- Medical Aid
- Currently Trending
The Best Medical Aids
- Compare Plans
- Gap Cover
- Best Gap Covers
- Hospital Plans
- Currently Trending
The Best Hospital Plans
- Medical Insurance
- Pet Insurance
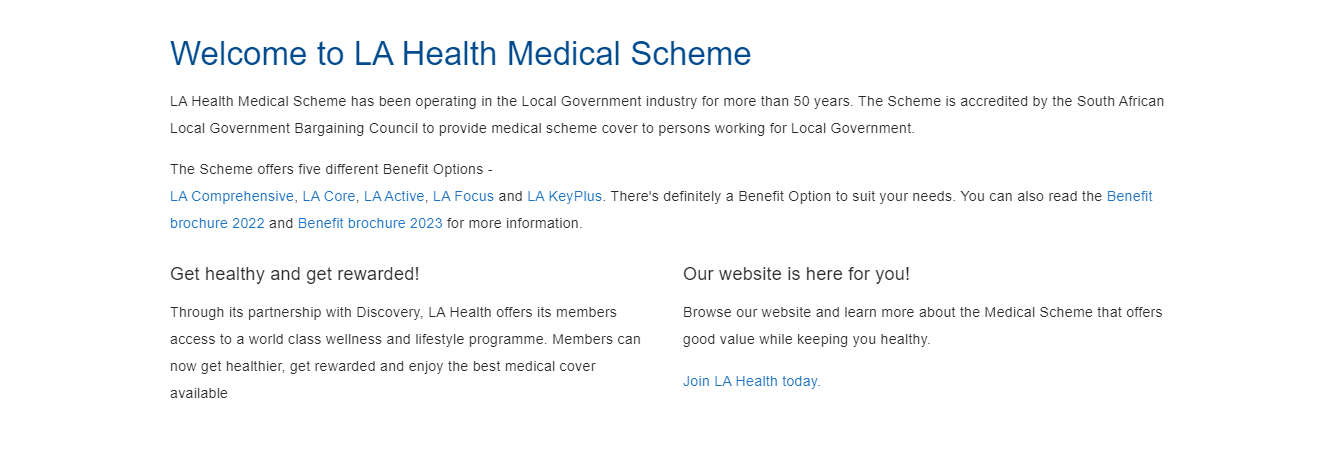
LA Health Medical Scheme
Overall, LA Health offers 5 medical aid plans (LA Comprehensive, LA Core, LA Active, LA Focus, and LA KeyPlus) starting from R1,390 per month. Additionally, LA Health offers 24/7 emergency support but does not offer comprehensive gap cover on any policy.
| 🔎 Medical Aid | 🥇 LA Health |
| 📈 Number of Employees | <50 |
| 📉 GCR Rating | n/a |
| 📊 Listed on the JSE | ❎ No |
| 📌 JSE Stock Symbol | None |
| 📍 The most recent Market Cap reported | None |
| 💯 Average Customer Rating | 3.5 |
| ❤️ Average Number of Reviews | 60+ |
| ✔️ Market Share | <1% |
| 5️⃣ Number of plans offered | 5 |

LA Health Review – Analysis of Medical Aids’ Main Features
- ✅ LA Health Regulation
- ✅ LA Health at a Glance
- ✅ LA Health Plan Overview
- ✅ LA Health – Advantages over Competitors
- ✅ LA Health Medical Savings Account
- ✅ How to apply for Medical Aid with LA Health
- ✅ How to Submit a Claim with LA Health
- ✅ How to Submit a Compliment or Complaint with LA Health
- ✅ How to Switch my Medical Aid to LA Health
- ✅ LA Health Customer Support
- ✅ LA Health vs Discovery Health vs Platinum Health – A Comparison
- ✅ LA Health Member Reviews
- ✅ LA Health – Our Verdict
- ✅ LA Health Pros and Cons
- ✅ LA Health Frequently Asked Questions
LA Health Regulation
The Council for Medical Schemes regulates LA Health Medical Scheme. The Council governs South Africa’s medical plan business for Medical Schemes (CMS), a regulating body set up under the Medical Schemes Act, No. 131 of 1998 (the Act). The CMS is responsible for a range of tasks related to the oversight of medical insurance plans, such as:
- Responsible for registering medical insurance plans and ensuring they comply with the law and other laws.
- Making sure healthcare plans have the money to pay claims.
- Examining and authorizing proposed price hikes for medical plans.
- Accepting and examining member complaints and initiating disciplinary action against medical plans that violate the Act or other applicable rules.
- Helping medical insurance plans follow the law and other laws.
Furthermore, if a medical scheme is found to violate the law, the CMS has the authority to issue administrative fines and penalties.
