- Medical Aid
- Currently Trending
The Best Medical Aids
- Compare Plans
- Gap Cover
- Best Gap Covers
- Hospital Plans
- Currently Trending
The Best Hospital Plans
- Medical Insurance
- Pet Insurance
Engen Medical Benefit Fund
Overall, the Engen Medical Benefits Fund is a trustworthy and comprehensive medical aid plan that offers 24/7 medical emergency assistance and in-hospital treatment to up to 3 Family Members. The Engen Medical Benefits Fund starts from R2,795 ZAR. The Engen Medical Benefits Fund has a trust rating of 4.
| 🔴 The average number of members | 10,000+ |
| 🟠 Number of Markets | 1 |
| 🟡 Number of Employees | 150+ |
| 🟢 JSE Stock Symbol | BSE “ENGEN” |
| 🔵 The most recent Market Cap reported | 2.6 billion ZAR |
| 🟣 Average Customer Rating | 4 |
| 🔴 Average Number of Reviews | 100+ |
| 🟠 Market Share | <1% |
| 🟡 The number of plans offered | 1 |
| 🟢 Number of Hospitals in Network | 150+ |
| 🔵 Home care provided | ✅ Yes |
| 🟣 Mobile App | ✅ Yes |
| 🔴 Medical Claims Portal | ✅ Yes |
| 🟠 Information Hub for COVID-19 | ✅ Yes |
| 🟡 Chronic Illness Benefits | ✅ Yes |
| 🟢 Number of PMB Diagnoses | 271 |
| 🔵 Number of PMB Chronic Conditions | 26 |
| 🟣 Screening and Prevention offered | ✅ Yes |
| 🔴 Maternity Benefit | ✅ Yes |
| 🟠 Medical Aid Contribution Range | 2,795 – 5,072 ZAR |
| 🟡 Average Waiting Period | 3 – 12 months |
| 🟢 Late-joiner penalties charged | ✅ Yes |
Engen Medical Benefit Fund – Analysis of Providers’ Main Features
- ✅ Engen Medical Benefit Fund Plan Overview
- ✅ Engen Medical Benefit Fund – Advantages Over Competitors
- ✅ How to apply for Medical Aid with Engen Medical Benefit Fund
- ✅ How to Submit a Claim with Engen Medical Benefit Fund
- ✅ Engen Medical Benefit Fund Medical Savings Account
- ✅ How to Submit a Compliment or Complaint with Engen Medical Benefit Fund
- ✅ How to Switch My Medical Aid to Engen Medical Benefit Fund
- ✅ Engen Medical Benefit Fund Customer Support
- ✅ Engen Medical Benefit Fund vs Notable Competitors – A Comparison
- ✅ Engen Medical Benefits Fund Customer Reviews
- ✅ Engen Medical Benefits Fund Pros and Cons
- ✅ Our Verdict on Engen Medical Benefit Fund
- ✅ Engen Medical Benefits Fund Frequently Asked Questions
Engen Medical Benefit Fund Plan Overview
Contributions
| 💵 Income Bracket | 👤 Principal Member | 👥 Adult Dependent | 🍼 Child Dependent |
| R0 – R6,550 | R2,795 | R2,375 | R838 |
| R6,551 – R18,960 | R4,192 | R3,353 | R1,195 |
| R18,961> | R5,072 | R4,235 | R1,446 |
In-hospital Cover
| 🟥 Hospital Admission | – |
| 🟧 Hospital stays in a general, labor, high care, intensive care unit, or theatre, including dressing materials and equipment. | Covered up to 100% of the fund rate. Unlimited cover. Pre-authorization required. Admission must be to a KeyCare Network Hospital. |
| 🟨 Psychiatric Hospitalisation | Covered up to 100% of the fund rate. Limited to 21 days per beneficiary per year or 15 outpatient psychotherapy consultations. Admission must be to a KeyCare Network Hospital. |
| 🟩 Day Clinic or Theatre Admission | Covered up to 100% of the fund rate. Unlimited cover. Admission must be to a KeyCare Network Hospital. |
| 🟦 In-Hospital Treatment | – |
| 🟪 Arthroplasty, colorectal surgery, coronary artery bypass graft, radical prostatectomy, and mastectomy pre-op evaluation. | Covered up to 100% of the fund rate. Unlimited cover. Pre-authorization required. |
| 🟥 Surgery, physiotherapy, ward and theatre medication, and blood transfusions | Covered up to 100% of the fund rate. Unlimited cover. Pre-authorization required. |
| 🟧 Anesthetics used in the theatre | Covered up to 100% of the fund rate. Unlimited cover. Pre-authorization required. |
| 🟨 Pathology | Covered up to 100% of the fund rate. Unlimited cover. Pre-authorization required. |
| 🟩 Endoscopic Investigations | Covered up to 100% of the fund rate. Unlimited cover. Pre-authorization required. |
| 🟦 To-Take-Out (TTO) Medicine | Covered up to 100% of the fund rate. 7 days’ supply. |
| 🟪 Organ transplants—preparation, harvesting, transportation, and immunosuppression. | Covered up to 100% of the fund rate. Limited to R505,000 per family per year, subject to PMBs. |
