benefits per individual benefit category. All claims are paid according to South African rates. Members must register their journey and get a travel certificate to qualify for cover. |
| 🟧 Hospital Emergency room and casualty emergency visits (no admission and excluding facility fees) | Paid from the PMSA and AFB. |
| 🟨 Lipogram | Limited to one fasting lipogram per beneficiary 20 years> once every 5 years. |
Discover the 5 Best Limited Day to Day Cover Plans
Wellness, Lifestyle, and Preventative Care Benefits
| 🔴 GP Wellness Consultation | Limited to one visit per beneficiary yearly. |
| 🟠 Blood Pressure, Blood Sugar, Cholesterol, BMI, and Waist Circumference | Limited to one measurement per beneficiary yearly for those 18 years>. |
| 🟡 Rapid HIV Test | One test per beneficiary yearly. |
| 🟢 Flu Vaccine | One vaccine per beneficiary yearly. |
| 🔵 Tetanus Vaccine | One injection as required. |
| 🟣 Prostate Specific Antigen (PSA) | One per male beneficiary 40 years>. |
| 🔴 Bowel Cancer Screening | One screening per beneficiary between 45 and 75 every two years. |
| 🟠 Glaucoma Test | One per beneficiary per year. |
| 🟡 Pap Smear | One per female beneficiary 18 years> once yearly. |
| 🟢 Mammogram | One test per female beneficiary 35 years> every two years. |
| 🔵 HPV Vaccine | One course per female beneficiary between 12 and 18 years. |
| 🟣 Adult Pneumococcal Vaccine | Per beneficiary as required. Subject to pre-approval and protocols. |
| 🔴 Fitness Assessment and Exercise Prescription | Fitness assessment and exercise prescription: Annual fitness assessment, virtual consultations, exercise prescription, and monitoring by Universal Network biokinetics. |
| 🟠 Additional Assessment for pregnant members | Limited to one additional assessment. Strict protocols will apply. |
| 🟡 Nutritional Assessment and Healthy Eating Plan | Fitness assessment and exercise prescription: Annual fitness assessment, virtual consultations, exercise prescription, and monitoring by Universal Network biokinetics. |
| 🟢 Additional Assessment for pregnant members | Limited to one additional assessment. Strict protocols will apply. |
| 🔵 Contraceptives | Limited to R3,360 per beneficiary per year for female beneficiaries up to 55 years. Reference pricing will apply. CompCare only covers UID devices. |
| 🟣 COVID-19 | Those who test positive for COVID-19 have access to several benefits in addition to PMBs. Subject to pre-approval and managed care protocols. |
| 🔴 Pulse Oximeter | Limited to R850 per month. |
| 🟠 Nebulizer | Limited to R550 per month. |
| 🟡 Thermal Thermometer | Limited to R450 per month. |
Newborn to Adult Benefit
| 🍼 Newborn Hearing Screening and Congenital Hypothyroidism Test | Limited to three Paediatric consultations. Access is given to pediatric telephonic advisory services. |
| 👶 Baby Wellness Visit | Two visits yearly for children between 4 weeks and 18 months. Members must use a DSP. |
| 💉 Childhood Immunisations | Available for children up to 12 years old, as per the Department of Health. |
| 🎓 School Readiness Assessment | Psychometric testing for children 5 – 7 years and 14 to 18. Pre-school eye and hearing screening for children between 5 and 6 years old. Dental Screening for children 5 – 7 years old. |
| 🏈 Kids Active Benefit | Universal Network biokinetics assesses and prescribes exercise for 8–12-year-olds. SporTeen: Universal Network bio kineticist-led annual fitness assessment, virtual consultations, and exercise prescription for 13 – 17-year-old children. |
| 🍎 Kids Nutritional Benefit | For 8-year-olds and older, Universal Network dietitians provide nutritional assessments and healthy eating plans. |
You might like Health Insurance for Kids
Chronic Conditions Covered
The following chronic conditions are covered under the DYNAMIX plan:
- ☑️ Addison’s disease
- ☑️ Allergic rhinitis
- ☑️ Angina
- ☑️ Ankylosing spondylitis
- ☑️ Asthma
- ☑️ Attention deficit disorder
- ☑️ Bechet’s disease
- ☑️ Bipolar mood disorder
- ☑️ Bronchiectasis
and many more.