LA Health at a Glance
| 🔎 Medical Aid | 🥇 LA Health |
| 📌 Date Established | 1973 |
| 📍 Headquartered | Gauteng, South Africa |
| 📎 Registration Number | 1145 |
| 👥 The average number of members | Unknown |
| 🌐 Number of Markets | South Africa |
| 👤 Number of Employees | <50 |
| ✒️ GCR Rating | n/a |
| 📈 Listed on the JSE | ❎ No |
| 📉 JSE Stock Symbol | None |
| 📊 The most recent Market Cap reported | None |
| 💯 Average Customer Rating | 3.5 |
| ❤️ Average Number of Reviews | 60+ |
| 📌 Market Share | <1% |
| 5️⃣ Number of plans offered | 5 |
| 🚑 Number of Hospitals in Network | 200+ |
| 🏠 Home care provided | ✅ Yes |
| 💙 Sponsorships | None |
| 📱 Is a Mobile App offered | ✅ Yes |
| ⚠️ Social Media Platforms and Links | ✅ Yes |
| 📖 LA Health Magazine for clients | ❎ No |
| 💻 Medical Claims Portal | ✅ Yes |
| 🖥️ Customer Support Operating Hours | Monday to Friday, 7 am to 5 pm |
| 😷 Information Hub for COVID-19 | ✅ Yes |
| ⚕️ Chronic Illness Benefits | ✅ Yes |
| 📌 Number of PMB Diagnoses | 270 |
| 📍 Number of PMB Chronic Conditions | 26 |
| 🖥️ Screening and Prevention offered | ✅ Yes |
| 👶 Maternity Benefit | ✅ Yes |
| 💵 Medical Aid Contribution Range (ZAR) | 1,390 – 9,379 ZAR |
| ⛔ Average Waiting Period | 12 months |
| 💶 Late-joiner penalties | ✅ Yes |
| 🌎 Is International Medical Cover offered | ✅ Yes |
| 💵 International Travel Benefit (ZAR) | 5 million ZAR |
Medical Aid LA Health Plan Overview
| 🔎 Plan | 💵 Contributions (Main) | 💶 Contributions (+ Adult) | 💴 Contributions Range (+ Child – MAX 3) | 💷 Medical Savings (Up to) | 📌 PMB Diagnosis | 📍 Chronic Conditions |
| 1️⃣ LA KeyPlus | 1,390 – 2,207 ZAR | 1,214 – 1,964 ZAR | 508 – 824 ZAR | None | 270 | 26 |
| 2️⃣ LA Focus | 2,904 ZAR | 1,875 ZAR | 852 ZAR | · 8,712 ZAR (Main) · 5,628 ZAR (Adult) · 2,556 ZAR (Child) | 270 | 26 |
| 3️⃣ LA Active | 3,539 ZAR | 2,380 ZAR | 1,174 ZAR | · 8,172 ZAR (Main) · 5,916 ZAR (Adult) · 3,384 ZAR (Child) | 270 | 26 |
| 4️⃣ LA Core | 6,998 ZAR | 6,317 ZAR | 2,091 ZAR | · 12,156 ZAR (Main) · 10,620 ZAR (Adult) · 4,884 ZAR (Child) | 270 | 26 |
| 5️⃣ LA Comprehensive | 9,379 ZAR | 7,161 ZAR | 2,274 ZAR | · 15,108 ZAR (Main) · 8,760 ZAR (Adult) · 3,828 ZAR (Child) | 270 | 26 |
LA KeyPlus
Overview
The LA KeyPlus Option provides comprehensive cover for hospital care, Prescribed Minimum Benefit Chronic Disease List cover, and day-to-day medical expenses. The Keycare Network of hospitals serves as the designated service provider for all planned Prescribed Minimum Benefits and procedures. Treatment for some care services is only available at one of the approved Day Surgery Network facilities. Members are fully covered for GP and other care services when utilizing providers’ services in the Keycare Primary Care Network.
Prescribed Minimum Benefits
Prescribed Minimum Benefits are paid according to the cost and clinical criteria and using the designated service providers in the Keycare Network. For non-PMB benefits, the cover is up to 100% of the Scheme Rate, subject to clinical criteria, the use of the Scheme’s designated providers, and applicable limits.
Emergency Cover
LA KeyPlus provides cover for emergency medical transport in case of an emergency, and the cost is paid from the Major Medical Benefit, with no overall limit. Authorizations can be obtained by calling Discovery 911.
GPs and Specialists In-Hospital and Out-of-Hospital
For in- and out-of-hospital care, there is no overall limit applied when a member is admitted to a hospital in the Keycare Network. The program pays up to 100% of the Direct Payment Arrangement Rate for Keycare hospital-based specialists who have agreed to these rates. For all other specialists working in a hospital in the Keycare Network, the scheme pays up to 100% of the LA Health Rate. In addition, certain defined procedures must be treated at a Day Surgery Network facility. The policy provides unlimited cover for out-of-hospital GP visits and selected small procedures when utilizing the services of a GP working in the Designated Service Provider Network.
However, authorization is required for GP visits exceeding 15 times in a year, from the 15th visit onward. For unscheduled emergency visits, the policy covers three visits per person per year at the chosen GP. The Out-of-Network Benefit covers four GP visits per person per year and selected blood tests, X-rays, and acute formulary medicine requested by a non-network GP. The policy offers a cover of R5,000 per person for out-of-hospital specialist visits, including radiology and pathology done in the Keycare network, when referred by a chosen Keycare GP.
Hospitalization Cover
The Keycare Network offers comprehensive cover for hospitalization, theatre fees, and costs for intensive and high care at private hospitals and specific procedures at Day Surgery Network facilities. The cover is subject to meeting certain clinical entry criteria and protocols, and treatment must be authorized. The Major Medical Benefit will cover the costs for planned and authorized admissions. In the case of an emergency, the Casualty Outpatient Benefit covers pathology, radiology, medicine, and specialist consultations (subject to applicable formularies) at a Keycare Network Hospital.
Approval must be obtained for the casualty visit unless it is an emergency. In addition, only one approved casualty visit per year per beneficiary at a Network provider will be covered. The beneficiary must pay a portion of the cost of the visit. The scheme will not cover the casualty visit if approval is not obtained.
Chronic Medication Benefits
Chronic medicine can be obtained from specific pharmacies. Furthermore, chronic medicine will be covered at cost for all conditions listed on the Prescribed Minimum Benefit Chronic Disease List. The Scheme’s Designated Service Provider pharmacy provides cover with no overall limit for prescribed acute medicine. However, when discharged from the hospital after an admission, take-home medicine will be covered up to a specific limit per person per event.