| 🟥 Spinal care program – In- and out-of-hospital spinal care and surgery for clinically appropriate procedures like Lumbar Fusion, Cervical Fusion, Laminectomy, and Laminotomy. | Covered up to 100% of the fund rate. Unlimited Cover Subject to pre-authorization, treatment guidelines, clinical criteria, and a basket of care. Limited to one hospital procedure per year. Includes basket-of-care outpatient conservative treatment |
| 🟧 Spinal prostheses or devices | Covered up to 100% of the fund rate if treated in a DSP. Non-DSP providers – limited to R26,250 for one level and R52,500 for two levels. |
| 🟨 Renal dialysis | Covered up to 100% of the fund rate. Unlimited cover provided. |
| 🟩 Drug and Alcohol Rehabilitation | Covered up to 100% of the fund rate. Limited to PMBs. Limited to 3 days in-hospital for detoxification and 21 days for rehabilitation. Subject to using a DSP such as SANCA, RAMOT, or Nishtara Lodge. Pre-authorization is required. |
| 🟦 Internal Prostheses | Covered up to 100% of the fund rate. Multiple external and internal prostheses are limited to R101,200 per beneficiary per year, and the sub-limits are listed. The following sub-limits apply per prostheses type: Hip or Knee replacement – R30,900 Shoulder replacement – R45,550 Artificial Limbs below the knee – R26,900 Artificial Limbs above the knee – R45,300 Artificial Eyes – R26,900 Finger joint Prostheses – R6,700 Pacemakers – Unlimited if supplied by a DSP. Internal Cardiac Defibrillator – Unlimited if supplied by a DSP. Cardiac Valves – R42,900 each Aortic Aneurysm Repair Graft – R179,200 Cardiac Stents are unlimited if using a DSP. Drug-eluting stent – R14,520 Bare metal stent – R10,330 |
| 🟪 Dentistry | – |
| 🟥 Maxillo-facial Surgery | Covered up to 100% of the fund rate. Unlimited cover. Pre-authorization required. |
| 🟧 Basic Dental Trauma Procedures for sudden and unexpected impact injuries to teeth and the mouth that result in partial or complete tooth loss and require urgent in- or out-of-hospital care. | Covered up to 100% of the fund rate. Limited to R61,500 per beneficiary per year. |
| 🟨 Hospital Admissions | – |
| 🟩 Voluntary admission: Hospital stay, consultations, surgery, treatment, medication, physiotherapy, anesthetics, etc. | Covered up to 100% of the fund rate. Unlimited cover. Pre-authorization required. Admission must be to a KeyCare Network Hospital. |
| 🟦 Emergency/involuntary non-DSP admission | Covered up to 100% of the fund rate but subject to PMBs. Unlimited cover. Pre-authorization required. Admission must be to a KeyCare Network Hospital. |
| 🟪 Day Surgery | – |
| 🟥 Provided in a Day Surgery Network facility and applicable to a defined list of procedures. | Covered up to 100% of the fund rate. If a non-DSP is involuntarily used, there is an R6,300 deductible per admission. Unlimited cover. Pre-authorization required. Member must use the day surgery network. |
| 🟧 Motor Vehicle Accidents and Third-party Claims | – |
| 🟨 The member must sign an accident injury form and report to receive payment. | Covered up to 100% of the fund rate. Unlimited cover. Admission must be to a KeyCare Network Hospital. |
| 🟩 Post-operative therapy and rehabilitation | Covered up to 100% of the fund rate. Post-operative physiotherapy, occupational, and speech therapy for the same condition as hospitalization for six weeks. Pre-authorization required |
| 🟦 Chronic Medication | – |
| 🟪 PMB CDL covers chronic medication for Chronic Illness Benefit members and dependents. | Covered up to 100% of the fund rate. Unlimited cover. Subject to MMAP, chronic medicine list, and PMBs. |
| 🟥 Non-PMB Chronic Medication | Covers long-term medication and injections. Limited to R15,700 per individual and R30,600 per family per year. |
| 🟧 Specialty Medication | Covered up to 100% of the fund rate. Limited to R178,400 per family per year. |
| 🟨 Outpatient Procedures and Emergency Visits | – |
| 🟩 Outpatient or casualty procedure after hospital admission (within 48 hours). | Covered up to 100% of the fund rate. Unlimited cover. Pre-authorization required. |
| 🟦 Emergency outpatient or casualty procedures, medication, and treatment | Covered up to 100% of the fund rate. Unlimited cover. |
| 🟪 Specialist and GP Consultations and Treatment Out-of-Hospital | – |
| 🟥 Consultations, material, and visits | Covered up to 100% of the DSP or fund rate. Limited to R3,200 for the main member only and up to R7,800 for the main +4> dependents. |