DYNAMIX Plan Exclusions and Waiting Periods
DYNAMIX Exclusions
The following are some of the exclusions on the CompCare DYNAMIX Plan:
- ✅ The scheme will not pay for expenses that exceed the annual maximum benefit.
- ✅ A general waiting period of 3 months may be applied to new members and their dependents according to the scheme rules.
- ✅ According to the scheme rules, a condition-specific waiting period of up to 12 months may be applied for pre-existing sickness conditions.
- ✅ The scheme will not cover any costs incurred during waiting periods.
- ✅ Certain professional fees and expenses incurred by healthcare professionals will not be covered, such as after-hours consultations at the member’s choice, unattended appointments, interest charges by healthcare providers, costs incurred for insurance medical purposes, fees for medical reports, and motivations unless required by the scheme, and discretionary conditions and services with unauthorized hospital admissions.
- ✅ Costs for services rendered by unregistered professionals or institutions, except state or provincial hospitals registered under South African law, will not be covered.
Frail care services will not be covered, including accommodation and nursing care in convalescent or nursing homes catering to the aged or chronically ill.
Read more about the 5 Best Medical Aid with Immediate Cover (No Waiting Period)
DYNAMIX Waiting Periods
Prospective members must disclose all details of any past medical condition or treatment. Furthermore, waiting periods are applied when joining the scheme or registering new dependents. In terms of the CompCare DYNAMIX plan, the following applies:
- ✅ A general waiting period of 3 months and a 12-month condition-specific waiting period may be imposed for pre-existing medical conditions if not covered on a medical scheme for more than 90 days.
- ✅ A condition-specific waiting period of 12 months may be imposed if applying for membership within 3 months of termination from a previous scheme and having been on a medical scheme for less than 24 months.
- ✅ If applying for membership within 3 months of termination from a previous scheme and having been on a medical scheme for more than 24 months, a general waiting period of 3 months will apply.
- ✅ Prescribed Minimum Benefits are available during waiting periods.
- ✅ The scheme may impose any unexpired balances by the previous scheme if the beneficiary suffers from any pre-existing condition.
- ✅ New members and their dependents have a 3-month general waiting period.
- ✅ Prescribed Minimum Benefits are available during the general waiting period.
- ✅ The waiting period does not apply to emergency medical treatment.
- ✅ Any costs incurred during waiting periods will not be covered.
- ✅ Members are responsible for submitting all claims within the required time frame.
Aside from a waiting period, a late joiner fee will apply.
Medical Aid Comparison : CompCare DYNAMIX Plan vs. Similar Plans from Other Medical Schemes
| 🔎 Medical Aid | 🥇 CompCare DYNAMIX | 🥈 Cape Medical Plan MyHealth 200 Plus | 🥉 Discovery Health Classic Smart Comprehensive |
| 🌎 International Cover | Subject to benefits per individual benefit category. | ❎ None | R5 million |
| 👤 Main Member Contribution | R7,578 | R9,140 | R7,163 |
| 👥 Adult Dependent Contribution | R5,920 | R9,140 | R6,611 |
| 🍼 Child Dependent Contribution | R2,113 | R1,476 | R1,671 |

Our Verdict on The DYNAMIX Plan
The DYNAMIX plan from CompCare offers members several unique features and benefits. One of the most notable advantages of the plan is its comprehensive cover for hospitalization, which includes in-hospital specialist consultations, procedures, and medication.
Members can receive top-quality medical care and treatment without worrying about unexpected costs. The plan also offers a range of benefits for chronic conditions such as cancer, diabetes, and hypertension.
Overall, the DYNAMIX plan offers members several unique features and advantages, such as its comprehensive hospitalization coverage and flexible day-to-day benefit options.
You might also consider the following plans from CompCare:
- 🏆 CompCare MEDX Plan
- 🏆 CompCare MUMED Plan
- 🏆 CompCare NETWORX Plan
- 🏆 CompCare PINNACLE Plan
- 🏆 CompCare SELFNET Plan
- 🏆 CompCare SELFSURE Plan
- 🏆 CompCare SYMMETRY Plan
- 🏆 CompCare UNISAVE Plan
DYNAMIX Plan Frequently Asked Questions
What is the DYNAMIX plan from CompCare?
The DYNAMIX plan from CompCare is a healthcare plan that offers comprehensive hospitalization coverage, chronic condition benefits, flexible day-to-day cover, and an extensive network of healthcare providers.
What is covered under the DYNAMIX plan’s hospitalization cover?
The DYNAMIX plan’s hospitalization cover includes in-hospital specialist consultations, procedures, and medication.
Does the DYNAMIX plan offer benefits for chronic conditions?
Yes, the DYNAMIX plan offers a range of benefits for chronic conditions such as cancer, diabetes, and hypertension.
Can I customize my benefits under the DYNAMIX plan?
Yes, members can choose from various benefit options, such as primary healthcare, chronic medication, and wellness benefits, to customize their coverage according to their specific needs and budget.
What is the DYNAMIX plan’s network of healthcare providers like?
The DYNAMIX plan has an extensive network of healthcare providers, including general practitioners, specialists, and pharmacies, ensuring that members have access to quality care and treatment wherever they are.
Are there waiting periods for certain benefits under the DYNAMIX plan?
Yes, there may be waiting periods for certain benefits under the DYNAMIX plan.
Are there any limitations on the number of consultations or procedures covered under the DYNAMIX plan?
Yes, there may be limitations on the number of consultations or procedures covered under the DYNAMIX plan.
Is the DYNAMIX plan affordable?
No, DYNAMIX is one of the more expensive plans that CompCare offers, starting from R7,578 per month for the main member, which is on par with most competitors’ premium plans.
Does the DYNAMIX plan offer health savings accounts?
Yes, an annual saving (PMSA) is available on DYNAMIX in addition to day-to-day benefits, above the threshold, and more.
Will I have any out-of-pocket expenses under the DYNAMIX plan?
Depending on the level of coverage and benefits selected, members may have some out-of-pocket expenses under the DYNAMIX plan.
Does the DYNAMIX plan offer any health and wellness programs?
Yes, DYNAMIX offers health and wellness programs, preventative benefits, and more.
How do I enroll in the DYNAMIX plan?
Members can enroll in the DYNAMIX plan by contacting CompCare directly or through a registered broker.
[xyz-ips snippet="KK-Star"]
You might also like
Table of Contents
Free Medical Aid Quote
Our Trusted Partners
We work with leading medical aid companies in South Africa.

7 Actionable Ways to save 32% on your MEDICAL AID in 14 days.

- +27 72 7967 530
- [email protected]
- 2nd Floor, West Tower, Nelson Mandela Square, Sandton, 2196, Johannesburg, Gauteng, South Africa
🔎 Report a bug or outdated data to be updated to [email protected]
© Medicalaid.com | All rights Reserved |
Copyright 2024
Top 5 Medical Aids
Top 5 Gap Cover Plans
Your compare list
Back
REMOVE ALL
0
