The Scheme will also pay the treating physician to complete the Chronic Illness Benefit application form if the condition is approved.
WHO Outbreak Benefits
The Scheme provides a basket of care for COVID-19 and Monkeypox, subject to clinical criteria and protocols.
Screening Tests and Vaccines
Health screening checks or a flu vaccine are also covered, with cover available at one of the Scheme’s contracted providers or network pharmacies.
Maternity and Post-Birth Benefits
For expectant mothers, the Scheme offers comprehensive maternity and post-birth benefits, including specific pre-and postnatal care for up to two years after the birth and cover for the baby or toddler up to the age of two. Benefits will be paid up to 100% of the LA Health Rate from the Major Medical Benefit. They will not affect other day-to-day benefits, such as antenatal consultations, selected blood tests, ultrasound scans, prenatal screening, and GP and specialist care after birth.
Try our free Menstrual Cycle Calculator
LA Focus
Overview
Under this Option, the Major Medical Benefit covers in-hospital and major expenses, including medicine for Chronic Disease List conditions that are part of the Prescribed Minimum Benefits. Basic dentistry and in-hospital or out-of-hospital care are also covered if obtained from a provider within the LA Focus Networks. In addition, day-to-day expenses are covered by a Medical Savings Account.
Prescribed Minimum Benefits
For the full cover of the Prescribed Minimum Benefits, the individual must seek treatment at a Keycare Network Hospital located in a province with a coastline or at a LA Focus Network Hospital that is also a Keycare Network Hospital in an inland province. These hospitals are the Scheme’s designated service providers for the Prescribed Minimum Benefits on this Option. If a member is admitted by a specialist at the designated service provider hospital or a Discovery Health Network GP or a Premier A or Premier B specialist, the Scheme will cover all claims related to the authorized Prescribed Minimum Benefit procedure or treatment in full, even if other providers treating the individual are not designated service providers.
However, if the individual does not seek treatment at a designated service provider network hospital or the admitting GP or specialist is not a designated service provider, the Scheme will only cover the Prescribed Minimum Benefit claims up to the Scheme Rate. Out-of-hospital Prescribed Minimum Benefits are covered in full, subject to the use of the Scheme’s designated service providers, or at cost if there are no designated service providers.
Non-Prescribed Minimum Benefits are covered up to 100% of the Scheme Rate, subject to clinical criteria, the use of the Scheme’s designated providers, and applicable limits.
Emergency Cover
Getting you to the hospital in an emergency is covered by LA Focus. There is no cap on the total amount the Major Medical Benefit will pay for this treatment. Members can receive authorization by dialing Discovery’s 911.
GPs and Specialists In-Hospital and Out-of-Hospital
When a patient is hospitalized within the LA Focus Hospital Network, there is no limit on the number of GP and specialist visits. In addition, LA Health will cover up to one hundred percent of the LA Health Rate from the Major Medical Benefit. Furthermore, the Medical Savings Account pays for non-hospital GP and specialist appointments.
Hospitalization Cover
In private hospitals, there is no overall cap on hospitalization, surgical expenses, or intensive and high-level care costs. However, pre-authorization is required for all planned procedures. Furthermore, LA Health will cover these charges from the Major Medical Benefit up to the LA Health Rate maximum of 100 percent. All non-prescribed Minimum Benefit care must be received in a hospital in the LA Focus network. These are all hospitals in South African provinces with a coastline and hospitals in the remaining provinces. Suppose you do not utilize the services of one of these network hospitals for scheduled treatments. In that case, you will be responsible for a portion of the expenditures (a deductible).
You must utilize one of the Scheme’s Network of Designated Service Provider Day Surgery facilities when undertaking certain treatments. If you fail, the facility will require you to pay a deductible.
Chronic and Acute Medication
You have medication coverage for all diseases on the Approved Prescribed Minimum Benefit Chronic Disease List, paid in full using the Major Medical Benefit up to the LA Health Medicine Rate for listed medications. In contrast, non-formulary medications are reimbursed up to a Chronic Drug Amount. Your Medical Savings Account is used to pay for prescription and acute medicines on the preferred medicine list up to the LA Health Rate for medicines and those on the non-preferred medicine list at 90% of the medicine rate. In addition, your Medical Savings Account covers 100% of the cost of over-the-counter (schedules 0, 1, and 2) medications purchased from a pharmacy. However, a sub-limit applies when certain unscheduled supplements are purchased over the counter.
When you are discharged from the hospital following an admission, LA Health will pay 100% of the LA Health Medicine Rate for medications on the preferred medicine list and 90% of the LA Health Medicine Rate for medications not on the preferred medicine list from the funds in your Medical Savings Account. In addition, the LA Health Scheme will pay for your doctor to complete the Chronic Illness Benefit application form if your condition is accepted.
Basic Dentistry (In and Out-of-Hospital)
Suppose you see a dentist in the LA Focus Dental Network. In that case, the Major Medical Benefit covers basic dental services such as fillings, extractions, and even dentures (every four years). Suppose you utilize the services of a non-network dentist. In that case, your Medical Savings Account covers all out-of-hospital dentistry, and in-hospital care is subject to the applicable restrictions and limits.
Screening Tests and Vaccines
- A screening test (to assess your blood glucose, blood pressure, cholesterol, and body mass index) or a flu vaccination administered by one of the Scheme’s certified service providers or network pharmacies. Additionally, we cover some screenings for seniors and children.
- One pneumococcal immunization during a member’s lifetime if they are eligible.
- Subject to clinical criteria, Pap smears, mammograms, prostate-specific antigen tests, and some colorectal cancer screenings.