| 🟧 Procedures performed in the doctor’s rooms | Covered up to 100% of the fund rate. Unlimited cover. |
| 🟨 Diabetes or cardio care program | Covered up to 100% of the fund rate. Non-PMB GP services are covered in a defined basked of care. |
| 🟩 Mental health care program | Covered up to 100% of the fund rate. Non-PMB GP services are covered in a defined basked of care. |
| 🟦 Oncology | – |
| 🟪 Chemotherapy, drugs, radiation, PET scans, and other oncology treatments | Covered up to 100% of the fund rate. Subject to the Prescribed Minimum Benefit, beneficiaries have an R250,000 annual threshold. Non-PMB claims are paid 80% of the Fund Rate after the threshold. |
| 🟥 Stoma and oxygen products | Covered up to 100% of the fund rate. Limited to R30,000 per family per year. |
| 🟧 Advanced Illness Benefit | – |
| 🟨 Offers comprehensive out-of-hospital palliative care for terminally ill patients. Psychosocial support, hospice care, oxygen, pain control, and home-based nursing | Covered up to 100% of the fund rate. Unlimited cover. |
| 🟩 Advanced Illness Member Support Program | – |
| 🟦 Advanced illness patients need help managing their symptoms and understanding their healthcare needs. | Covered up to 100% of the fund rate. Unlimited cover subject to a basket of care. |
| 🟪 Radiology and Pathology | – |
| 🟥 X-rays, pathology, and radiology Includes doctor-performed endoscopies | Covered up to 100% of the fund rate. Unlimited cover. |
| 🟧 Specialized Radiology | – |
| 🟨 MRI and CT scans | Covered up to 100% of the fund rate. Limited to 2 scans per beneficiary per year in and out-of-hospital. Subject to PMBs. |
| 🟩 Clinical and Medical Technologies | – |
| 🟦 Clinical and medical technologists: services, materials, and equipment | Covered up to 100% of the fund rate. Unlimited cover. |
| 🟪 Maternity | – |
| 🟥 Hospitalization, water births, and midwife pre-and post-natal care. Covers face-to-face, tele, and virtual consultations as needed. | Covered up to 100% of the fund rate. Unlimited cover. |
| 🟧 Midwife, GP, or gynecologist prenatal visits. | Covered up to 100% of the fund rate. Limited to 12 visits per pregnancy per year. |
| 🟨 Postpartum midwife, GP, or gynecologist consultation | Covered up to 100% of the fund rate. Limited to 1 visit per pregnancy. |
| 🟩 Counseling or psychotherapy for post-natal mental health | Covered up to 100% of the fund rate. Limited to 2 sessions per pregnancy. |
| 🟦 The registered nurse or lactation specialist consultation | Covered up to 100% of the fund rate. Limited to 1 consultation per pregnancy. |
| 🟪 GP, pediatrician, or ENT visits for registered under-2-year-olds | Covered up to 100% of the fund rate. Limited to 2 visits per child <2 years. |
| 🟥 Ante-natal ultrasound examinations | Covered up to 100% of the fund rate. Limited to 2 prenatal exams. 3D and 4D ultrasound scans are charged at 2D scan rates. |
| 🟧 Antenatal classes (in- and out-of-hospital) or registered nurse pre- and post-natal consultations | Covered up to 100% of the fund rate. Limited to 5 classes per confinement. |
| 🟨 Nutrition assessment with a dietitian after the delivery | Covered up to 100% of the fund rate. Limited to 1 assessment per confinement. |
| 🟩 Pathology | Covered up to 100% of the fund rate. Restricted to benefits in a defined basked of pregnancy-related pathology. |
| 🟦 Genetic or chromosome screenings | Covered up to 100% of the fund rate. Limited to one of the following tests: Nuchal Translucency Test Non-invasive Prenatal Test (NIPT) T21 Chromosome test |
| 🟪 Pregnancy-related External Medical Items (registered essential devices like breast pumps or nebulizers) | Covered up to 100% of the fund rate. Limited to R5,700 per pregnancy. |
| 🟥 Chronic Appliances | – |
| 🟧 Oxygen therapy, including products, cylinders, ventilation, and stoma supplies | Covered up to 100% of the fund rate. Limited to R30,000 per family per year. |
| 🟨 Medical and Surgical Appliances | – |
| 🟩 Medical and surgical appliances, including wheelchairs and hearing aids. | Covered up to 100% of the fund rate. Limited to R30,000 per family per year. |
| 🟦 Second hearing aid | Limited to R14,700 per family per year. |