Furthermore, your Medical Savings Account is charged for the consultation and other connected expenses. If these are required as part of the Prescribed Minimum Benefit, the Major Medical Benefit will cover the costs. LA Health will cover these charges from the Major Medical Benefit up to the LA Health Rate maximum of 100%.
Maternity and Post-Birth Benefits
Suppose you obtain pre-authorization for your hospital admission to the LA Focus Network. In that case, there is no overall limit for hospitalizations. Furthermore, suppose the mother registers for the Scheme’s Maternity Program. In that case, LA Health will provide certain out-of-hospital benefits from the Major Medical Benefit for the mother and child. All pregnancy-related benefits will be paid from the Medical Savings Account without registration.
WHO Outbreak Benefits
The Program provides PMB benefits for treatment and care linked to the COVID-19 epidemic. Benefits are contingent on meeting clinical requirements and utilizing the Scheme’s Designated Service Providers. This covers cover for COVID-19 vaccines and treatment and care. In addition, the Scheme provides various care benefits for treatment and care associated with Monkeypox.
LA Active
Overview
This Option offers comprehensive medical cover for in-hospital and major expenses, including medication for Chronic Disease List conditions as part of the Prescribed Minimum Benefits. It also covers daily expenses from a Medical Savings Account. It offers additional cover through the Extended Day-to-day Benefit for visits to GPs, specialists, dentists, acute medicine, radiology, pathology, and optical services. Note that pre-authorization is required for all planned procedures.
Prescribed Minimum Benefits
The Prescribed Minimum Benefits are reimbursed at cost and subject to clinical criteria. If a Keycare Network Hospital admits the beneficiary, a Specialist in the Keycare hospital, a Discovery Health Network GP, or a Premier A or Premier B Specialist, all claims related to the authorized procedure or treatment will be paid in full, regardless of the providers treating the beneficiary. However, if the beneficiary does not go to a Keycare Network Hospital or the admitting GP or Specialist is not a Designated Service Provider, the Scheme will only pay the PMB claims up to the Scheme Rate.
For out-of-hospital Prescribed Minimum Benefits, full reimbursement is subject to the use of the Scheme’s Designated Service Providers or at a cost in the absence of Designated Service Providers. Non-PMB Benefits are reimbursed up to 100% of the Scheme Rate, subject to clinical criteria, the use of the Scheme’s Designated Providers, and applicable limits.
Emergency Cover
LA Active provides cover for medical emergency transport. LA Health’s Major Medical Benefit will cover the cost of this service, with no overall limit. To obtain authorization, contact Discovery 911.
GPs and Specialists In-Hospital and Out-of-Hospital
When admitted to a hospital, there is no limit on the total number of doctor and specialist visits. Furthermore, LA Health will cover up to one hundred percent of the LA Health Rate from the Major Medical Benefit. Using the Medical Savings Account or the Extended Day-to-Day Benefit, LA Health will cover GP and specialist visits outside hospitals.
Hospitalization Cover
There is no overall cap for hospitalization, theatre fees, or intensive and high care expenditures at private hospitals. However, you must seek pre-authorization from the Scheme for any planned procedures. Furthermore, LA Health will cover these charges from the Major Medical Benefit up to the LA Health Rate maximum of 100%. When you need to undergo specific treatments, you must utilize the services of Designated Service Provider Day Surgery centers. The facility will require you to pay a deductible if you don’t.
Chronic Medication Benefits
Beneficiaries have cover for approved Prescribed Minimum Benefit Chronic Disease List conditions, with the cost of medicine fully covered by the Major Medical Benefit up to the LA Health Medicine Rate for listed medicine. In addition, medicine not on the Scheme’s medicine list is covered by the Chronic Drug Amount. Prescribed acute medicine on the preferred medicine list is covered from the available funds in the Medical Savings Account or the Extended Day-to-day Benefit at 100% of the LA Health Rate for medicine.
- Medicine on the non-preferred list is covered at 90%.
- Over-the-counter (schedule 0, 1, and 2) medicine purchased at a pharmacy is covered at 100% of the cost from the available funds in the Medical Savings Account or the Extended Day-to-day Benefit, with a sub-limit applying when certain unscheduled supplements are purchased as OTCs.
Upon discharge from the hospital after an admission, take-home medicine is covered from the available funds in the Medical Savings Account or the Extended Day-to-day Benefit at 100% of the LA Health Rate for medicine on the preferred list and 90% for medicine on the non-preferred list. The Scheme also covers the cost of completing the Chronic Illness Benefit application form by the doctor if the condition is approved.
WHO Outbreak Benefits
The Major Medical Benefit provides cover for:
- Screening tests include blood glucose, blood pressure, cholesterol, and body mass index tests or flu vaccinations at designated service providers or network pharmacies. Additionally, certain screening tests for seniors and children are covered.
- One pneumococcal vaccination in a beneficiary’s lifetime for qualifying members.
- Pap smears, mammograms, prostate-specific antigen tests, and selected colorectal cancer screenings are subject to clinical criteria, along with consultations and other related costs, which are paid from the Medical Savings Account. If these are deemed part of the Prescribed Minimum Benefit, the Major Medical Benefit covers the costs.
- The Major Medical Benefit covers these costs up to 100% of the LA Health Rate.
Screening Tests and Vaccines
The scheme covers COVID-19 screening, testing, consultations, and PMB-related treatments and care, both in and out of the hospital, including vaccinations and treatment and care for long COVID-19. Additionally, the Scheme offers a basket of care benefits for treatment and care related to Monkeypox.
Maternity and Post-Birth Benefits
The cover has no overall limit when a beneficiary is admitted to the hospital with pre-authorization. In addition, certain out-of-hospital benefits for the mother and baby will be covered by the Major Medical Benefit if the mother is registered on the Scheme’s Maternity Program. However, if the mother is not registered, all pregnancy-related benefits will be covered from the available benefits in the Medical Savings Account or Extended Day-to-day Benefits.
LA Core
Overview
This Option includes a Major Medical Benefit for any hospitalization-related and major expenses. In addition, it provides cover for medications for Chronic Disease List diseases that are included in the Prescribed Minimum Benefits, as well as for a few other chronic conditions. It provides for day-to-day expenses through a Medical Savings Account and Extended Day-to-Day Benefits for general practitioners, specialists, dentists, acute medicine, radiography, pathology, and optical benefits. All scheduled operations require prior authorization.
Prescribed Minimum Benefits
The Prescribed Minimum Benefits (PMBs) are covered at cost, contingent upon meeting certain clinical criteria. When utilizing the services of a Keycare Network Hospital or a Designated Service Provider for PMBs or seeking treatment from a specialist at a Keycare hospital or a Discovery Health Network GP, or a Premier A or Premier B Specialist, the claims related to the authorized procedure or treatment will be fully covered, regardless of the provider. However, suppose treatment is received outside a Keycare Network Hospital or from a non-Designated Service Provider. In that case, the PMB claims will only be covered up to the LA Health Rate.
Out-of-hospital PMBs will be fully covered when using a Designated Service Provider or at a cost in the absence of such a provider. Non-PMB Benefits are subject to clinical criteria and will be covered up to 100% of the LA Health Rate, using the Scheme’s Network providers and any applicable limits.
Emergency Cover
LA Core provides cover for emergency medical transport services. This cover is paid from the Major Medical Benefit with no overall limit. Authorization for this service may be obtained by calling Discovery 911.
GPs and Specialists In-Hospital and Out-of-Hospital
For LA Health to fully cover Prescribed Minimum Benefit claims during hospitalization, the admitting GP or specialist must be part of the Scheme’s Network. There is no overall limit for general practitioner and specialist visits during hospitalization, and cover up to 100% of the LA Health Rate is provided by the Major Medical Benefit. The Medical Savings Account or the Extended Day-to-day Benefit covers GP and specialist visits outside the hospital.
Hospitalization Cover
Hospitalization, theatre fees, and intensive and high care costs at private hospitals are covered with no overall limit. However, pre-authorization from the Scheme is required for any planned procedures. If pre-authorization is not obtained, a deductible may apply. These costs are covered by up to 100% of the LA Health Rate from the Major Medical Benefit. In addition, designated Service Provider Day Surgery facilities must be utilized for certain procedures, and failure to do so will result in a deductible that must be paid to the facility.
Chronic Medication Benefits
Regarding medication cover, LA Core provides cover for approved conditions on the Prescribed Minimum Benefit Chronic Disease List. The cost for the listed medicine will be fully covered by the Major Medical Benefit, up to the LA Health Medicine Rate. Medicine not on the list is subject to the Chronic Drug Amount. For conditions on the Additional Disease List, medicine is covered up to an annual limit, specific to the family size, up to the Chronic Drug Amount. Acute medications on the preferred list are covered by the Medical Savings Account or the Extended Day-to-Day Benefit at 100 percent of the LA Health Rate. Medicine on the non-preferred list is paid up to 90%, according to the LA Health Rate for medicine.
Additionally, over-the-counter (schedule 0, 1, and 2) medicine purchased at a pharmacy is covered at 100% of the cost from the available funds in the Medical Savings Account or the Extended Day-to-day Benefit. However, a sub-limit applies for certain unscheduled supplements purchased over the counter. For individuals admitted to the hospital, take-home medicine will be covered from the Medical Savings Account or the Extended Day-to-day Benefit at 100% of the LA Health Rate for medicine on the preferred list and 90% for medicine on the non-preferred list after discharge.
Lastly, the Scheme will cover the cost of the Chronic Illness Benefit application form completion by the provider if the condition is approved.
WHO Outbreak Benefits
The Scheme provides Minimum Prescribed Benefits for treatment and care linked to the COVID-19 epidemic. This covers cover for COVID-19 vaccines and treatment and care. Benefits are contingent on meeting clinical requirements and utilizing the Scheme’s Designated Service Providers. In addition, the Scheme provides various care benefits for treatment and care associated with Monkeypox.
Screening Tests and Vaccines
- A screening test (to assess your blood glucose, blood pressure, cholesterol, and body mass index) or a flu vaccination administered by one of the Scheme’s certified service providers or network pharmacies. LA Health also covers additional screenings if you are over 65 years old and specific screenings for younger members.
- One pneumococcal immunization during a member’s lifetime if they are eligible.
- Pap smears, mammograms, prostate-specific antigen testing, and colorectal cancer screenings are subject to clinical criteria.
Your Medical Savings Account is charged for the consultation and other connected expenses. Suppose these are required as part of the Prescribed Minimum Benefit. In that case, the costs will be covered by the Major Medical Benefit. LA Health will cover these charges from the Major Medical Benefit up to the LA Health Rate maximum of 100 percent.
Maternity and Post-Birth Benefits
During hospitalization for pregnancy, there is no overall limit if pre-authorization is obtained. In addition, certain out-of-hospital benefits for the mother and baby are covered by the Major Medical Benefit if the mother is registered in the Scheme’s Maternity Program. If not registered, all pregnancy-related benefits will be covered from the available benefits in the Medical Savings Account or Extended Day-to-day Benefits.