| 🟪 Bluetooth-enabled glucose monitoring devices | Covered up to 100% of the fund rate. Limited to one device per beneficiary per year. |
| 🟥 Continuous glucose monitoring sensors | Covered up to 100% of the fund rate. Sensors are limited to R1,660 per beneficiary per year. The transmitter/receiver is limited to 1 device per beneficiary per year up to R4,600 per transmitter. |
| 🟧 Dentistry | – |
| 🟨 Basic Dentistry | Covered up to 100% of the fund rate. Limited to R4,500 per main member and up to R9,900 for the main member +4> dependents. |
| 🟩 Specialized Dentistry includes Inlays, crowns, bridges, study models, metal-base dentures and their repair, oral medicine, periodontics, orthodontics, prosthodontics, and Osseo-integrated implantology. | Covered up to 100% of the fund rate. Limited to R10,000 per main member and up to R22,300 for the main member +4> dependents. |
| 🟦 Blood Transfusions | – |
| 🟪 Blood Transfusions | Covered up to 100% of the fund rate. Unlimited cover. |
| 🟥 Ambulance and Emergency Services | – |
| 🟧 Air and road emergency medical transport or interhospital transfers | Covered up to 100% of the fund rate. Unlimited cover when using ER24. |
| 🟨 Step-down and Rehabilitation Facilities | – |
| 🟩 Sub-acute physical rehab centers without hospitalization. | Covered up to 100% of the fund rate. Managed Care Regulations will apply. Unlimited cover. |
| 🟦 Home-based care | – |
| 🟪 Includes devices for home monitoring (based on clinical need) for qualifying members instead of hospitalization, early discharge, continued care after discharge, or home-based readmission prevention. | Covered up to 100% of the fund rate. Unlimited cover. |
| 🟥 Private Nursing and Registered Private Nurse Practitioners | – |
| 🟧 Private nursing and RNs, including hospice and frail care | Covered up to 100% of the fund rate. Limited to R30,600 per family per year. |
| 🟨 HIV Management | – |
| 🟩 HIV treatment | Covered up to 100% of the fund rate. Unlimited cover but subject to formularies. |
Screening and prevention
| 🔴 Pharmacy Screening Benefits | – |
| 🟠 Pharmacy Screening Benefits for Adults | Covered up to 100% of the fund rate. Covers one or all of the following (if done simultaneously in one visit): Blood Glucose test Blood Pressure test Total Serum Cholesterol Test BMI |
| 🟡 Pharmacy Screening Benefit for seniors | Covered up to 100% of the fund rate. Screening tests for members 65>. At-risk beneficiaries receive one annual comprehensive screening at a Network GP. |
| 🟢 Pharmacy Screening Benefit for Children | Covered up to 100% of the fund rate. One or all of these tests (if done simultaneously) per 2-to-18-year-old per year: Basic hearing and dental screening. Body mass index for children 2 – 18, including counseling. Head circumference for children 2 – 5. Blood pressure for children 3 – 18. Health and milestone tracking for 2–18-year-olds. |
| 🔵 Other Screening Benefits | – |
| 🟣 Pap Smear | Covered up to 100% of the fund rate. Screening test every 3 years. HIV-positive or Pap smear-abnormal beneficiaries receive one screening test per year. Clinical entry and authorization are required. |
| 🔴 Mammogram | Two-year mammograms with ultrasounds. Annual mammogram or MRI breast screening and one-time BRCA testing for at-risk beneficiaries. Clinical entry and authorization are required. |
| 🟠 Fecal Occult Blood Test | Limited to 1 of the listed tests paid every 2 years for beneficiaries 45–75. Limited to 1 colonoscopy per year for at-risk or positive test results. Clinically admissible |
| 🟡 Trauma Recovery | – |
| 🟢 Trauma-specific cover. | Covered up to 100% of the fund rate. The benefit is paid until the end of the year after the trauma. The General Rules for Designated Service Providers and clinical entry criteria determine benefits. Allied and therapeutic healthcare services are limited to R22,300 and R42,850, depending on how many members are on the plan. Prescribed medicine is limited between R6,200 to R13,500, depending on the number of members on the plan. |
| 🔵 Counseling sessions with a psychologist, registered counselor, or social worker | Covered up to 100% of the fund rate. Limited to 6 sessions per beneficiary. |
✅ World Health Organisation (WHO) Outbreak Benefit
- Global Who-recognised disease outbreaks out-of-hospital management and supportive treatment.
- Subject to Prescribed Minimum Benefits, the Fund’s DSP/Preferred providers’ services, protocols, and the condition and treatment meeting the Fund’s entry criteria and guidelines.
✅ COVID-19
- 100% of the DSP agreed on the rate for PMB or Fund Rate for non-DSP or non-PMB.
- Unlimited cover.
✅ MonkeyPox
- 100% of the DSP agreed on the rate for PMB or Fund Rate for non-DSP or non-PMB.
- MonkeyPox benefits are subject to a Fund-determined basket of care.
Day-to-Day Cover
| 🟥 Consultations and non-surgical procedures | – |
| 🟧 General practitioners, medical specialists, homeopaths, naturopaths, and registered private nurse practitioners, including outpatient fees. Face-to-face, telephonic, and virtual consultations | Covers 100% of GP and Specialist Fund Rates. Other providers receive a 100% Fund Rate. Limits range from R3,200 to R7,800 depending on the number of dependents on the plan. |
| 🟨 Acute, homeopathic, and naturopathic medicine | – |
| 🟩 Acute, homeopathic, and naturopathic medicine | Covers up to 100% of the MMAP from MSA, then from Primary Care (day-to-day) limit. Limits range from R6,200 to R13,500 depending on the number of dependents on the plan. |
| 🟦 Self-medication and Over-the-counter (OTC) medication | Covers up to 100% of the cost. Limited to R330 per prescription per beneficiary per day. |
| 🟪 Optometry | – |
| 🟥 Eye tests and tonometry tests | Covered up to 100% of the fund rate from the MSA. Limited to one eye exam per beneficiary per year. |
| 🟧 Glasses, lenses, frames, and contacts Covers hardening, tinting, reflective lens coating, and refractive eye surgery. | Covered up to 100% of the fund rates. Limited to R5,500 per single member and R11,200 per family, including R1,800 for the frame. |
| 🟨 Paramedical Services | – |
| 🟩 Acupuncture | Covered up to 80% of the fund rate. Limited to R2,000 per family per year. |
| 🟦 Chiropractor | Covered up to 80% of the fund rate. Limited to R3,700 per family per year. |
| 🟪 Dietician | Covered up to 80% of the fund rate. Limited to R1,300 per family per year. |
| 🟥 Non-surgical prostheses | Covered up to 80% of the cost. Limited to R3,600 per family per year. |
| 🟧 Audiology and speech therapy | Covered up to 80% of the fund rate. Limited to R3,600 per family per year. |
| 🟨 Occupational Therapy | Covered up to 80% of the fund rate. Limited to R3,600 per family per year. |
| 🟩 Physiotherapy and Biokinetics | Covered up to 80% of the fund rate. Limited to R3,600 per family per year. |
| 🟦 Private nursing and private nurse practitioners | Covered up to 80% of the fund rate. Limited to R30,600 per family per year. |
| 🟪 Podiatry or Chiropody | Covered up to 80% of the fund rate. Limited to R2,400 per family per year. |
| 🟥 Clinical Psychology | Covered up to 80% of the fund rate. Limited to R10,000 per family per year. |
| 🟧 Preventative Care | – |
| 🟨 Smoking cessation | Covered up to 100% of the fund rate. Limited to R800 per beneficiary per month. |
| 🟩 Human Papilloma Virus (HPV) Screening | Covered up to 100% of the fund rate. Limited to R630 per beneficiary per year. |
| 🟦 Implantation of Contraceptive Devices (UID) | Covered up to 100% of the fund rate. Limited to the MSA. |
Engen Medical Benefit Fund – Advantages Over Competitors
The advantages of choosing the Engen Medical Benefit Include:
- ✅ A wide range of comprehensive medical scheme benefits that cover different needs and a plan structure that suits most budgets.
- ✅ Competitive rates and affordability, with transparent pricing structures.
- ✅ Unlimited cover for in-hospital and day-to-day medical expenses, with options for co-payments and deductibles.
- ✅ Cover for chronic medication and specialized treatments, such as oncology and renal dialysis.
- ✅ Access to an extensive network of healthcare providers, including hospitals, doctors, and pharmacies.
- ✅ A dedicated wellness program that offers preventative care and lifestyle support.
- ✅ Personalised service, with a team of experienced medical scheme administrators and consultants to assist with inquiries and claims.
- ✅ Convenient digital platforms, such as the Engen Med app, for easy access to information and services.
- ✅ Flexible payment options, including debit orders and payroll deductions.
Collaboration with reputable partners, such as Discovery Health and Momentum Health, to enhance services and benefits.