LA Comprehensive
Overview
This Option includes a Major Medical Benefit for any hospitalization-related and major expenses. In addition, it covers medications for Chronic Disease List diseases that are included in the Prescribed Minimum Benefits and several other chronic conditions. It pays for a portion of day-to-day expenses from a Medical Savings Account. It provides additional coverage through the Above Threshold Benefit for most medical specialties, subject to applicable maximums. All scheduled operations require prior authorization.
Prescribed Minimum Benefits
Subject to clinical requirements, Prescribed Minimum Benefits are paid at cost. If you visit any of the following providers, LA Health covers all claims related to a specific authorized procedure or treatment, even if the provider is not a DSP:
- A Keycare Network Hospital
- The Scheme’s Designated Service Provider for Prescribed Minimum Benefits
- A Keycare hospital specialist
- A Discovery Health Network general practitioner
- A Premier A or Premier B specialist
The Scheme will only pay the Scheme Rate for PMB claims if you do not go to a Keycare Network Hospital and if your admitting GP or Specialist is not a DSP provider. Out-of-hospital If the Scheme’s Designated Service Providers are used, the entire amount of the Prescribed Minimum Benefits is paid. Otherwise, the Prescribed Minimum Benefits are paid at cost. Subject to clinical criteria, utilizing the Scheme’s Network or Preferred Providers, and applicable limits, Non-PMB Benefits are paid up to 100% of the Scheme Rate.
Emergency Cover
LA Comprehensive includes emergency medical transport cover. In addition, this service is covered by the Major Medical Benefit, with no overall limit, and members of LA Health can contact Discovery 911 for approval.
GPs and Specialists In-Hospital and Out-of-Hospital
To have claims for Prescribed Minimum Benefits fully covered during hospitalization, the treating specialist or GP must be a part of the Scheme’s Network. There is no overall limit for GP and specialist visits during hospitalization; these costs will be covered up to 100% of the LA Health Rate from the Major Medical Benefit. The Medical Savings Account or the Above Threshold Benefit will cover out-hospital GP and specialist visits.
Hospitalization Cover
No overall limit applies to hospitalization, theater fees, and costs for intensive and high care at hospitals. However, pre-authorization from the Scheme must be obtained for planned procedures. If there is any non-preauthorized treatment, a deductible amount must be paid directly to the facility. These costs will be covered by the Major Medical Benefit up to 100% of the LA Health Rate. For certain procedures, a Designated Service Provider Day Surgery facility is required. A deductible must be paid directly to the facility if not using such a facility.
Chronic Medication Benefits
The Major Medical Benefit offers cover for diseases on the Prescribed Minimum Benefit Chronic Disease List, covering listed medications in full up to the LA Health Medicine Rate. Cover for medicines not on the list (formulary) is provided up to a Chronic Drug Amount. The approved Additional Disease List conditions are covered up to a Chronic Drug Amount, with an annual limit based on the family size. The Specialized Medicine and Technology Benefit covers specific biological and high-technology medicines up to a specified amount, subject to authorization. In addition, the beneficiary might be required to fund the treatment themselves partially. Prescribed and acute medicines on the Scheme’s preferred medicine list are covered from the available funds in the Medical Savings Account or the Above Threshold Benefit, at 100% of the LA Health Medicine Rate, with other medicines covered at 90% of the rate.
Specific limits based on family size apply. Over-the-counter (schedule 0, 1, and 2) medicines purchased at a pharmacy are covered at 100% of the cost from the available funds in the Medical Savings Account, with a sub-limit applying for certain unscheduled supplements purchased as over-the-counter items. For those discharged from the hospital after an admission, take-home medicine is covered from the available funds in the Medical Savings Account or the Above Threshold Benefit, at 100% of the LA Health Medicine Rate for the preferred list and 90% for other medicines.
The Scheme also covers the cost of completing the Chronic Illness Benefit application form by the treating physician if the condition is approved.
WHO Outbreak Benefits
The Scheme provides Minimum Prescribed Benefits for COVID-19-related treatment and care. This includes cover for COVID-19 vaccinations, as well as treatment and care. Benefits are conditional on achieving clinical criteria and using the Scheme’s Designated Service Providers. Furthermore, the Scheme provides various advantages for monkeypox treatment and care.
Screening Tests and Vaccines
The Major Medical Benefit provides cover for various screening tests and vaccinations, including a screening test for:
- Blood glucose
- Blood pressure
- Cholesterol
- Body mass index
- Flu vaccination
- Specific pneumococcal vaccination
- Certain cancer screenings subject to clinical criteria
The Medical Savings Account or the Major Medical Benefit will cover the consultation and related costs per the Prescribed Minimum Benefits requirements.
Maternity and Post-Birth Benefits
The Major Medical Benefit will cover the mother and baby for maternity-related benefits if the mother is registered on the Scheme’s Maternity Program. If not registered, pregnancy-related benefits will be covered from the available Medical Savings Account or the Above Threshold Benefit.

LA Health – Advantages over Competitors
- LA Health offers cheap, well-managed medical coverage with moderate contribution increases.
- To meet various healthcare needs, the scheme provides a comprehensive range of benefits in five Benefit Options.
- In a medical emergency, the company provides life-saving medical transport to the policyholder and their family, regardless of where they are.
- The extensive hospital cover covers a wide range of procedures and treatments. As a result, the primary member of LA Health and their family may concentrate on rehabilitation rather than worrying about medical bills.
- LA Health’s cover extends to significant chronic conditions, allowing members to obtain the necessary medication and treatment.
- LA Health covers routine healthcare expenses such as doctor visits, prescribed medication, and dentistry.
- Members will receive complete cover for Prescribed Minimum Benefits if they use a Network provider, including full cover at a Network Hospital.