How to apply for Medical Aid with Engen Medical Benefit Fund
Engen Medical Benefit Fund membership is restricted to full-time, permanent Engen employees and participating employers. To apply for Medical Aid through Engen Medical Benefit Fund, you must:
- Click the “Join Now” button on the Engen Medical Benefit Fund website at https://www.engenmed.co.za/.
- Include your full name, identification number, email address, and phone number.
- Select the medical plan option that meets your needs and budget the best. The Engen Medical Benefit Fund provides various options, such as a traditional medical plan, a network option, and a hospital plan.
- Engen employees can select the most convenient payment method, such as a monthly debit order or payroll deduction.
Submit your application and await the Engen Medical Benefit Fund’s response. Once your application has been processed and approved, you will be notified.

How to Submit a Claim with Engen Medical Benefit Fund
To be eligible for benefits, a claim must be submitted to the Fund by the end of the fourth month following the month the service was performed. If you believe a claim was rejected in error, you have sixty days to report the error and resubmit the claim; otherwise, the claim will be deemed stale. Follow these steps to submit a claim to Engen Medical Benefit Fund:
- Obtain the required documentation, including your medical invoice, completed claim form, and any additional supporting documents required by Engen Medical Benefit Fund.
- Ensure that the selected medical plan option covers the medical service or treatment you receive.
- Submit your claim form and supporting documentation to Engen Medical Benefit Fund within the time frame specified. This can be accomplished via mail, email, or the Engen Med app.
- Wait for Engen Medical Benefit Fund’s response. They will evaluate your claim and provide you with feedback.
If your claim is approved, Engen Medical Benefit Fund will pay the healthcare provider directly or reimburse you if you have already paid the provider.
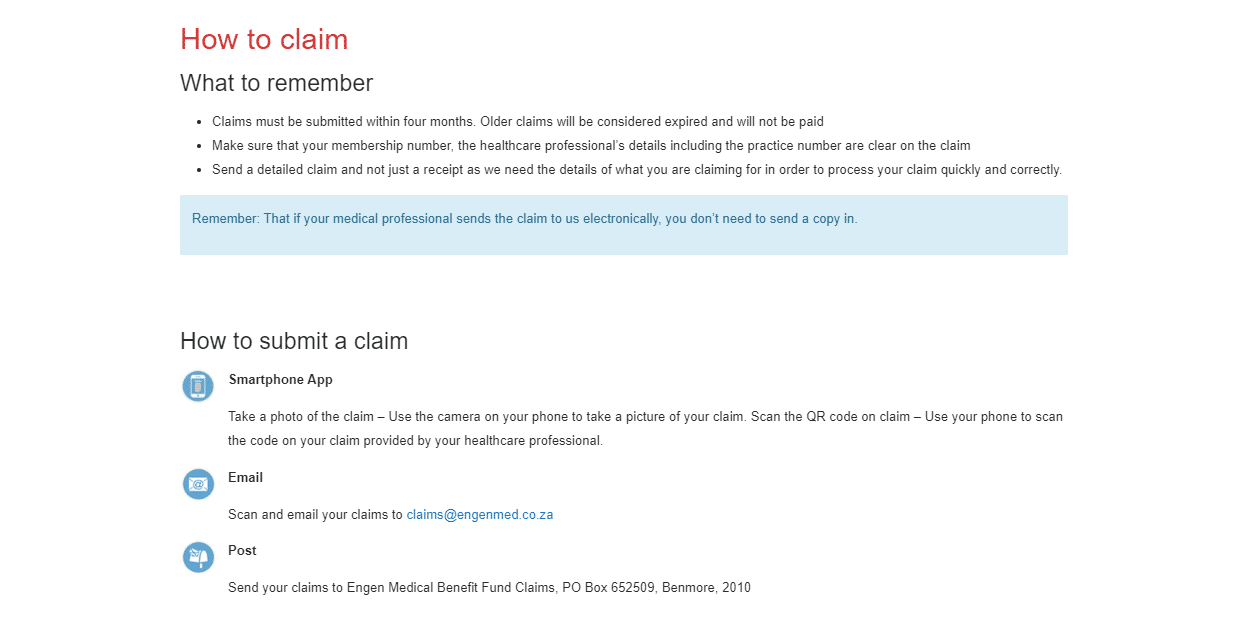
Engen Medical Benefit Fund Medical Savings Account
Engen Medical Benefit Fund offers a Medical Savings Account (MSA) whereby members contribute 10% of their monthly contribution into this account. For instance, if your monthly contribution is R1 000, R100 (10% of R1 000) will be allocated to the MSA and R900 towards the Fund’s risk pool. A positive balance in the MSA at month-end attracts interest.
If you resign from the Fund, any positive MSA balance will be kept for four months to settle any claims incurred before your resignation.