- LA Health also offers a Wellness Program that assists participants in living a healthier and more fulfilling existence.
- LA Health is well-known for its effective call center, which provides the greatest service and assistance. In addition, the claims process is rapid, and the website is user-friendly, allowing members to access information at their fingertips via the mobile app.
LA Health Medical Savings Account
LA Health offers four plans that have a medical savings account, including:
- ✅ LA Focus
- ✅ LA Active
- ✅ LA Core
- ✅ LA Comprehensive
LA Focus
| 👤 Member | ☑️ Main Member | ☑️ Spouse or Adult | ☑️ Child (Maximum 3) |
| 💶 MSA | R8,206 | R5,292 | R2,412 |
LA Active
| 👤 Member | ☑️ Main Member | ☑️ Spouse or Adult | ☑️ Child (Maximum 3) |
| 💶 MSA | R8,206 | R5,292 | R2,412 |
| 🔎 Extended Day-to-Day Benefit | R5,598 | R3,913 | R1,129 |
LA Core
| 👤 Member | ☑️ Main Member | ☑️ Spouse or Adult | ☑️ Child (Maximum 3) |
| 💶 MSA | R11,172 | R9,756 | R4,488 |
| 🔎 Extended Day-to-Day Benefit | R7,429 | R5,188 | R2,021 |
LA Comprehensive
| 👤 Member | ☑️ Main Member | ☑️ Spouse or Adult | ☑️ Child (Maximum 3) |
| 💶 MSA | R13,884 | R8,052 | R3,516 |
| 🔎 Extended Day-to-Day Benefit | R19,260 | R19,260 | R19,260 |
How to apply for Medical Aid with LA Health
Medical Aid Quote LA Health Medical Scheme process explained
To apply for Medical Aid through LA Health, you can:
- Call LA Health on 0860 103 933 to have an agent assist you with an application.
- Complete the online request form to have an agent call you back.
- If you already have a relationship with a LA Health broker in your region, fill out an application form and submit it through that broker.
When you submit your application, the following will occur:
- LA Health will collect and verify your information.
- LA Health will call or write to you if any information is missing.
- To complete your membership, LA Health might consult your broker regarding further needs.
Once your application is approved, LA Health will be in touch in the following ways:
- When LA Health activates your membership, the scheme will send you an SMS with your membership number.
- LA Health will also send you a new member welcome gift.
- Remember to withdraw your present medical scheme membership once you receive a formal acknowledgment from LA Health Medical Scheme that your application has been approved. Furthermore, it is illegal to simultaneously be a member of two medical schemes.
- Furthermore, you can contact your broker if you have not heard from LA Health within seven days of submitting your application.
How to Submit a Claim with LA Health
Claims can be submitted to LA Health using the following channels:
- Email – members can send copies of the claim or the electronic copy to [email protected].
- Fax – members can fax their claims to 0860 329 252.
- Post–members can send their claims to PO Box 652509, Benmore, 2010, or Postnet Suite 116, Private Bag X19, Milnerton, 7435.
- App – members can log into the mobile app and submit their claims.
- Online – members can log into their member profile on the LA Health website to submit a claim.
How to Submit a Compliment or Complaint with LA Health
Compliments
Compliments can be sent to LA Health via email, fax, post, or telephonically. There are also several review websites where compliments can be posted that other non-members and members can see.
Complaints
Before filing a formal complaint with the Council for Medical Schemes, you must pursue the internal dispute resolution procedure.
How to file a grievance
The subsequent steps are:
- Dial 0860 103 933 to speak with a service specialist at the call center. Do not forget to request a reference number.
- If the problem cannot be resolved, you can escalate the issue to the consultant’s team leader and a Client Relationship Manager.
- If the issue is not resolved, raise the question to the Scheme’s fund manager and the Principal Officer. At this level, a benefit request can be sent to the Scheme’s own medical adviser or medical advisory panel for review.
- If you are still dissatisfied, you may submit an appeal letter to the Scheme or its Medical Advisory Committee. This might be in the form of a formal letter or an email and should include information on the choice that was reversed as well as additional reasons or fresh clinical evidence.
- If the Medical Advisory Committee’s judgment is unacceptable, you may request that the Scheme’s Board of Trustees review the decision.
External Complaints Process
- After you have exhausted all internal Scheme procedures, you may file a disagreement. The Scheme will then convene its Disputes Committee to decide.
- You can file an appeal with the Council for Medical Schemes if you are dissatisfied with the decision of the Disputes Committee.
How to Switch my Medical Aid to LA Health
To switch your medical aid to LA Health, you can follow these steps:
- Research and compare different medical aid options offered by LA Health to determine the best fit for your needs.
- Gather information about your current medical aid plan, including any outstanding claims or pre-existing conditions that need to be considered.
- Contact LA Health and inform them of your intention to switch medical aid providers. They will guide you through the process and provide you with the necessary forms and documentation.
- Fill out the application form provided by LA Health, ensuring that all required information and supporting documentation are included.
- Submit the completed form to LA Health and any additional required documentation.
- Wait for LA Health to process your application and provide you with confirmation of your new membership.
- Once your membership has been confirmed, notify your previous medical aid provider to cancel your existing policy.
- It’s important to remember that switching medical aid providers may have implications on your cover, so be sure to thoroughly understand the terms and conditions of your new policy before deciding.
LA Health Customer Support
- You can contact their customer service department via phone for assistance. You may find the number on their website or by conducting a simple Google search.
- You can send an email to their customer service email address, which can be found on their website or by conducting an online search.
- You can also communicate with LA Health via its social media outlets, such as Facebook and Twitter.