Any remaining balance will be paid out to you in the fifth month after your resignation or transferred to your new medical scheme, provided they have an MSA benefit. However, on termination of membership, any positive MSA balance may be used to offset any debt owed to the Fund, including outstanding contributions.
The Fund advances 12 months of MSA to members effective 1 January each year. Overdrawn MSA will be deducted from the outstanding balance when a member resigns from the Fund.
Payments from the MSA will be made at 100% of the Fund rate, subject to the availability of funds on the claim processing date. For example, suppose MSA is available at the end of the financial year (31 December). In that case, the positive balance will be carried over to the next year.
In the event of a member’s death, the MSA balance due will be transferred to their dependents if they decide to continue with Fund membership. Alternatively, the balance will be paid into the estate if there are no dependents.
POLL: Best Hospital Plans with a Savings option
How to Submit a Compliment or Complaint with Engen Medical Benefit Fund
Here are the steps to follow for the Engen Medical Benefit Fund complaints procedure:
- ✅ Contact Engen Medical Benefit Fund’s Client Service Department during office hours and try to resolve your query.
- ✅ If the result is unsatisfactory, ask to escalate to more senior resources in the Administrator’s Service Team, such as a Team Leader or Manager.
- ✅ If you are still unsatisfied, send a written request to the Principal Officer of the Fund to attend to the matter. The query should be addressed to the Principal Officer and sent to the normal email or postal addresses of the Fund.
- ✅ If the outcome of the escalation process to the Principal Officer is not accepted, complain in writing for the attention of the Engen Medical Benefit Fund’s Disputes Committee. The details for the Disputes Committee are available on the Engen Medical Benefit Fund website. The Disputes Committee will meet to decide on the complaint or dispute and determine the procedure to follow. You have the right to be heard at these proceedings, either in person or through a representative.
If still dissatisfied after the Disputes Committee’s decision, the appeal can be further escalated by approaching the Council for Medical Schemes for resolution.

How to Switch My Medical Aid to Engen Medical Benefit Fund
Follow these steps to switch your medical insurance to Engen Medical Benefit Fund:
- ✅ Research to compare the options and benefits of the Engen Medical Benefit Fund with your current medical aid. Determine whether the offerings of Engen Medical Benefit Fund meet your healthcare needs and budget.
- ✅ Contact Engen Medical Benefit Fund’s customer service department for additional details on their medical scheme options, benefits, and pricing.
- ✅ Obtain and complete the application form for the Engen Medical Benefit Fund medical plan option that best meets your needs and budget. You can access the application form on their website or by contacting their customer service department.
- ✅ Ensure you include all required information on the application form, including your personal and contact information, previous medical aid information, and any chronic or pre-existing medical conditions.
- ✅ Submit the completed application via email, mail, or the Engen Med app to Engen Medical Benefit Fund.
- ✅ Wait for Engen Medical Benefit Fund’s response. They will evaluate your application and provide you with feedback.
- ✅ If your application is approved, you must complete any outstanding administrative tasks, such as signing a membership agreement, paying your first premium, and submitting additional information or documentation.
Once all administrative tasks have been completed, Engen Medical Benefit Fund will take over your medical cover.

Engen Medical Benefit Fund Customer Support
Engen Medical Benefit Fund offers customer support through various channels, including:
- ✅ You can contact the Engen Medical Benefit Fund’s customer service team via phone on their toll-free number at 0800 001 615. The lines are open Monday to Friday from 8 am to 5 pm.
- ✅ Email: You can email Engen Medical Benefit Fund’s customer service team at [email protected] for any queries or support.
You can use the Engen Med App to access your medical aid information and services and contact the customer service team.
Engen Medical Benefit Fund vs Notable Competitors – A Comparison
| 🔎 Medical Health Plan | 🥇 Engen Medical Benefit Fund | 🥈 Momentum Medical Scheme | 🥉 Genesis Medical Scheme |
| 📌 Years in Operation | 26 years | 57 Years | 28 years |
| 📍 Average # Members | 10,000+ | 293,000 | 70,000+ |
| 📉 GCR Rating | n/a | AA | n/a |
| 📈 Number of Employees | 150+ | 500 – 1,000 | 100 – 500 |
| 📊 Market Share | <1% | 20% | <1% |
| ➡️ Market Cover | South Africa | South Africa | South Africa |
| ❤️ Customer Rating | 4 | 4.5 | 3.7/5 |
| ☑️ Number of reviews | 100+ | 2,000+ | 100+ |
| 📱 Mobile App | ✅ Yes | ✅ Yes | ✅ Yes |
| 💴 Contribution Range (ZAR) | 2,795 – 5,072 ZAR | 541 – 13,573 ZAR | R1,530 – R3,000 |
| 💵 International Travel Benefit (ZAR) | No | Up to 9.01M ZAR | No |
| 💷 Market Capitalisation | 2.6 billion ZAR | n/a | n/a |

Engen Medical Benefits Fund Customer Reviews
Very Happy.