- If you prefer written correspondence, you can write a letter to their mailing address, which can be discovered on their website or by conducting an online search.

LA Health vs Discovery Health vs Platinum Health – A Comparison
| 🔎 Medical Aid | 🥇 LA Health | 🥈 Discovery Health | 🥉 Platinum Health |
| 📌 Years in Operation | 50 Years | 30 Years | 22 Years |
| 👥 Average # Members | Unknown | 3.3 million | <55,000 |
| 📈 GCR Rating | – | AAA | A+ |
| 👤 Number of Employees | <50 | 13,500 | 100+ |
| 📊 Market Share | <1% | 56.7% | <5% |
| ➡️ Market Cover | South Africa | 40 Markets | South Africa |
| 💙 Customer Rating | 3.5/5 | 4.4/5 | 3/5 |
| ✒️ Number of reviews | 60+ | 20,000+ | 3,000+ |
| 📱 Mobile App | ✅ Yes | ✅ Yes | No |
| 💵 Contribution Range (ZAR) | 1,390 – 9,379 ZAR | 1,102 – 10,303 ZAR | |
| 💶 International Travel Benefit (ZAR) | 5 million ZAR | Up to 5 million ZAR | – |
| 💷 Market Capitalization | – | 86.2 billion ZAR | – |
LA Health Member Reviews
Very Satisfied.
I would like to express my sincere satisfaction with the medical scheme I have been enrolled in for the past three years. The level of customer service I have received has been unparalleled compared to my previous experiences with other medical schemes. In addition, their diligence in addressing my concerns and their commitment to meeting the needs of their clients is commendable. – Ada Gates

Excellent Support.
I appreciate their prompt response to an issue I had with my change of address, which was not accurately reflected in my statements. Despite the seemingly small nature of the issue, the customer service department took the time to explain their system updates and apologize for the inconvenience. This level of professionalism and dedication is truly remarkable. – Gregory Salinas

Comprehensive and efficient.
The cover provided by this medical scheme has been comprehensive and efficient. I have found the process of obtaining medical treatment to be seamless and stress-free. The scheme has covered all my hospital visits, doctor and specialist appointments, and prescription medicines. – Lila Gibbons

LA Health – Our Verdict
LA Health is a South African-based medical scheme providing health insurance coverage to its members. As a medical scheme, LA Health operates on a non-profit basis. In addition, LA Health is well-regulated by the Council for Medical Schemes in South Africa. Members of LA Health can expect to receive coverage for various healthcare services, including hospitalization, doctor visits, and prescribed medicines. However, the exact level of coverage provided by LA Health may vary depending on the specific plan selected by the member. One of the benefits of being a member of LA Health is that members have access to a network of healthcare providers, which can include hospitals, clinics, and other medical facilities. This network provides members with a range of options for accessing healthcare services and can help ensure that members receive the care they need when needed.
LA Health Pros and Cons
| ✅ Pros | ❎ Cons |
| There are five comprehensive plans that fit every need and budget | Some limits may apply, and there can be a lot of out-of-pocket expenses, especially on lower plans |
| LA Health is partnered with Discovery, the largest medical aid scheme in the country, providing LA Health with credibility | LA Health is only available to government employees |
LA Health Frequently Asked Questions
Can anyone in South Africa join LA Health?
Not everyone is permitted to join LA Health. The Scheme is restricted to Local Government personnel and employees linked with the sector through employment or other relevant ties.
Is LA Health part of Discovery Health?
Discovery Holdings administers the LA Health website.
Where can I find LA Health medical aid prices?
You can visit the LA Health website and view the available plans and contributions by downloading the plan brochure for 2023.
What is the LA Health contact number?
LA Health can be contacted telephonically at 0860 103 933.
Where can I view the LA Health Network Doctors List?
You can view the LA Health Network Doctors list on the official website or your plan brochure.
What is the LA Health claims contact number?
You can enquire about claims when you call 0860 103 933. Alternatively, you can view your claims and status in your members’ area or app.
What are the LA Health active benefits?
To view the comprehensive list of benefits, you can view the brochures for each plan on the LA Health website.
What is the price range of LA Health Focus?
LA Focus’ price range is R2,904 for a main member, R1,875 for an adult-dependent/spouse, and R852 per child (up to a maximum of three children).
How many providers are on the LA Health Active Hospital Network?
There are over 200 providers on the LA Health Active Hospital Network across South Africa.
How do I Downgrade my Plan with LA Health?
To downgrade your plan, navigate to the “Find a Document” section of the LA Health website or ask your payroll department to provide the relevant form. Complete the “Options change form 2023” by filling out the following sections, Member’s Details and Employer or Pension Fund Approval
How do I add a Beneficiary to LA Health?
A dependent is an individual entitled to cover under the LA Health Medical Scheme membership, of which you are the primary member. However, it is important to note that there are certain eligibility criteria for dependents. Contact LA Health directly or visit www.lahealth.co.za, where the relevant application form and supporting documentation can be found.
You might also like
Table of Contents
Free Medical Aid Quote
Our Trusted Partners
We work with leading medical aid companies in South Africa.

7 Actionable Ways to save 32% on your MEDICAL AID in 14 days.

- +27 72 7967 530
- [email protected]
- 2nd Floor, West Tower, Nelson Mandela Square, Sandton, 2196, Johannesburg, Gauteng, South Africa
🔎 Report a bug or outdated data to be updated to [email protected]
© Medicalaid.com | All rights Reserved |
Copyright 2024
Top 5 Medical Aids
Top 5 Gap Cover Plans
