I express my gratitude for the prompt resolution of my queries, particularly given my advanced age of 85 and frequent need for payment certifications. – Bianca Davidson
Great Service.
As a parent of a child with trisomy 13, we incurred significant medical expenses. Fortunately, Engen Medical Benefits Fund was available to settle our claims, with minimal claim rejections or co-payments required. – Zander van Staden
Exceptional Service.
I commend the Engen Medical Benefits Fund team for their exceptional service. My recent claim and approval process was completed efficiently and with minimal inconvenience. Many thanks for your wonderful service. – Susan Vermeulen

Engen Medical Benefits Fund Pros and Cons
| ✅ Pros | ❎ Cons |
| Comprehensive benefits, including unlimited hospital cover | Pre-authorization is required for certain medical procedures and treatments |
| Medical Savings Account (MSA) feature for managing day-to-day medical expenses | Co-payments are required for certain treatments |
| Range of wellness and preventative care benefits such as screenings, vaccinations, and health assessments | Premiums may be higher compared to other medical aid schemes |
| Cover for emergency medical services, trauma and accident benefits, and certain medical procedures such as organ transplants | It may not cover all elective procedures |
| Wellness program offering health assessments, screenings, and vaccinations | Restricted medical aid – only available to Engen employees and their dependents |
Our Verdict on Engen Medical Benefit Fund
Engen Medical Benefits Fund is a medical aid scheme in South Africa administered by Discovery Health. Our research shows that the scheme offers a variety of options to choose from, with different levels of benefits to cater to different needs and budgets.
One standout feature of the scheme is the Medical Savings Account (MSA), where 10% of your total monthly contribution is allocated to the MSA. This can benefit those who prefer to manage their day-to-day medical expenses.
Engen Medical Benefits Fund Frequently Asked Questions
What is the Medical Savings Account (MSA) feature offered by Engen Medical Benefits Fund?
The MSA is a portion of your monthly contribution allocated to a savings account, which you can use to pay for day-to-day medical expenses.
Does Engen Medical Benefits Fund cover chronic medicine?
Yes, the scheme offers comprehensive cover for chronic medicine, subject to certain conditions and requirements.
What emergency medical services and trauma benefits are covered by the Engen Medical Benefits Fund?
The scheme covers medical and trauma benefits, including ambulance services, emergency room visits, and hospitalization.
How do I know if the Engen Medical Benefits Fund covers a specific provider?
You can check the provider network list on the scheme’s website or contact their customer service team to confirm.
What wellness and preventative care benefits are covered by Engen Medical Benefits Fund?
The scheme offers a range of wellness and preventative care benefits, including health assessments, screenings, and vaccinations.
How much do Engen Medical Benefit Fund premiums cost?
The cost of premiums starts from R2,795 for the main member, R2,375 per adult, and R838 per child dependent.
Are co-payments required for certain medical procedures and treatments?
Yes, some procedures and treatments may require co-payments, which vary depending on the specific plan and cover options the member selects.
Do I need pre-authorization for medical procedures and treatments?
Yes, certain medical procedures and treatments may require pre-authorization, which can be obtained by contacting the scheme’s customer service team.
What maternity and child health coverage is offered by Engen Medical Benefits Fund?
The scheme offers cover for prenatal care, childbirth, and child health services, subject to certain conditions and requirements.
Does Engen Medical Benefit Fund offer mental health benefits and services?
Yes, the scheme provides cover for mental health services, subject to certain conditions and requirements.
How do I Downgrade My Plan with Engen Medical Benefits Fund?
Engen Medical Benefits Fund only offers one plan option. Therefore, a downgrade is not available.
How do I add a Beneficiary to Engen Medical Benefits Fund?
If you want to add a child or adult dependent, you can log into your Engen Medical Benefits Fund profile or contact customer support.
You might also like
Table of Contents
Free Medical Aid Quote
Our Trusted Partners
We work with leading medical aid companies in South Africa.

7 Actionable Ways to save 32% on your MEDICAL AID in 14 days.

- +27 72 7967 530
- [email protected]
- 2nd Floor, West Tower, Nelson Mandela Square, Sandton, 2196, Johannesburg, Gauteng, South Africa
🔎 Report a bug or outdated data to be updated to [email protected]
© Medicalaid.com | All rights Reserved |
Copyright 2024
Top 5 Medical Aids
Top 5 Gap Cover Plans
































